"This innovative at-home technology is not just about regaining physical function; it’s about restoring fundamental human dignity and the profound sense of freedom that comes with independence after a stroke. For survivors like Amanda James-Hammett, it marks a pivotal shift from dependence to self-sufficiency."
The devastating impact of stroke, which affects hundreds of thousands annually and leaves over a million grappling with long-term disability in the UK alone, has long presented a significant challenge to healthcare systems worldwide. Traditional rehabilitation, while crucial, often struggles with accessibility, intensity, and duration, leaving many survivors yearning for greater recovery. A groundbreaking nationwide NHS trial, the Triceps study, is now offering a beacon of hope by testing a novel at-home device that combines targeted brain stimulation with rehabilitation exercises, promising to revolutionize post-stroke care and empower individuals to reclaim their lives.
A Personal Journey of Regaining Freedom

Amanda James-Hammett’s life irrevocably changed at the age of 37 when, while performing the routine task of washing dishes, she experienced a sudden, disorienting "pop" in her head. "I tried to scream, but it wasn’t a normal scream. I knew something wasn’t right," she recounts, describing the terrifying onset of a stroke that would, within hours, strip her of the ability to speak and move her right arm. The ensuing years were a relentless battle, a painstaking process of relearning basic human functions – how to talk, read, and perform the myriad everyday tasks most take for granted. This journey, fraught with physical and emotional hurdles, highlights the profound impact of stroke, which often extends far beyond the initial medical crisis, affecting every facet of a survivor’s existence.
Six years after her stroke, Amanda embarked on a new chapter in her recovery by participating in the Triceps trial. Her initial skepticism quickly gave way to cautious optimism. After just a few weeks of using the device, she began to notice tangible improvements in her hand and arm movement. For Amanda, the true measure of this progress wasn’t just physical; it was deeply personal. A passionate seamstress before her stroke, the inability to engage in her beloved hobby had been a source of immense frustration. The device, however, allowed her to return to her sewing machine, meticulously cutting fabric and operating the intricate machinery. "It’s about freedom," Amanda passionately declares, "It’s given me my freedom back." This sentiment encapsulates the trial’s core promise: to restore not just movement, but the autonomy and quality of life that define true independence. She now describes herself as "a new woman," able to perform essential daily tasks like putting on socks and shoes, and managing her household without constant reliance on others. These "small things," she emphasizes, make "a big difference," underscoring the profound psychological and practical benefits of regaining functional independence.
Understanding the Silent Epidemic: Stroke and its Aftermath
Dr. Sheharyar Baig, a distinguished neurologist at Sheffield’s Royal Hallamshire Hospital, underscores the critical nature of stroke. He explains that a stroke occurs when the blood supply to a part of the brain is interrupted, either by a clot (ischemic stroke) or a burst blood vessel (hemorrhagic stroke). This interruption deprives brain cells of oxygen and nutrients, causing them to die within minutes. The specific symptoms – ranging from weakness and paralysis to visual disturbances and speech problems – depend entirely on the affected area of the brain. Dr. Baig stresses the urgency of recognizing symptoms, advising immediate emergency medical attention by calling 999.

The statistics paint a stark picture: stroke is the leading cause of adult-onset disability in the UK, impacting approximately 100,000 individuals each year. More than a million people are currently living with its long-term effects, a testament to the chronic and often debilitating nature of the condition. A staggering half of all stroke survivors contend with persistent arm weakness, a condition that can manifest anywhere from subtle loss of dexterity to complete paralysis. This impairment severely compromises the ability to perform Activities of Daily Living (ADLs) such as dressing, cooking, and working, often leading to increased dependence, social isolation, and a significant reduction in overall quality of life. The ripple effect extends to the healthcare system, exacerbating pressure on already strained health and social care services. Consequently, developing innovative solutions that facilitate recovery outside of traditional hospital settings is not merely beneficial, but vital for sustainable long-term care.
The Science of Recovery: Vagus Nerve Stimulation
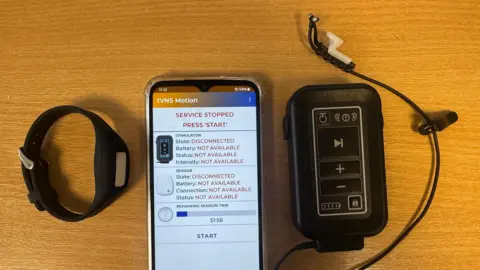
The technology at the heart of the Triceps trial represents a significant leap in stroke rehabilitation. Participants utilize a small, non-invasive electrical device that comfortably fits inside the ear. This device delivers targeted stimulation to the vagus nerve, a crucial cranial nerve that extends from the brainstem through the neck and into the chest and abdomen. The vagus nerve plays a pivotal role in regulating various bodily functions, including heart rate, digestion, and mood, and crucially, has connections to brain regions involved in motor control, learning, and memory.
Unlike earlier, more invasive forms of vagus nerve stimulation (VNS) that required surgical implantation, this transcutaneous auricular VNS (taVNS) device offers a comfortable and easily accessible alternative. The device is designed to be used concurrently with conventional rehabilitation exercises. Dr. Baig elaborates on the underlying principle: "The recovery process is unfortunately quite slow for many people… So we’re interested in ways we can boost the effects of rehab and create a brain environment that’s more responsive to it."
The scientific rationale behind combining VNS with physical therapy lies in its ability to enhance neuroplasticity – the brain’s remarkable capacity to reorganize itself by forming new neural connections and pathways. VNS is believed to achieve this by modulating the release of key neurotransmitters, such as acetylcholine and norepinephrine, which play critical roles in attention, learning, and memory consolidation. By stimulating the vagus nerve during active rehabilitation, the brain is essentially "primed" to better absorb and retain the motor learning from the exercises. This synergistic approach aims to make each rehabilitation session more effective, accelerating the recovery of lost function. The electrical pulses delivered by the ear-piece are meticulously calibrated to ensure comfort and freedom from pain, making the treatment both effective and user-friendly.
The Triceps Trial: A Landmark Endeavour
The Triceps trial, a substantial £2 million study, stands as the largest trial of brain stimulation and stroke ever undertaken, a testament to the ambition and potential impact of this research. It is a collaborative effort spearheaded by Sheffield Teaching Hospitals NHS Foundation Trust in partnership with the University of Sheffield, demonstrating a robust fusion of clinical expertise and academic innovation. The trial’s expansive reach encompasses 19 NHS sites across the UK, ensuring a diverse and representative participant pool. With a recruitment target of approximately 270 individuals, the study is designed to gather comprehensive data, providing statistically significant insights into the efficacy of the device.
Crucially, the trial employs a blinded methodology, meaning neither the participants nor the researchers directly involved in their care know whether an individual is receiving active vagus nerve stimulation or a placebo. This rigorous scientific approach is essential for eliminating bias and ensuring the validity of the results. The Stroke Association, a key partner and part-funder of the research, is deeply invested in the trial’s success. Maeva May, the charity’s associate director of systems engagement, highlights an additional layer of research: "The team are doing brain imaging and taking blood tests because we know that some stroke patients really respond well to this technology while some don’t. We want to understand what patients respond best and how." This focus on identifying biomarkers for responsiveness is critical for the future of personalized medicine in stroke rehabilitation, allowing clinicians to tailor treatments to individuals who are most likely to benefit.

Promising Early Outcomes and Future Horizons
With over 200 individuals already having participated, the early indications from the Triceps trial are remarkably promising. Despite the blinded nature of the study, Dr. Baig reports "wonderful improvements in people’s arm function." While cautioning that the treatment is not a cure, he emphasizes its potential to significantly enhance daily life. He shares compelling anecdotes of participants experiencing tangible improvements, such as an individual who progressed from being unable to carry a cup of tea with one arm to stably walking from room to room with it, and another who achieved a post-stroke personal best in a 5K run, noting improved arm function during their activity. These examples, though anecdotal at this stage, powerfully illustrate the potential for functional gains that profoundly impact quality of life.
The scalability of this technology is another key factor in its potential widespread adoption. Dr. Baig notes that if proven effective, the device could be "quite scalable" due to its affordability, convenience, and ease of integration into existing rehabilitation pathways. This is a crucial consideration for national healthcare systems grappling with the long-term care needs of stroke survivors. A successful outcome from the Triceps trial could pave the way for a paradigm shift in post-stroke rehabilitation, moving towards more accessible, home-based, and technologically augmented recovery programs. Such a shift could alleviate pressure on inpatient facilities, reduce healthcare costs, and most importantly, empower stroke survivors to continue their recovery journey in the comfort and familiarity of their own homes.
For Amanda James-Hammett, the impact is already undeniable. Her ability to perform everyday tasks independently, to engage in her cherished hobbies, and to navigate her daily life with newfound autonomy speaks volumes. "It’s about being independent again," she reiterates. "Those small things make a big difference." As the Triceps trial progresses towards its final analysis, the medical community, stroke survivors, and their families eagerly anticipate results that could transform the landscape of stroke recovery, offering a tangible path toward greater independence and a richer, more fulfilling life.
