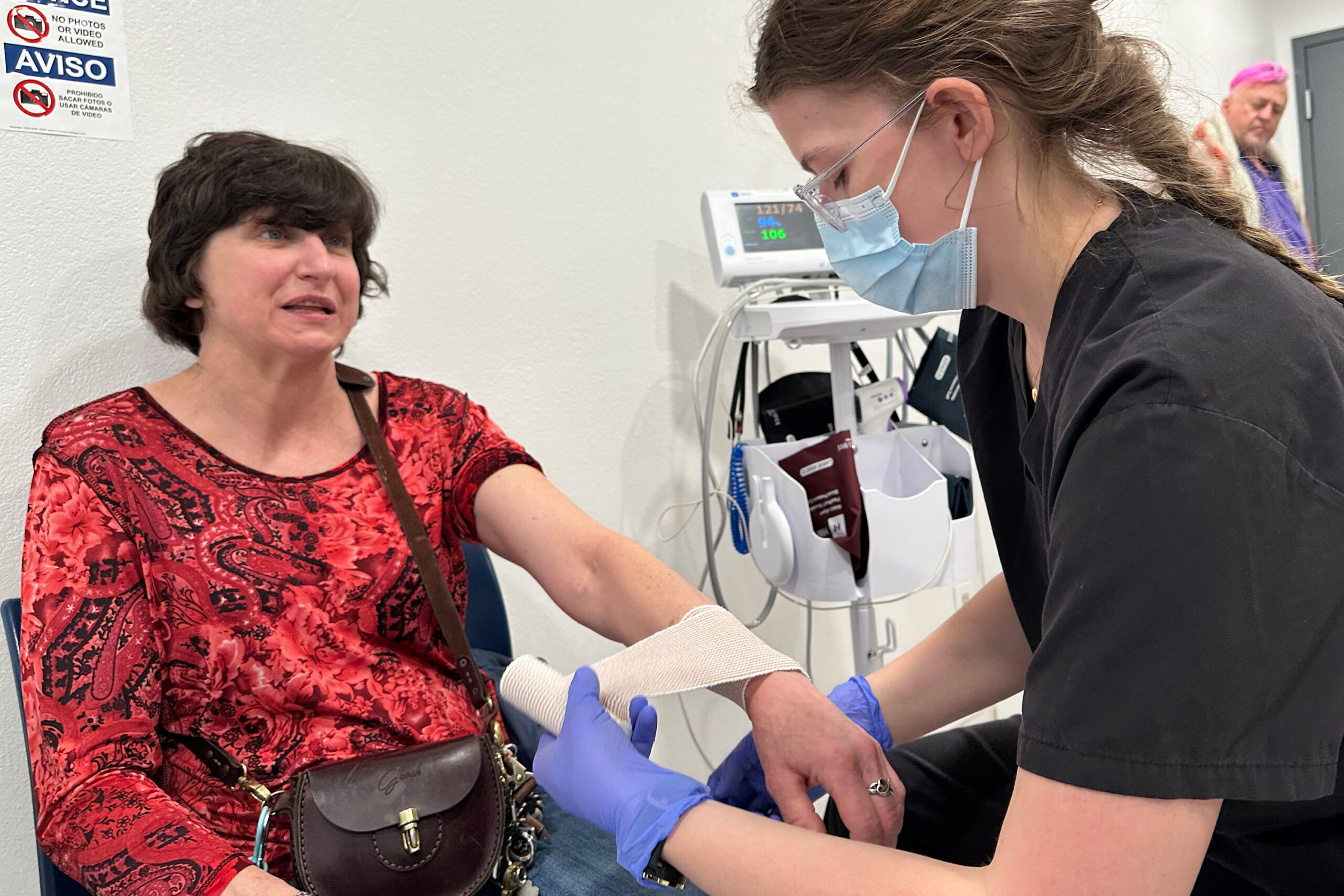
"For seniors experiencing homelessness, traditional shelters are often ill-equipped to handle their unique medical and mobility challenges. The MVP shelter in Sandy, Utah, is redefining elder homelessness support by integrating on-site medical care, accessible facilities, and specialized case management, offering a pathway to stability and dignity."
Nestled in Sandy, Utah, a suburb of Salt Lake City, an unassuming two-story brick building has been transformed into a vital sanctuary for the community’s most vulnerable seniors. This former hotel now operates as the Medically Vulnerable People (MVP) shelter, a groundbreaking facility dedicated to providing a safe and supportive environment for individuals aged 62 and older, as well as younger adults grappling with chronic health conditions. Unlike conventional homeless shelters, the MVP facility is meticulously designed to address the specific needs of its aging clientele, offering features such as accessible shared rooms and private bathrooms, a crucial amenity for seniors managing incontinence.
The escalating crisis of senior homelessness is a growing concern nationwide. Dennis Culhane, a researcher at the University of Pennsylvania, highlights that older adults are the fastest-growing demographic experiencing homelessness. This trend is twofold: individuals who have faced chronic homelessness for years are aging, and a significant number of seniors are finding themselves without housing for the first time in their lives, often due to financial instability, medical crises, or the loss of affordable housing options. Traditional shelters, with their often-basic facilities like bunk beds and shared bathrooms, present significant hurdles for older adults. Challenges such as navigating bunk beds, managing complex medication regimens, and the urgency of accessing communal bathrooms can be overwhelming. In some instances, staff at conventional shelters have been forced to ask seniors to leave if their health or mobility issues make them unable to independently manage within the shelter’s limitations.
The MVP shelter distinguishes itself by offering integrated on-site medical care, a critical component for serving residents as their health needs evolve. This approach was vividly illustrated by the experience of Jamie Mangum, a woman in her 50s battling lung cancer. After a fall in her room, her proximity to an emergency medical technician on-site meant her swollen wrist was treated promptly, allowing her to return to her room without significant delay. Mangum recounted that in other shelters, such an immediate response would have been impossible, likely requiring hours of waiting or arranging for emergency transport. "There, I’d have to wait hours as opposed to come in here, be seen," she stated, underscoring the profound difference specialized care makes.

Beyond immediate medical attention, the MVP’s specialized case managers have been instrumental in assisting Mangum with her ongoing lung cancer treatment. The shelter’s comprehensive support extends to residents with diverse and complex needs. Baleigh Dellos, manager of the MVP shelter for The Road Home, a local nonprofit, explained, "We have clients that need memory care. Maybe they were living independently before, but they were unable to maintain that and got evicted due to dementia or different things like that." This highlights the shelter’s capacity to accommodate individuals whose housing loss stems from cognitive decline or other chronic conditions that impact their ability to live independently.
The on-site medical infrastructure at the MVP is robust. Specialized medical case managers are available, and primary care physicians and therapists make weekly visits. Residents can even access physical therapy within private spaces on the premises, further enhancing the continuity and accessibility of care. This comprehensive medical support is facilitated through a partnership with the Fourth Street Clinic, which provides essential health services to the shelter’s residents.
Matt Haroldsen from the Fourth Street Clinic emphasizes the fundamental importance of medication management for individuals experiencing homelessness. "Their medications get jacked when they’re in their camps," he observed, illustrating the precariousness of storing essential medicines on the streets. He further detailed the plight of diabetic patients who, lacking refrigeration, resort to burying their insulin to keep it cool, often leading to lost or spoiled medication. By enabling residents to securely store and access their medications, the MVP shelter helps stabilize their health conditions. This stability, in turn, allows individuals to focus on other critical tasks, such as obtaining identification and vital documents necessary to apply for disability benefits, Social Security, and programs that can ultimately lead to permanent housing.
The innovative MVP model is not isolated. Similar specialized shelters have emerged in Florida, California, and Arizona, reflecting a growing recognition of the unique challenges faced by older unhoused adults. Caitlin Synovec, assistant director of the National Health Care for the Homeless Council, asserts that access to such tailored facilities can be a matter of life and death. In colder climates, the refusal of shelter to seniors with mobility or health issues, such as incontinence, can have dire consequences. She cited a tragic incident in Bozeman, Montana, in 2022, where a senior froze to death after being turned away from a shelter due to his incontinence.
The inherent risks posed by complex medical needs are often beyond the scope of traditional shelters. Synovec noted, "A typical shelter doesn’t allow somebody on oxygen to come in because that’s such a fire hazard and risk." By creating environments equipped to manage these complexities, the MVP model provides a safer alternative. Synovec advocates for increased integration of healthcare services within shelters as the most effective strategy for helping seniors transition successfully into stable housing. She identifies health issues as a primary driver of housing instability among older adults, making comprehensive medical support a cornerstone of long-term solutions.
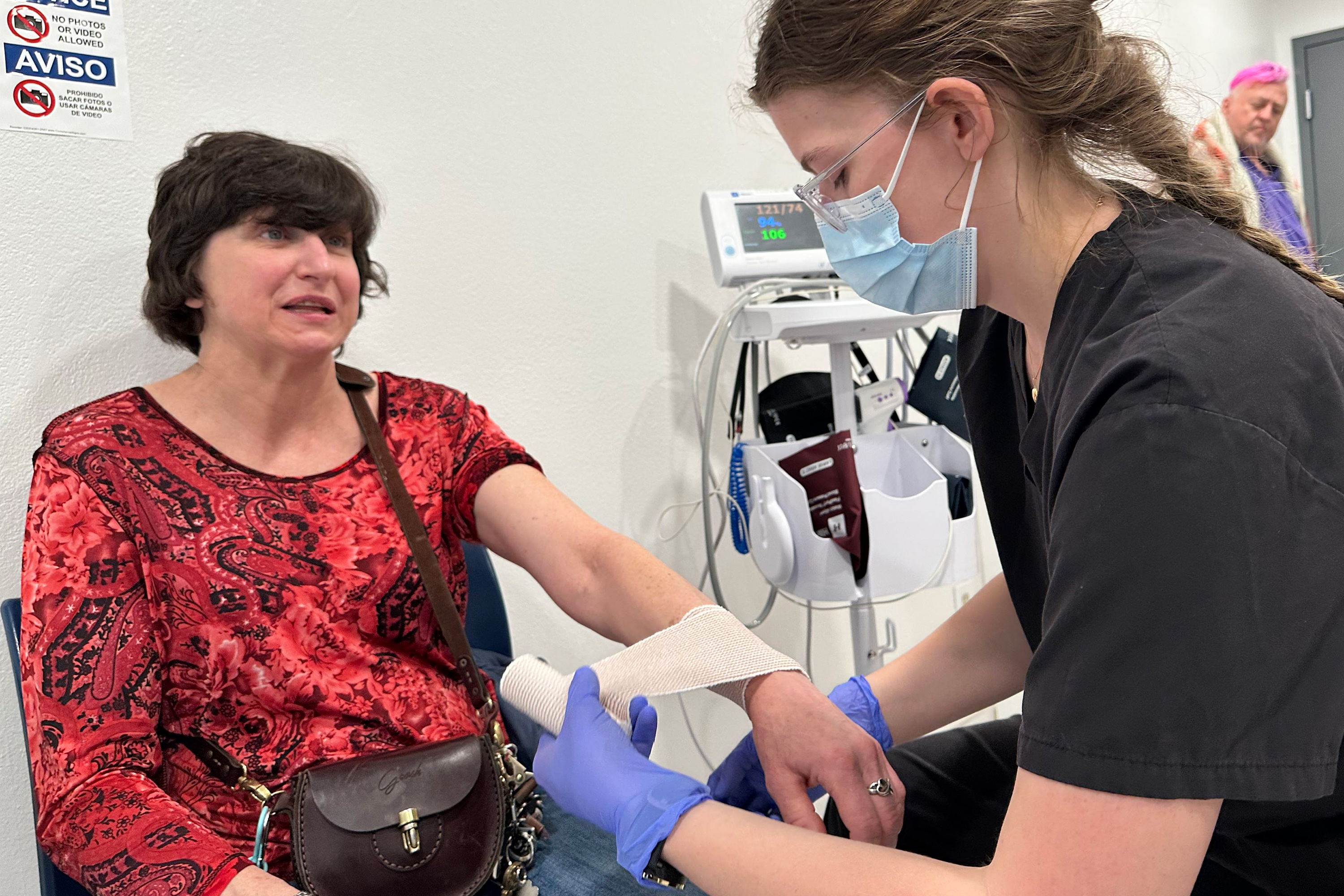
The efficacy of the MVP model is demonstrably contributing to positive outcomes. In Fort Lauderdale, Florida, the nonprofit TaskForce for Ending Homelessness operates Elder Haven, a shelter that has achieved remarkable success. Jacob Torner, vice president of programs for the TaskForce, reported that "Over 80% of the people who’ve stayed in our program this past year have moved into stable or permanent housing." Similarly, the MVP shelter near Salt Lake City has made significant strides, permanently housing 36 seniors by late last year.
Despite these successes, the demand for such specialized services continues to outstrip capacity. Dellos, the MVP shelter manager, indicated that the waitlist typically hovers around 200 individuals. The shelter prioritizes admissions based on medical urgency rather than the length of time on the waitlist, ensuring that those with the most critical needs receive timely assistance. For those fortunate enough to secure a room, the impact is transformative.
Jeff Gregg, a 62-year-old resident, shared his journey at the MVP shelter. A chronic back injury had led to a decades-long opioid addiction, a cycle he found exceptionally difficult to break. He described the constant struggle of trying to maintain employment and housing while battling his addiction and chronic pain. "Fighting that, having a job, insurance, then losing the job, not having insurance, going out to the streets and being back in that crap, and I’d be back in the same position," he reflected.
Gregg explained that the immediate exigencies of survival on the streets—finding food and shelter—often overshadowed his efforts toward sobriety. The MVP shelter provided him with the stability and support he needed to prioritize his recovery. "I was able to get clean. It took me a couple months, but I just kept plucking away," he said. This period of focused recovery paved the way for him to undergo back surgery. He expressed hope that with reduced pain, he can secure employment and, eventually, afford his own apartment, illustrating how specialized support can unlock pathways to independent living.
This article is part of a collaborative effort between NPR and Montana Public Radio.