"The proportion of American adults taking anxiety medications jumped from 11.7% in 2019 to 14.3% in 2024, an increase of 8 million people, with sharp rises seen among young adults, college graduates, and the LGBTQ+ community. This surge, largely occurring during the COVID-19 pandemic, is fueled by increased access, reduced stigma, and complex societal factors, even as debates continue regarding the safety and efficacy of certain psychiatric drugs."
The landscape of mental health treatment in the United States is undergoing a significant transformation, marked by a dramatic increase in the use of anxiety medications. This trend, accelerated by the widespread disruptions and stresses of the COVID-19 pandemic, reflects both evolving societal attitudes towards mental well-being and ongoing scientific and political discourse surrounding pharmacological interventions. While many individuals, like Sadia Zapp, a communications director who found relief from post-cancer treatment anxiety with Lexapro, report significant benefits, the rise in prescription rates has also ignited controversy. Critics, including prominent public figures, have raised concerns about the potential harms and addictive nature of these medications, particularly Selective Serotonin Reuptake Inhibitors (SSRIs), while medical professionals and researchers largely defend their safety and efficacy as front-line treatments.

Sadia Zapp, 40, experienced the profound impact of anxiety following a grueling year of chemotherapy, surgery, and radiation for breast cancer. The once manageable hum of daily stress escalated into a deep, distracting worry, where every physical sensation, like a knee ache, was interpreted as a harbinger of the end. This led her to join the growing ranks of Americans seeking pharmacological support, finding solace and stability in Lexapro, a serotonin-boosting SSRI. "I love it. It’s been great," Zapp shared. "It’s really helped me manage." Her experience mirrors that of millions, as the Centers for Disease Control and Prevention (CDC) reports a substantial increase in the prescription of anxiety medications.
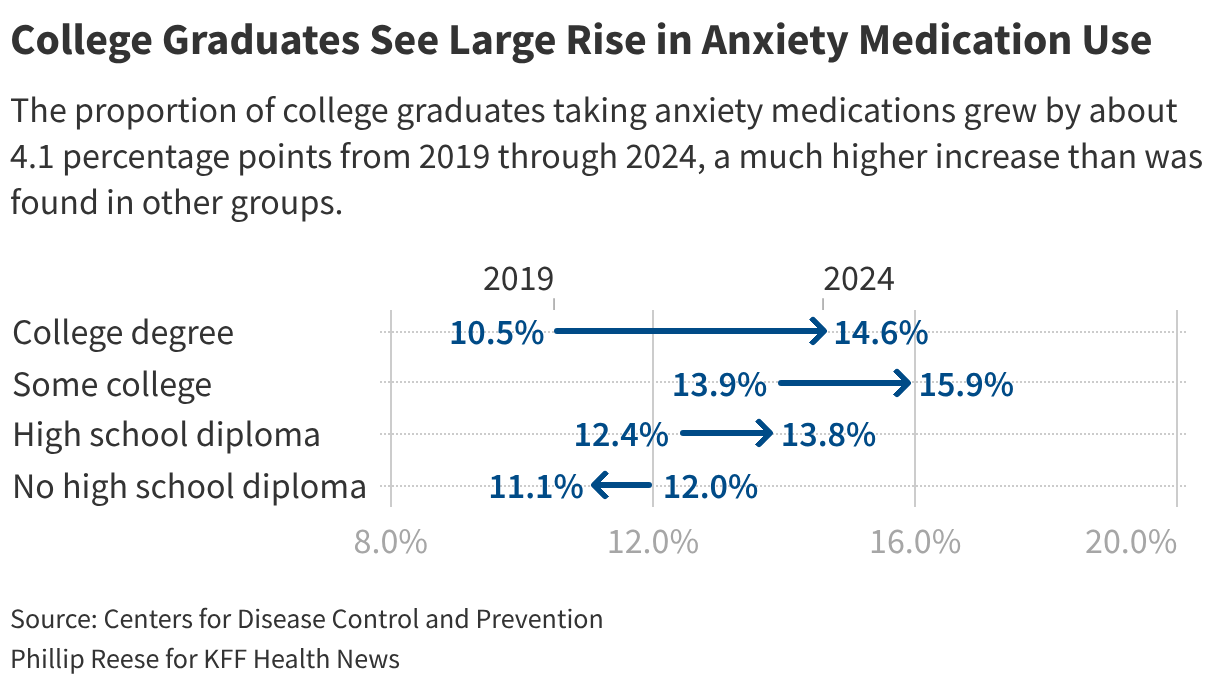
According to CDC survey data, the percentage of American adults taking anxiety medications climbed from 11.7% in 2019 to 14.3% in 2024. This translates to an additional 8 million individuals, bringing the total to approximately 38 million. The surge is particularly pronounced among specific demographics, including young adults, individuals with a college degree, and those identifying as LGBTQ+. This data highlights a significant demographic shift in the utilization of these treatments, suggesting that broader societal factors are influencing who is seeking and receiving care.
The increasing public acceptance and accessibility of psychiatric medications, facilitated in part by the expansion of telehealth services, have coincided with a growing debate about the role of SSRIs. Medications such as Prozac, Zoloft, and Lexapro are widely recognized by doctors and researchers as foundational treatments for various anxiety disorders, including generalized anxiety disorder and panic disorder. Despite evidence supporting their safety for long-term use, these SSRIs have faced criticism from a vocal segment of the "Make America Healthy Again" movement, who assert they are harmful and addictive.
This criticism has been amplified by public statements from influential figures. Health and Human Services Secretary Robert F. Kennedy Jr. has voiced strong opposition to the expanded use of SSRIs. During his confirmation hearing on January 29, he remarked that he knew individuals, including family members, who found discontinuing SSRIs more challenging than quitting heroin. More recently, he indicated that his agency is investigating a potential correlation between SSRI use, other psychiatric medications, and instances of violent behavior, such as school shootings. Similarly, Food and Drug Administration Commissioner Marty Makary has suggested that SSRI use during pregnancy could be linked to adverse birth outcomes.
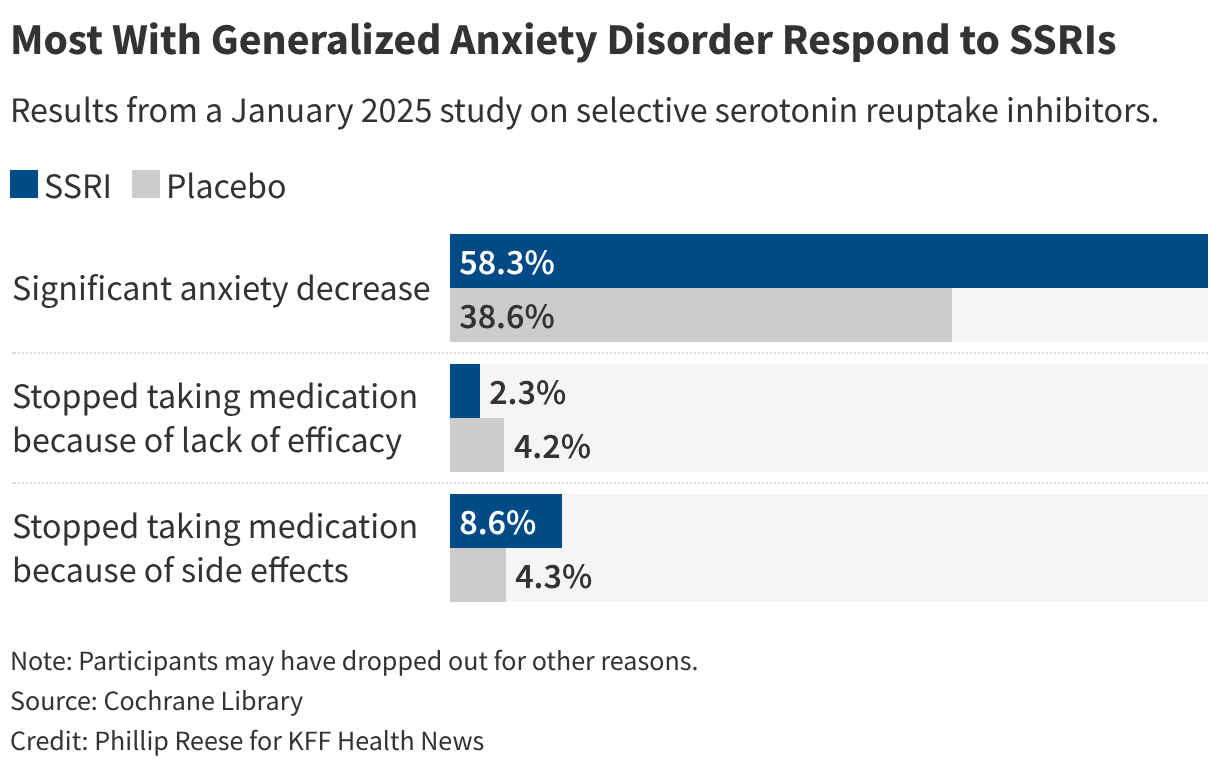
While these concerns are voiced, the medical community generally maintains a different perspective. Common side effects associated with SSRIs can include gastrointestinal upset, cognitive fogginess, and fatigue. Some individuals may also experience a reduced libido or other sexual side effects. However, for many, these side effects are manageable and outweighed by the significant benefits of treating chronic anxiety. Dr. Patrick Kelly, president of the Southern California Psychiatric Society, emphasized that the criticisms leveled against SSRIs are often not grounded in empirical evidence. He noted that a comprehensive Cochrane Review indicated that over half of individuals with generalized anxiety disorder experienced at least a 50% reduction in anxiety symptoms when taking an SSRI. Approximately one in twelve individuals discontinued SSRIs due to side effects, a figure that underscores the generally tolerable nature of these medications for the majority of users.
Dr. Emily Wood, a psychiatrist practicing in Los Angeles, underscored the importance of appropriate clinical management, stating, "When it’s being done right and when you’re also using appropriate therapy techniques, SSRIs can be really, really helpful." She further highlighted that while healthy lifestyle choices like a balanced diet and regular exercise are encouraged as adjunctive therapies for anxiety and depression, medication remains a critical tool for many. The utilization of mental health counseling also saw a significant boom between 2019 and 2024, with teletherapy playing a crucial role in increased access. Wood specifically noted that "Anxiety disorders are amongst our psychiatric disorders that really respond well to cognitive behavioral therapy."
However, the debate intensifies when considering the use of SSRIs during pregnancy. While studies generally indicate low risks for both mother and child, the pronouncements from government officials have raised concerns among clinicians like Dr. Wood, who fear they could inadvertently lead to harm by discouraging necessary treatment for pregnant women experiencing depression, a condition known to increase maternal and infant complications.
The discussion around addiction is also a point of contention. While benzodiazepines, such as Xanax, which are often prescribed as a second-line treatment for acute anxiety, carry a risk of dependence and can be challenging to discontinue, the concept of addiction does not accurately apply to SSRIs. Dr. Kelly clarified that studies support the assertion that SSRIs are not addictive in the same manner as substances like benzodiazepines. Discontinuation symptoms, such as nausea or insomnia, can occur if SSRIs are stopped abruptly, but this is distinct from addiction.
Beyond SSRIs, other medications are also being utilized for anxiety. Benzodiazepines, while effective for short-term management of acute anxiety, require careful monitoring due to their potential for habituation and the risk of opioid overdose when taken concurrently with opioids. Dr. Wood cautioned that these medications are not ideal for long-term daily use, as tolerance can develop, necessitating higher doses and a carefully managed tapering process for discontinuation. Additionally, beta-blockers like propranolol are increasingly being used "off-label" to manage the physical symptoms of anxiety, such as a racing heart, particularly in performance-related situations. While beta-blockers can cause side effects like dizziness and fatigue, they are considered nonaddictive and can be effective in calming the autonomic nervous system.

Several theories attempt to explain the significant rise in anxiety medication use. Physicians and researchers point to factors such as increased social media engagement, greater social isolation, and heightened economic uncertainty. The COVID-19 pandemic, with its associated lockdowns and disruptions, undoubtedly exacerbated stress levels for many, particularly young adults. Telehealth has also made it easier to obtain prescriptions, with many primary care physicians and even brief teletherapy appointments leading to SSRI or benzodiazepine prescriptions.
Social media itself plays a dual role. While influencers openly discussing their mental health struggles can help destigmatize seeking help among younger generations, it also contributes to a trend of self-diagnosis based on online information. This can be problematic, especially when coupled with the ease of searching for online pharmacies that may offer medications without a guaranteed prescription.
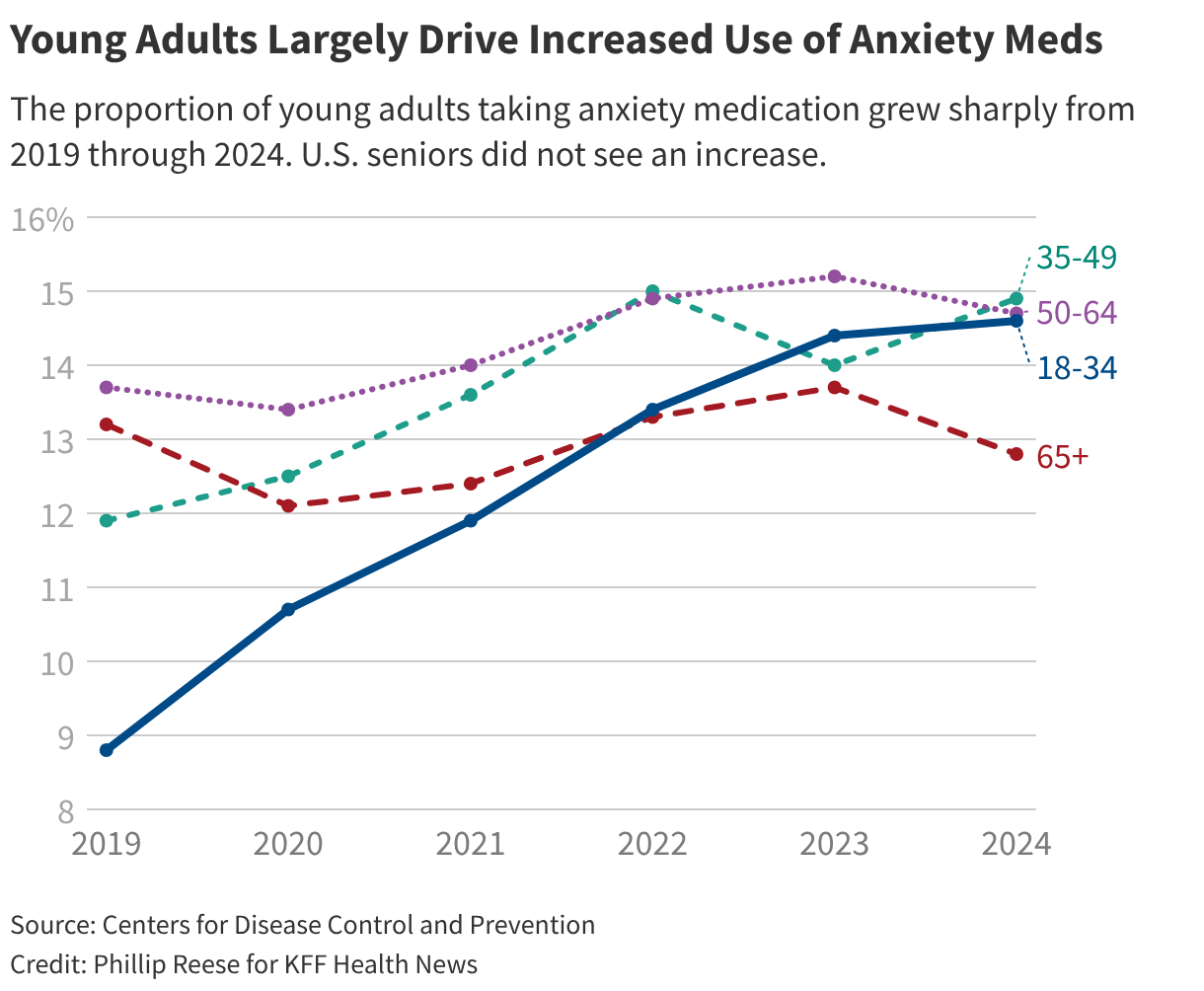
Demographic data reveals that young adults are a driving force behind the increased use of anxiety medication. The proportion of Americans aged 18 to 34 using these medications rose from 8.8% in 2019 to 14.6% in 2024. In contrast, the rate remained relatively stable among adults aged 65 and older. This generational difference suggests that younger cohorts may be more open to seeking pharmacological help or are experiencing higher levels of anxiety due to unique societal pressures.
The data also indicates that women are more likely than men to take anxiety medication. Sociologist Jason Schnittker, author of "Unnerved: Anxiety, Social Change, and the Transformation of Modern Mental Health," suggests this is due to women being more likely to require such treatment and more inclined to report their anxiety symptoms. He also notes that clinicians may be more attuned to recognizing anxiety in female patients. Schnittker posits that broader societal trends, including growing income inequality, increased social isolation, and a decline in communal activities, have contributed to a pervasive sense of unease and anxiety across generations.
For Sadia Zapp, the journey to managing her anxiety was not instantaneous. It took several months on Lexapro to experience noticeable relief, after which her mind felt quieter, allowing for improved focus. While she also engaged in talk therapy, her chronic anxiety is now effectively managed by medication alone. "It definitely helped me get back to my day-to-day in a way that was productive and not just riddled with my anxieties throughout the day," she concluded. Her experience highlights the potential for medication to be a crucial component in reclaiming a functional and fulfilling life amidst significant personal challenges.
