“This is not just a shelter; it’s a bridge to dignity and health for our most vulnerable seniors.”
In Sandy, Utah, a repurposed two-story brick building is redefining what a homeless shelter can be. The Medically Vulnerable Population (MVP) facility, operated by The Road Home, is specifically designed to serve individuals aged 62 and older, as well as younger adults with chronic health conditions. This innovative approach addresses a critical and growing crisis: the increasing number of seniors experiencing homelessness, a demographic facing unique challenges that traditional shelters are often ill-equipped to handle.
The MVP facility offers a stark contrast to the often-harsh realities of general homeless shelters. Here, shared rooms are thoughtfully designed with mobility issues in mind, and private bathrooms are a standard feature, a vital consideration for residents managing conditions like incontinence. This level of specialized care is crucial, as Dennis Culhane, a researcher at the University of Pennsylvania, points out that the senior homeless population is the fastest-growing segment of the unhoused in the United States. This growth is fueled not only by individuals who have experienced long-term homelessness and are now aging, but also by seniors who are losing their housing for the first time in their lives due to economic hardship, health crises, or lack of affordable housing.
The physical and logistical demands of traditional shelters can be insurmountable for older adults. The simple act of navigating bunk beds, adhering to medication schedules, and accessing shared bathrooms can present significant obstacles. In some instances, individuals unable to manage these challenges independently may be asked to leave, exacerbating their vulnerability. The MVP, however, stands out by integrating medical care directly into its services, creating a supportive environment that can adapt to the evolving health needs of its residents.

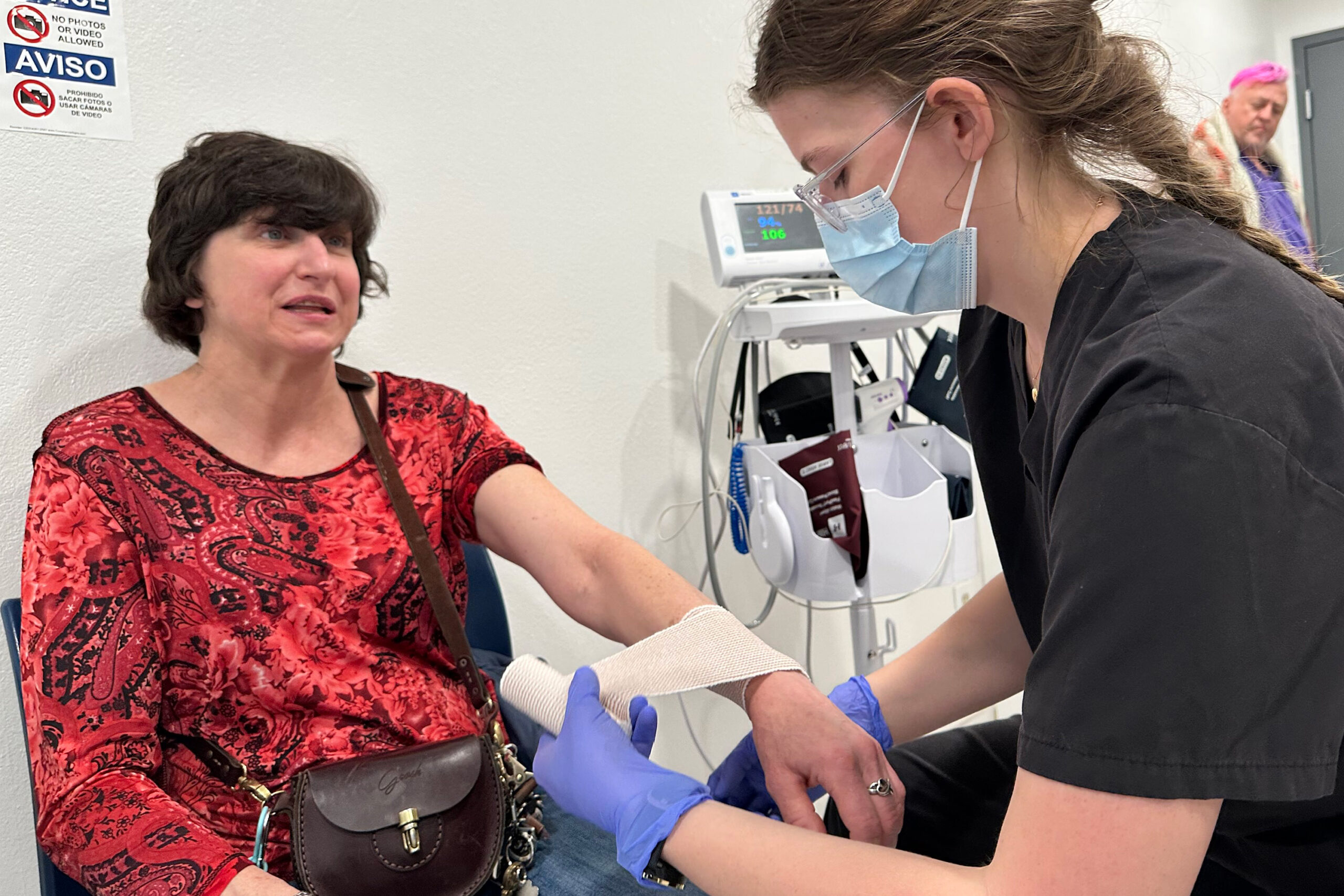
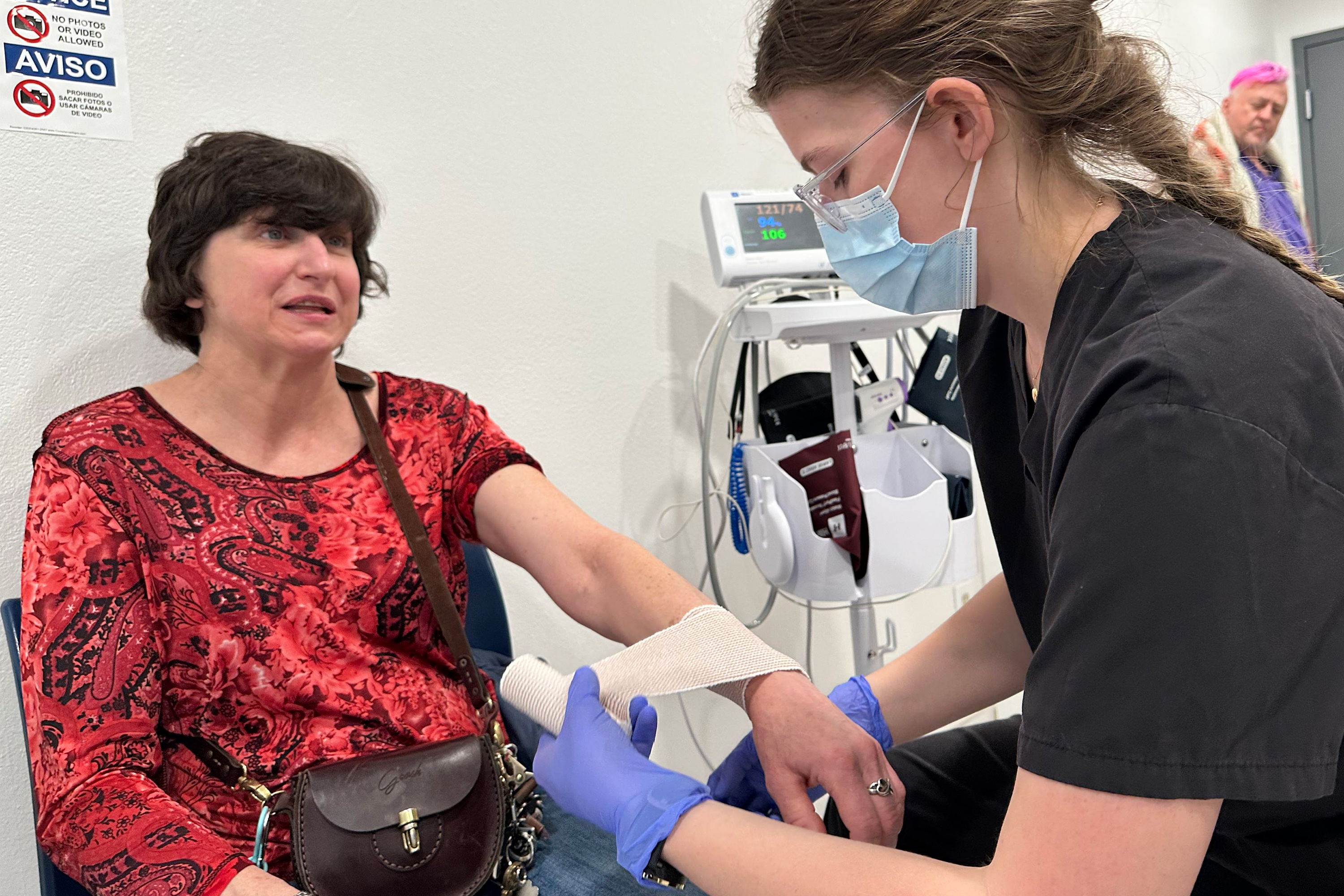
Jamie Mangum, a woman in her early 50s battling lung cancer, experienced this difference firsthand. After a fall in her room, a simple trip downstairs brought her to an on-site emergency medical technician who promptly bandaged her swollen wrist. "In other places, I would have had to wait hours," Mangum stated. "Here, I just go in and they take care of me." Beyond immediate medical attention, the MVP has also facilitated her access to specialized social workers who are assisting her with cancer treatment. This integrated care model ensures that residents receive timely and appropriate medical attention without the added stress of navigating external healthcare systems.
Baleigh Dellos, the manager of the MVP shelter for The Road Home, emphasizes the diverse needs of their residents. "We have clients who need memory care. They may have lived independently before but can no longer do so and were evicted due to dementia or other reasons." The facility addresses these complex needs through a team of specialized medical case managers, along with weekly visits from primary care physicians and therapists. Residents can even receive physical therapy within the shelter’s private spaces, further streamlining their access to essential health services.
The partnership between MVP and the Fourth Street Clinic is a cornerstone of this comprehensive approach. Matt Haroldsen of Fourth Street Clinic highlights that for many newly arrived individuals, managing their medications is the immediate priority. For those experiencing homelessness, simply keeping medications safe and viable is a significant challenge. "When they’re in encampments, their medicine gets stolen," Haroldsen explained. Insufficient refrigeration, for example, can lead to insulin spoiling, rendering it useless for individuals with diabetes. By ensuring access to and proper storage of medications, the MVP helps stabilize residents’ health conditions. This stability, in turn, allows them to focus on other crucial steps toward self-sufficiency, such as obtaining identification, applying for disability benefits, Social Security, and programs that can help secure permanent housing.
The MVP model is not an isolated initiative. Local governments and non-profit organizations in states like Florida, California, and Arizona have also recognized the growing need and launched similar specialized shelters to address the unique requirements of older adults experiencing homelessness. Caitlin Synovec, deputy director of the National Health Care for the Homeless Council, underscores the life-saving potential of these facilities. "Access to specialized shelters can mean the difference between life and death," she stated. In colder climates, denying shelter to seniors due to mobility issues or medical conditions can be particularly perilous. Synovec recounted the tragic case of an elderly man in Montana who died of exposure after being turned away from a shelter due to incontinence, a situation that specialized facilities are designed to prevent.
Furthermore, the complex medical needs of some homeless seniors can pose safety risks in traditional shelters, which are often not equipped to manage such situations. "A typical shelter won’t allow someone in with oxygen because it represents a fire risk," Synovec noted. By providing on-site medical care, specialized shelters not only protect their senior residents but also create a safer environment for everyone within the facility. Synovec also points out that addressing health issues within shelters is paramount to helping seniors maintain housing once they secure it. Health problems are a common reason why many older adults struggle to afford or keep their homes.
The MVP model is demonstrating significant success, both in Utah and in replication efforts across the country. Jacob Torner, vice president of programs at the Task Force for Ending Homelessness in Fort Lauderdale, Florida, which operates a similar shelter called Elder Haven, reported that "More than 80% of the people who went through our program last year were able to move into stable or permanent housing." The MVP facility in Sandy has also achieved notable success, permanently housing 36 seniors by the end of last year.
Despite these successes, the demand for such specialized services far outstrips the available capacity. Dellos shared that the MVP’s waiting list consistently hovers around 200 individuals. The facility prioritizes those with the most acute medical needs, rather than simply following a first-come, first-served approach, ensuring that resources are directed to those who require immediate and intensive care.
For those who do secure a place at the MVP, the impact can be transformative. Jeff Gregg, a 62-year-old resident, shared his journey of recovery. Plagued by chronic back pain from an old injury, Gregg had struggled with opioid addiction for decades. He described the cyclical nature of his homelessness, losing jobs and health insurance, only to find himself back on the streets. "Struggling with that, having a job, health insurance, then losing the job, no insurance, ending up on the street and back in that hell. And I’d go back to the same place," he recounted.
Gregg explained that during periods of homelessness, the immediate need for food and shelter often overshadowed his desire for sobriety. At the MVP, however, he found an environment conducive to healing. "I was able to get off the drugs. It took me a couple of months, but I chipped away at it," he said. This newfound stability allowed him to undergo back surgery, significantly reducing his chronic pain. Gregg now hopes that with improved health, he can find employment and secure his own apartment, marking a profound step towards independence and a life free from the constant struggle of homelessness. The MVP shelter, therefore, represents more than just a roof over their heads; it is a vital sanctuary offering comprehensive care, dignity, and a pathway to a more stable and healthier future for aging individuals facing unprecedented challenges.