"Hundreds of GPs admit they have never refused a sick note for mental health, highlighting a system where doctors often feel caught between advocating for patients and policing workplace absence, with significant implications for both healthcare and national productivity."
This revelation stems from a BBC News investigation, which surveyed over 5,000 General Practitioners across England, uncovering widespread frustration and a perceived inability to deny requests for sick leave due to mental health conditions. The findings illuminate a complex and increasingly strained system, where GPs are struggling with escalating demands, ethical conflicts, and patient pressures, ultimately questioning the efficacy and appropriateness of their role in certifying fitness for work.
The Unspoken Burden: GPs and Mental Health Fit Notes
A groundbreaking investigation by BBC News has cast a revealing light on the escalating pressures faced by General Practitioners in England, particularly concerning their role in issuing "fit notes" for mental health conditions. The survey, which reached out to over 5,000 GPs, revealed that a significant majority of those who responded have never refused a patient’s request for sick leave due to mental health issues, underscoring a profound systemic challenge within primary care.
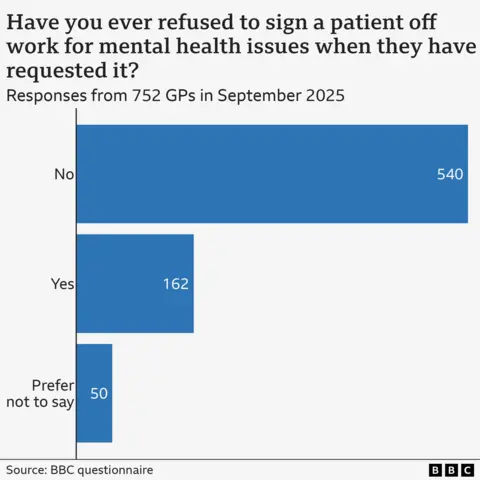
Of the 752 GPs who participated in the questionnaire, a striking 540 (approximately 72%) reported that they had never once denied a request for a fit note related to mental health. In contrast, only 162 GPs (around 21.5%) indicated they had turned down such a request, while a further 50 preferred not to disclose their stance. This stark imbalance suggests that many GPs feel compelled, or at least highly predisposed, to approve these requests, raising critical questions about diagnostic autonomy, patient-doctor dynamics, and the broader societal implications of long-term work absence.

The findings resonate deeply with long-standing concerns within the medical community regarding the expanding administrative burden on GPs and the inherent conflict of interest embedded in the fit note system. Many respondents expressed profound frustration, with some vehemently arguing that the provision of fit notes should not fall under the purview of general practice. This sentiment highlights a crucial tension: GPs are trained to be patient advocates, focusing on health and recovery, yet they are simultaneously tasked with acting as gatekeepers for the welfare system and employers, a role often perceived as adversarial to their primary function.
Escalating Demands: The Rise of Mental Health Absences
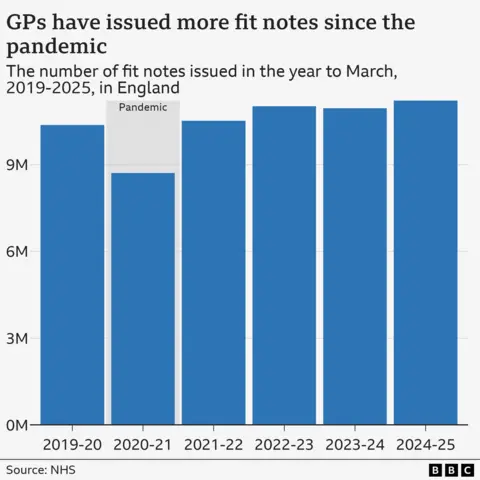
The context for these GP insights is a national trend of steadily increasing fit note issuance. Data reveals that over 11.2 million fit notes were approved by GP practices in England last year alone, marking an increase of almost 850,000 over the past six years. This upward trajectory, only briefly interrupted during the initial phase of the Covid-19 pandemic, reflects a growing challenge in keeping the workforce healthy and engaged. The economic impact of such widespread absence, both in terms of lost productivity and the cost of statutory sick pay and benefits, is substantial and a key driver for calls for reform.
Crucially, mental health and behavioural disorders have emerged as the predominant underlying reason for these absences. Last year, more than 956,000 fit notes specifically cited these conditions, far surpassing any other single medical category, such as musculoskeletal problems or respiratory illnesses. This surge in mental health-related sick leave points to a multifaceted crisis, potentially driven by factors such as heightened workplace stress, increased awareness and reduced stigma around mental illness leading to more self-reporting, and potentially inadequate access to timely mental health support services that could facilitate earlier intervention and return to work. Societal shifts, the pervasive influence of digital communication, and post-pandemic anxieties are also cited by experts as contributing factors to the rising tide of mental ill-health impacting the working population.
Fit notes, which replaced the traditional "sick note" in 2010, were initially designed to advise on how a patient’s health problems impact their ability to work for more than seven days. They offer two main designations: "not fit for work" or "maybe fit for work" with suggested adjustments. The latter option was intended to encourage partial returns or modified duties, fostering a more nuanced approach to workplace reintegration. However, the vast majority of fit notes currently issued declare individuals "not fit for work" entirely, and a significant 72% do not even specify a reason for absence, making it difficult for employers to offer appropriate support or modifications. While GPs issue the majority, the ability to provide fit notes has recently been extended to other healthcare professionals, including nurses, pharmacists, physiotherapists, and occupational therapists, reflecting a broader acknowledgement of the need to distribute this responsibility and leverage diverse expertise.
The GP’s Ethical Tightrope: Advocate, Judge, or Target?

The hundreds of comments submitted by GPs alongside their questionnaire responses paint a vivid picture of the daily struggles. A recurring theme was the profound ethical and professional dilemma of being both a "patient’s advocate and a judge." This dual role is inherently problematic, creating an environment where the therapeutic relationship can be compromised. As one GP articulated, "Patients come for support – not to be dismissed," underscoring the conflict arising when a patient expects unconditional support for time off, while the doctor feels a responsibility to objectively assess the medical necessity and the system’s integrity. This conflict can erode trust and make genuine medical advice challenging to deliver.
The pressure to issue fit notes is not merely perceived; it often manifests in challenging patient encounters. GPs reported instances of patients becoming aggressive or refusing to leave the practice without a fit note. One doctor recounted a patient refusing to depart until their demand was met. Such situations force GPs into an untenable position, where safety and the desire to avoid conflict can override their professional judgment. "It would be insane to challenge the patient," admitted one respondent, while another highlighted the stark reality: "They argue and fight, we end up having to give in for our own safety." This reveals a disturbing dimension to the fit note process, where doctors may feel coerced into signing documents against their better medical opinion, often due to a lack of robust support systems for handling such confrontations.
The particular difficulty in refusing time off for mental health complaints was a prominent concern. Unlike physical ailments, which often present with observable symptoms or diagnostic markers, mental health conditions are inherently subjective. "Who am I to say I don’t believe that someone is struggling with their mental health? It’s not like a chest infection where there is definite proof of illness," one GP questioned. This difficulty in objective verification contributes significantly to the reluctance to refuse, as doctors grapple with the ethical implications of questioning a patient’s self-reported suffering, especially when a lack of external validation might be misconstrued as disbelief or insensitivity.
Perceptions, Cynicism, and the Path of Least Resistance
Amidst the collective frustration, there was a discernible divide in GPs’ attitudes towards patients seeking fit notes. While some expressed unequivocal trust in their patients’ honesty, believing that individuals would not seek time off unless genuinely unwell, a significant number conveyed cynicism, accusing patients of being "not genuine" or "milking the system." These differing perspectives underscore the complex interplay of individual doctor-patient relationships, prior experiences with perceived malingering, and broader societal views on work ethic and illness. Such cynicism, however understandable given the pressures, can further strain the doctor-patient relationship.
Several GPs also noted a perceived trend among younger adults being more likely to request time off work for mental health. One commented, "We sign off legions of young patients with anxiety and depression who are quite clearly not ill." While this observation requires further data validation, it might suggest evolving generational attitudes towards work, greater mental health literacy leading to more self-diagnosis and seeking help, or differing expectations regarding employer support and work-life balance compared to older generations. Without clear data, however, such perceptions risk reinforcing stereotypes.
Ultimately, for many GPs, the path of least resistance often prevails. Some openly admitted that signing a fit note was "not worth the grief" or "the hassle" of a prolonged argument or a formal complaint. The time and emotional toll of challenging a patient’s request, coupled with the administrative burden of dealing with subsequent complaints, often outweigh the perceived benefit of upholding a stricter standard. This pragmatic, albeit problematic, approach highlights a system that, in its current form, inadvertently incentivizes compliance over rigorous medical assessment, especially when doctors are already operating under immense time constraints and resource limitations, often with only 10-minute appointment slots.
Towards Systemic Reform: A Collaborative Future?
The growing recognition of these issues has prompted calls for significant reform. A government-commissioned report, "Keep Britain Working," published last year, explicitly labelled fit notes as "often problematic." The review highlighted that GPs frequently lack both the time and the specialized occupational health training required to comprehensively assess an individual’s fitness for work, or to advise effectively on workplace adjustments that could facilitate a quicker return. The report also cited compelling evidence: the longer a patient remains off sick, the less likely they are to ever return to work, with return rates plummeting from 96% after 4-6 weeks to just 50% after a year. This emphasizes the critical importance of early and appropriate intervention and the need for a system that actively promotes recovery and reintegration.
The Royal College of GPs (RCGP) has echoed these concerns, stating that family doctors may not always be "the most appropriate professionals" to provide long-term support for returning to work. While acknowledging the necessity of GPs issuing fit notes for shorter periods (up to three weeks) to address acute illness, the RCGP has expressed openness to exploring alternative models where responsibility for longer-term fit notes could be shifted to other, more specialized professionals or services, such as dedicated occupational health teams or multi-disciplinary panels with expertise in rehabilitation and workplace accommodations.
In response, the government has acknowledged the pressing need for reform, stating clearly that the current fit note system requires an overhaul and that new approaches are actively being tested to "build a system that works for everyone." Officials are reportedly exploring various options, including the development of "stay in/return to work" plans, which would involve closer collaboration between businesses, occupational health professionals, and potentially other healthcare providers. The aim is to create a more integrated and proactive system that supports employees in remaining in or returning to work safely and effectively, shifting the focus from simply signing people off to actively managing their health in relation to their work.
Jaguar Land Rover (JLR) offers a glimpse into a potential future model. As one of 60 companies collaborating with government officials on these new approaches, JLR has established six "centres of wellbeing" for its UK employees. These centres adopt a holistic, preventative approach, offering everything from exercise classes and NHS health checks to dedicated support for physiotherapy, counselling, and occupational health. Dr. Richard Peters, JLR’s chief medical officer, champions this employer-led model, asserting that firms have "a part to play" in supporting employee health. He highlights the mutual benefits: "It’s the right thing to do because if we have a healthier staff, then we have a more productive workforce," demonstrating a clear business case for investing in employee well-being.
However, scaling such initiatives across the entire economy presents significant challenges. Small businesses, in particular, face concerns regarding additional burdens. Tina McKenzie from the Federation of Small Businesses warned that proposals to make small businesses shoulder the cost of occupational health advice and fit notes would "add to these costs as well as piling on extra bureaucracy," potentially hindering their ability to implement supportive measures and exacerbating existing financial pressures. The forthcoming changes to statutory sick pay, which will require small businesses to pay from the first day of absence, further compound these concerns.
Furthermore, mental health charities urge caution. Tom Pollard, head of policy and campaigns at Mind, emphasized that any alternative system must be "approached with caution" and "built around trusting and compassionate relationships." He stressed the paramount importance of ensuring that individuals do not feel "forced to work when they don’t feel able to," highlighting the delicate balance between promoting work and safeguarding mental well-being, especially for those experiencing severe or complex mental health conditions.
The ongoing reform efforts signify a critical juncture for the UK’s healthcare and employment landscape. Addressing the GP fit note dilemma requires a comprehensive, collaborative approach that respects the expertise of medical professionals, prioritizes patient well-being, supports employers, and ultimately fosters a healthier, more productive workforce. The journey from a reactive, GP-centric system to a proactive, integrated model will undoubtedly be complex, but the imperative for thoughtful, comprehensive change is clearer than ever.
