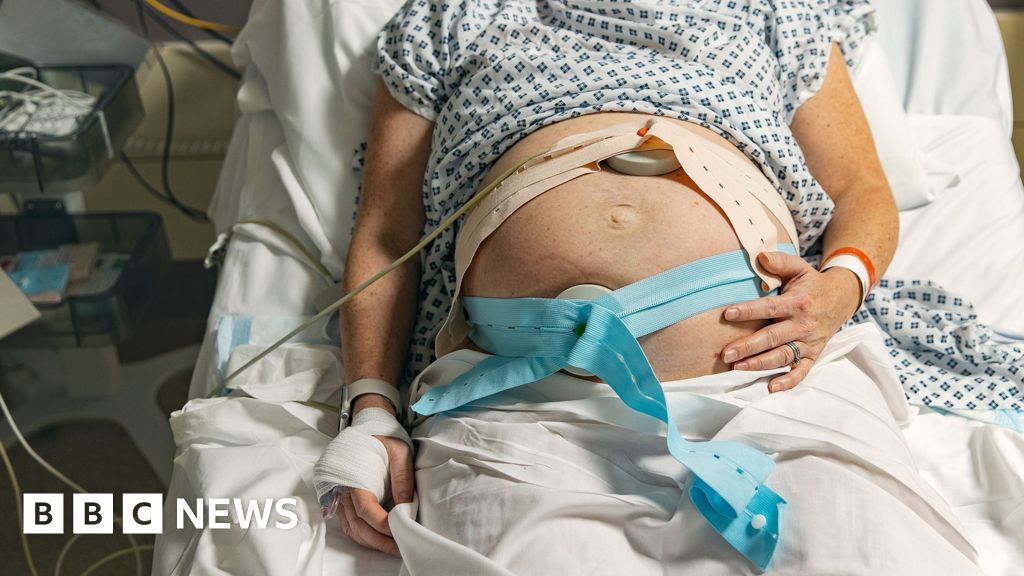
"Maternity and neonatal services in England are failing too many women, babies, families and staff," states Baroness Amos, leading a government-commissioned review, highlighting a deeply concerning pattern of inconsistent and often poor care across the nation.
An interim report has cast a stark light on the widespread systemic failures within England’s maternity services, revealing a troubling landscape where problems persist at every critical stage of the maternity journey. The review, spearheaded by Baroness Amos, identifies critical issues including pervasive racism, acute staffing shortages, and a chronic lack of accountability as key drivers behind the delivery of substandard care, impacting thousands of families and underscoring an urgent need for comprehensive reform.
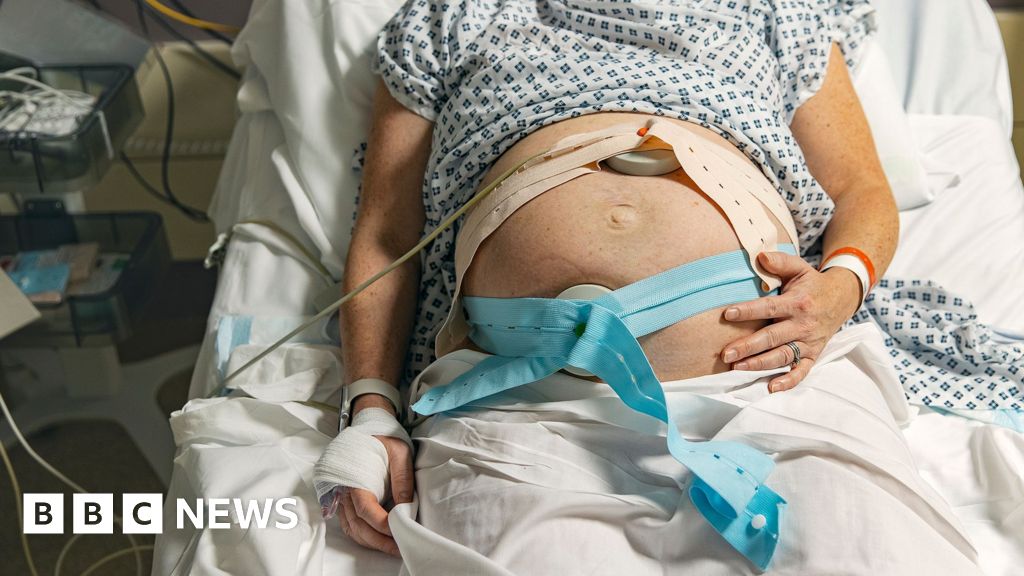
Maternity services across England are currently failing a significant number of families, with issues identified at every point from antenatal care through to birth and postnatal support, according to a pivotal interim report. This extensive review, led by Baroness Amos and commissioned by the government, has pinpointed six critical factors contributing to these widespread failings: systemic racism, chronic staffing shortfalls, a profound lack of accountability, poor staff relationships, inadequate listening to patient concerns, and insufficient learning from past incidents.
The magnitude of the crisis is underscored by the overwhelming response to the review, with over 8,000 individuals having submitted evidence and Baroness Amos personally engaging with more than 400 affected families. Her final recommendations, eagerly anticipated, are scheduled for release in April, with Health Secretary Wes Streeting pledging to implement them decisively.
Speaking to BBC Breakfast, Baroness Amos articulated the deeply inconsistent nature of care delivery: "I have seen bad, poor, good and excellent care co-existing side by side. Families have described to me good experiences, terrible experiences. It is patchy, it is inconsistent and what this investigation is about, is trying to find out the things that move us from poor and bad to good and excellent." She unequivocally affirmed the existence of safe and good care in some areas, yet stressed that "way too many examples of poor care" have been uncovered. The emotional toll on families is immense, with experiences described as "so traumatic and distressing." While some NHS Trusts have demonstrably changed practices in response to previous incidents, the overall picture remains profoundly mixed and inconsistent.
The six key areas of concern identified in Baroness Amos’s interim report paint a comprehensive picture of the challenges facing maternity and neonatal services. While specific details of each bullet point were not provided in the original text, the overarching themes are clear. Racism within the system manifests in various forms, from overt discrimination to subtle biases that can lead to poorer outcomes for Black, Asian, and other ethnically diverse women and their babies. This can include delayed care, dismissive attitudes towards pain and concerns, and a general lack of cultural competency among staff. Addressing this requires not only explicit anti-racism training but also systemic changes to ensure equitable care pathways and a truly inclusive environment.
Staffing issues are a perennial problem across the NHS, and maternity services are particularly vulnerable. Chronic understaffing, coupled with high rates of burnout among midwives and obstetricians, leads to increased pressure, rushed care, and a greater propensity for errors. The lack of sufficient skilled personnel can mean longer waiting times, reduced one-to-one care during labour, and a struggle to meet the complex needs of all patients. This directly impacts both patient safety and staff well-being, creating a vicious cycle of stress and suboptimal care.
Accountability issues are deeply rooted, contributing to a culture where mistakes are not always learned from, and individuals or institutions are not consistently held responsible for failings. This can manifest as a lack of transparency, an inability to conduct thorough investigations, or a reluctance to implement necessary changes following adverse events. Without robust accountability mechanisms, there is little incentive for systemic improvement, and the same mistakes can be tragically repeated.

Poor staff relationships and communication breakdowns within maternity teams can have devastating consequences. A lack of trust, hierarchical structures that stifle open dialogue, and inter-professional rivalries can prevent vital information from being shared, concerns from being escalated, and collaborative decision-making from occurring effectively. This "cultural problem," as described by some families, where professionals may believe they know better than the mother herself, directly undermines patient-centred care and can lead to serious errors when patient concerns are dismissed.
The failure to listen to women’s concerns is a recurring and deeply distressing theme. Many families have reported feeling unheard, dismissed, or even patronized when raising anxieties about their own health or that of their baby. This can result in delayed diagnosis, missed warning signs, and ultimately, preventable harm. Empowering women to advocate for themselves and ensuring that their voices are central to their care journey is paramount.
Finally, the lack of effective learning from past incidents means that critical lessons are often lost or not universally applied. Despite numerous reports and inquiries into specific trusts, systemic issues persist, indicating a failure to translate findings into widespread, impactful change across the entire maternity landscape.

Baroness Amos’s statement encapsulates the gravity of the situation: "It is clear from the meetings and conversations I have had with hundreds of women, families and staff members across the country, that maternity and neonatal services in England are failing too many women, babies, families and staff." This acknowledgment validates the long-standing concerns of numerous families and advocates.
Indeed, failures within the system are not a new revelation. For more than a decade, the BBC has diligently reported on cases of poor care, speaking to bereaved and harmed families across various NHS Trusts. High-profile inquiries into failings at Morecambe Bay, Shrewsbury & Telford, East Kent, Nottingham, and Leeds, among others, have consistently exposed patterns of preventable deaths, severe injuries, and a culture of inadequate care. These investigations have highlighted issues such as insufficient staffing, a lack of fetal monitoring expertise, an overreliance on natural birth at all costs, and a failure to escalate concerns appropriately. Despite these previous findings, the current interim report suggests that fundamental problems remain stubbornly entrenched.
The tragic case of Orlando Davis serves as a poignant example of the consequences of these systemic failures. Orlando died in September 2021, aged just 14 days, after staff at Worthing Hospital in Sussex failed to identify that his mother, Robyn, had developed hyponatremia – a dangerously low level of sodium in her bloodstream – during labour. An inquest later concluded that neglect had contributed to the infant’s death. Robyn’s heartfelt testimony, "not listening to my concerns is the main reason we’re sat here without our son," resonates deeply with the experiences of many other families. Her husband, Jonathan, attributes this to a "cultural" problem within maternity services, where midwives may erroneously believe their professional knowledge surpasses the mother’s intrinsic understanding of her own body. He argues that "the only one that truly knows what’s going on in that individual’s body is the mother."
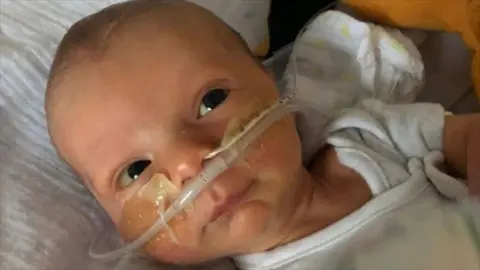
The Davis family is a leading voice in "Truth for Our Babies," a campaign group advocating for an independent investigation into maternity services at the University Hospitals Sussex NHS Trust. Their efforts gained further urgency following a joint investigation by BBC News and the New Statesman, which revealed that at least 55 babies over a five-year period might have survived had they received better care at the trust.
Despite the ongoing government-commissioned review, the Davis family expresses profound skepticism that the Amos review will instigate the necessary improvements across England, and they are vociferously calling for a statutory inquiry instead. Robyn asserts that the current review "is not going deep enough… it’s not just what’s happening at these hospitals. It’s the regulators as well." She points out that the regulators themselves are not subject to review by Baroness Amos, a critical oversight in their view. Jonathan echoes this sentiment, stating, "As families, we have received lacklustre care. We [therefore] deserve the gold standard of accountability – and progressing a rushed, high-level review, instead of a statutory inquiry, is not receiving the gold standard. Future mothers and future children may not suffer the same irreversible fate that we have if a [properly] conducted inquiry happens." A statutory inquiry, with its broader powers to compel evidence and make binding recommendations, is seen by many as the only mechanism capable of delivering the depth of investigation and accountability required.
Labour MP Michelle Welsh, a prominent campaigner for maternity safety, shares these concerns, warning that the Amos review risks becoming a "damp squib" if not followed by robust action. She urges the government to act decisively, including the crucial step of creating a dedicated maternity commissioner responsible for driving and overseeing improvements in care nationwide. "This inquiry must result in some big, bold policies with regards to maternity services, that really says that as a government we want to improve maternity services, we want to invest in it, and we will secure the truth and accountability for families," Welsh emphasized.

Further exacerbating anxieties, it has recently emerged that a maternity taskforce, which Health Secretary Wes Streeting pledged to chair early this year to drive improvements, has yet to be established. Announced last June, the delay in forming this critical group raises questions about the government’s commitment and urgency in addressing the crisis. The Department for Health and Social Care has stated that the membership would be announced "shortly," but Welsh underscores the importance of its immediate formation: "It is important that the taskforce is established as soon as possible, because without it we don’t have that driving force [and] those big, bold policies."
The interim report by Baroness Amos serves as a sobering reminder of the profound challenges embedded within England’s maternity services. It highlights a system struggling with deep-seated issues that compromise safety, equity, and the quality of care for expectant mothers and their babies. As the final recommendations approach, the focus will undoubtedly shift to the government’s response and its capacity to translate these findings into tangible, lasting improvements. The calls from bereaved families and dedicated campaigners for a more comprehensive, accountable, and urgent approach underscore the high stakes involved in reforming a service that is fundamental to the health and well-being of the nation. Without decisive action, the cycle of tragic failings and profound distress for families risks continuing unabated.