"A new government incentive offers GP practices in England £3,000 annual bonuses for prescribing the weight loss drug Mounjaro, alongside £1,000 for referrals to weight management programs, aiming to broaden access and shift towards preventative care, yet critics warn it won’t resolve the deep-seated issues of limited NHS eligibility and the growing private market."
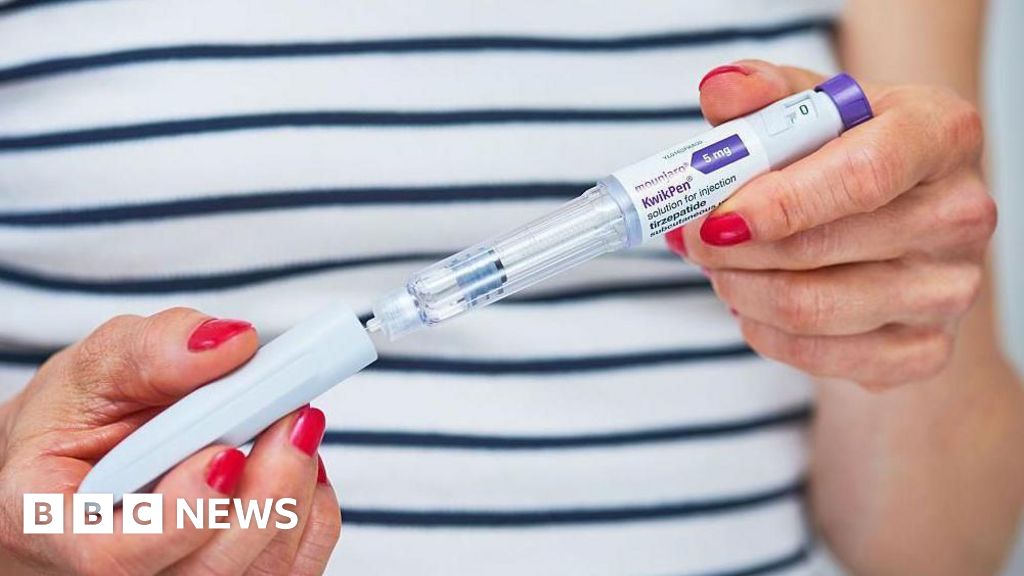
The UK government is introducing a significant shift in its approach to tackling obesity, integrating financial incentives into the General Practitioner (GP) contract in England. Starting this April, GP practices will be eligible for annual bonuses of £3,000 for prescribing the weight loss medication Mounjaro (tirzepatide) to eligible patients, with an additional £1,000 available for referring individuals to structured weight management programmes. This move, championed by ministers as a crucial step towards democratising access to effective weight loss support and fostering a preventative healthcare model, has ignited a complex debate among healthcare professionals and public health experts regarding its true impact on the nation’s obesity crisis.
Addressing a Growing Public Health Challenge
Obesity remains one of the most pressing public health challenges in England, with alarming rates contributing to a significant burden on the National Health Service (NHS). Statistics reveal that approximately two-thirds of adults in England are overweight or obese, leading to a myriad of associated health conditions such as Type 2 diabetes, heart disease, certain cancers, and musculoskeletal problems. The direct and indirect costs of obesity to the NHS and wider economy are staggering, estimated in the billions of pounds annually. Against this backdrop, the advent of new-generation weight loss medications, often referred to as GLP-1 (Glucagon-like peptide-1) receptor agonists and, in the case of Mounjaro, also a GIP (Glucose-dependent insulinotropic polypeptide) receptor agonist, has been hailed as a potential "game changer." These injectable drugs work by mimicking natural hormones that target areas of the brain involved in appetite regulation, leading to reduced hunger, increased satiety, and improved blood sugar control, resulting in significant weight loss for many patients.
The government’s introduction of these incentive payments signals a strategic intent to leverage the primary care network in addressing this chronic condition. Health Secretary Wes Streeting articulated this vision, stating, "Weight loss drugs can be a real game changer for those who need them. I’m determined that access should be based on need, not ability to pay." He further underscored the policy’s dual aims: to combat the proliferation of unregulated private prescribers and potentially dangerous unlicensed drugs, and to reposition the NHS’s focus from reactive treatment to proactive prevention.
The Mechanism of GP Incentives: A Closer Look
Incentive payments are not a novel concept within the GP contract framework in England. They form a core component of the Quality and Outcomes Framework (QOF), a voluntary annual scheme that rewards practices for achieving specific targets in areas like chronic disease management, preventative care, and public health initiatives. Historically, QOF payments have incentivised improvements across a spectrum of care, from boosting vaccination rates and enhancing dementia care to promoting statin prescriptions for cardiovascular risk reduction. This new inclusion marks the first time that weight loss drugs have been integrated into this incentivisation model. The £3,000 bonus is structured to reward practices for prescribing Mounjaro to the maximum number of eligible patients within their caseload, reflecting a direct link between clinical activity and financial remuneration.
For Mounjaro specifically, its introduction to GP prescribing commenced during the current financial year. Initial access has been tightly controlled, primarily restricted to individuals with severe obesity, defined as a Body Mass Index (BMI) of over 40, who also present with co-morbid health conditions related to their weight. The eligibility criteria are set to expand in the upcoming year, encompassing patients with a BMI over 35 who meet the co-morbidity criteria. Furthermore, the guidelines acknowledge and account for ethnic disparities in health risks associated with weight, offering lower BMI thresholds for certain ethnic groups. The ambition is substantial, with projections aiming for 220,000 patients to be receiving Mounjaro via the NHS by 2028. However, reports suggest that the initial rollout has been uneven, with some GPs not prescribing the drug as extensively as anticipated, possibly due to a combination of factors including supply issues, lack of familiarity, or concerns over patient eligibility and ongoing support needs.
Navigating the Complexities: Eligibility, Access, and the Private Market
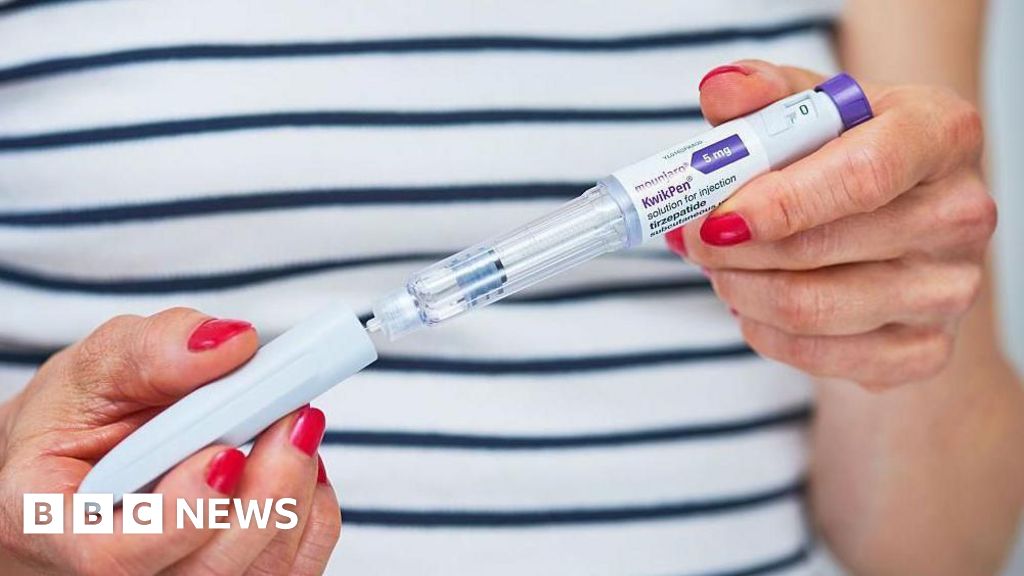
While the incentive scheme aims to broaden access, a significant point of contention revolves around the strict NHS eligibility criteria. Unlike Mounjaro, its counterpart, Wegovy (semaglutide), is currently only prescribed through specialist NHS weight management services, not by GPs. This distinction highlights a tiered system of access within the NHS, dictated by the severity of obesity and the associated clinical complexity.
The stark reality is that the vast majority of individuals currently using these new-generation weight loss drugs in the UK—estimated at over 1 million people—are doing so by paying privately. This burgeoning private market, often fuelled by online pharmacies and weight loss clinics, underscores a critical divide: those with the financial means can access these medications, while those reliant on the NHS face stringent criteria and potentially long waits. Health Secretary Streeting’s comments implicitly acknowledge this "pay-to-access" conundrum, framing the GP incentive as a means to level the playing field. However, critics argue that without a fundamental expansion of NHS eligibility criteria, the incentive primarily encourages GPs to prescribe to an already narrowly defined group, doing little to bridge the gap for the broader population struggling with obesity. The dangers of the private market, including the availability of unregulated or counterfeit drugs and the absence of comprehensive medical oversight, are also a serious concern that the government is keen to mitigate.
Expert Skepticism and Practical Concerns
The announcement has been met with a nuanced, often critical, reception from leading medical and public health bodies. Katharine Jenner, Director of the Obesity Health Alliance, while welcoming the incentives as a step forward, tempered expectations. She emphasised that "This doesn’t mean weight loss drugs will suddenly be available to everyone who wants them." Jenner highlighted that NHS access would remain highly restricted, focused on those with the greatest clinical need, and crucially, that these treatments are most effective when integrated with sustained, holistic support – a component that the incentive payment for referrals only partially addresses. She further stressed the need for a broader public health strategy, advocating for "stronger action to improve the food environment and prevent obesity in the first place," rather than solely focusing on pharmaceutical interventions.
Dr Katie Bramall, representing the British Medical Association (BMA), echoed these concerns, stating unequivocally that "While the headlines promise much, in reality there will be no change to NHS England’s eligibility criteria for patients to access injectable weight-loss medication on the NHS." Dr Bramall underscored that the proposals would do nothing in the short term to address the profound disparity between those who can afford private treatment and those who cannot.
Adding to this, Professor Victoria Tzortziou Brown of the Royal College of GPs (RCGP) raised important practical and ethical considerations. She firmly asserted that "GPs do not withhold treatment or prescribe based on financial incentives. Decisions are guided by clinical judgement and what is safest and most appropriate for individual patients." Professor Tzortziou Brown articulated the RCGP’s apprehension that a wider rollout of these medications in general practice could significantly increase workload in an already overstretched system, potentially creating unsustainable pressures. Furthermore, she warned against the risk of "raising unrealistic expectations among patients who may not be eligible or for whom these medicines are not suitable," highlighting the complexities of managing patient demand and clinical appropriateness within the confines of current NHS resources and guidelines.
Towards a Comprehensive Solution
The government’s new incentive scheme for GP-prescribed weight loss drugs represents a significant policy intervention in the ongoing battle against obesity. It reflects a commitment to leverage pharmaceutical advancements and primary care infrastructure to address a critical public health issue. By integrating these incentives into the GP contract, ministers hope to streamline access for eligible patients, encourage earlier intervention, and ultimately alleviate some of the pressure on specialist services and the broader NHS.
However, the policy faces considerable challenges. The fundamental issue of limited NHS eligibility, driven by the high cost of these medications and the need for careful patient selection, remains unresolved. Critics argue that without a substantial expansion of these criteria, the incentive primarily serves to optimise existing, restricted pathways rather than truly democratising access. Moreover, the concerns raised by professional bodies regarding potential increases in GP workload, the ethical implications of financial incentives in clinical decision-making, and the need for comprehensive, wrap-around support alongside medication, cannot be overlooked.
The long-term effectiveness of this strategy will depend not only on the uptake of prescriptions but also on its integration into a broader, multi-faceted approach to obesity prevention and management. This includes sustained investment in public health campaigns, policies aimed at improving the food environment, and a robust system of behavioural and lifestyle support programmes. While the £3,000 bonus is a notable step, the journey towards a healthier nation, where access to effective weight management is truly equitable and sustainable, is far from complete and will require continuous evaluation, adaptation, and a holistic vision beyond pharmaceutical interventions alone.