"Despite an ‘opt-out’ organ donation system designed to save hundreds of lives annually, a crucial ‘fatal flaw’ allows families to veto a loved one’s wishes, leaving over 8,000 people in the UK in a desperate, life-threatening wait for a transplant. Open family conversations are now more critical than ever to bridge this gap between presumed consent and actual donation."
The introduction of an "opt-out" organ donation system in England in 2020, following Wales’ lead, was heralded as a progressive step poised to significantly boost the number of available organs and save countless lives. Yet, nearly four years on, the UK faces an unprecedented crisis: a record high of over 8,000 individuals are languishing on organ transplant waiting lists, while donor consent rates stagnate. The stark reality reveals a critical disconnect between presumed consent and the final act of donation, largely due to families exercising their right to override a deceased loved one’s registered wishes. This "fatal flaw," as described by long-standing campaigners, underscores the urgent need for frank discussions within families, highlighting that a signed register entry alone may not be enough to ensure a legacy of life.
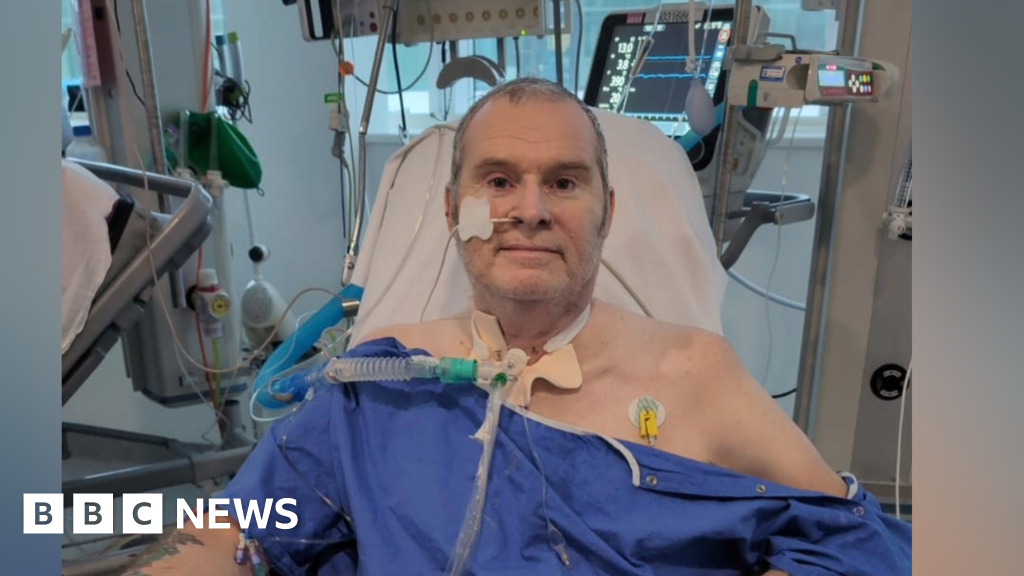
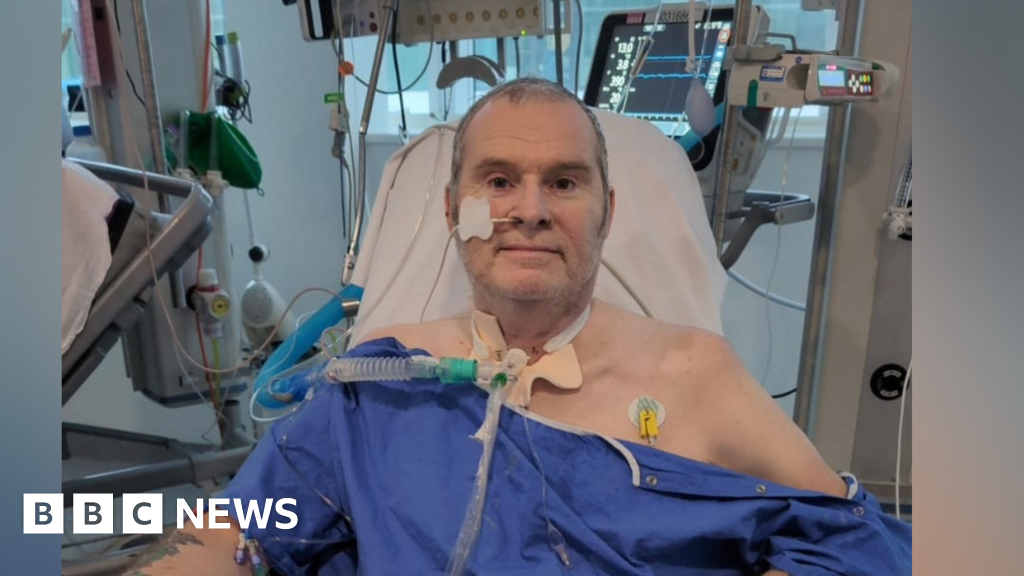
For Matthew Smith, a resident of Wednesbury in the West Midlands, every dawn for nearly a year brought with it a profound, anxiety-inducing question: "Is today going to be the day we get that call?" Diagnosed with a terminal lung condition in 2023, Matthew’s life, and that of his wife Nicola, became a relentless vigil. Tethered to oxygen tanks, his existence revolved around the desperate hope for a double lung transplant, the only viable path to survival. Nicola vividly recalls the sleepless nights, frequently checking her phone, terrified of missing the life-altering notification. Their 10-month ordeal, a period marked by profound uncertainty and deteriorating health, culminated in that longed-for call, granting Matthew a second chance at life. However, Matthew’s story, while ultimately hopeful, casts a stark light on the broader national challenge, where the journey to a transplant is fraught with increasing delays and despair for many.
The national organ donation landscape is currently facing a critical imbalance. While the demand for life-saving organs has soared to an all-time high, the rate at which donations are actually proceeding has remained stubbornly flat. This disparity is particularly acute in regions like the West Midlands, where over 500 individuals are in urgent need of a vital organ. The primary impediment to increasing donation rates, even under an "opt-out" system, is the power of family veto. Despite an individual explicitly registering their consent to donate their organs after death, or falling under the presumed consent of the opt-out law, family members retain the legal right to refuse permission. This often places medical professionals in an incredibly sensitive and challenging position, caught between the wishes of the deceased and the immediate grief and conflicting perspectives of their next of kin.
The "opt-out" system, officially known as Max and Keira’s Law in England, was implemented in May 2020, building upon Wales’ pioneering introduction five years earlier. The core principle of this system is that all adults are presumed to consent to organ donation unless they have explicitly recorded a decision to opt out. When it was proposed, Theresa May’s government in 2018 optimistically estimated that this shift could lead to saving up to 700 additional lives each year. The intention was to simplify the donation process and increase the pool of potential donors by removing the inertia of individuals not signing up to a register. However, the subsequent reality has revealed that presumed consent does not automatically translate into actual donations when families intervene.
Reasons cited by families for blocking donations are complex and deeply personal, often stemming from profound grief and difficult circumstances. These can include a lack of clear communication from the deceased regarding their wishes, leading to uncertainty for the family at a time of immense emotional distress. Some families express discomfort with the perceived length or invasiveness of the donation process, or the notion of further surgery to a loved one’s body after death. Furthermore, deeply held religious or cultural beliefs can play a significant role, with certain faiths or traditions holding specific views on bodily integrity after death, which may not align with organ donation. These deeply personal considerations highlight the importance of not just legal frameworks, but also robust societal conversations and clear individual expressions of intent.
Christine Cox MBE, a formidable campaigner from Wolverhampton, has dedicated over 35 years to advocating for organ donation, a mission ignited by personal tragedy. Her brother, Peter, died from a brain tumour in 1989 at the tender age of 24. While no organ could save Peter’s life, his final, selfless wish was that his life should benefit others. This profound act of generosity resulted in 17 individuals receiving life-saving organs. Peter’s dying words, "it was our duty to ensure that as many organs as possible could benefit others," became Christine’s enduring mantra. In the wake of Peter’s death, Christine and her parents discovered a critical systemic flaw: there was no centralised list for individuals willing to donate. Donation then relied entirely on physical donor cards, which were often not carried or easily accessible, creating significant barriers for medical staff. This experience spurred Christine into relentless campaigning, eventually leading to the establishment of the UK’s first national Organ Donor Register in 1994, a monumental achievement that transformed the landscape of donation.

Having witnessed the evolution of organ donation policy, Christine initially welcomed the introduction of the opt-out system with immense hope. However, her enthusiasm has since been tempered by the realisation of what she terms the "fatal flaw"—the ability of next of kin to override a registered or presumed consent. For Christine, this loophole undermines the very spirit of the law and the wishes of potential donors. Her current focus, therefore, is not just on registering intent but on fostering open, honest dialogue within families. "I implore everybody not just to make their wishes known but to talk to their friends and their family and also find out what their friends and family want," she urges. "It possibly will never happen however everyone needs to know what your wishes are." This emphasis on discussion is rooted in the understanding that when families are aware of a loved one’s decision, they are far more likely to honour it, even in the depths of grief.
The importance of these crucial family discussions is strongly echoed by the NHS, which recently launched its "Hope Takes Flight" campaign, specifically urging families to communicate about organ donation before it’s too late. Harpreet Matharu, an organ donation specialist nurse for the NHS, explains the practical impact: "What we’ve always said is talk to your loved one, make a decision and sign on the register, because we know when a patient has opted in and had those conversations, consent is much higher in those circumstances." This highlights a significant disparity: while the opt-out system creates a default of consent, informed consent, backed by family awareness, leads to far better outcomes in terms of actual donations.

Matharu also addresses common hesitations and misconceptions, particularly the "squeamishness" some people feel about the process. She stresses the importance of understanding the factual realities of donation, reassuring potential donors and their families that the process is handled with the utmost dignity and respect. "When you donate, you are looked after with the upmost respect in hospitals and all your religious and cultural needs are still catered for," she states. Furthermore, specialist nurses like Matharu play a vital role in supporting donor families through their grief, often highlighting how the act of donation can provide a profound sense of comfort and meaning, transforming tragedy into a lasting legacy of hope and life for others. For many grieving families, knowing their loved one has saved lives can be an integral part of their healing process.
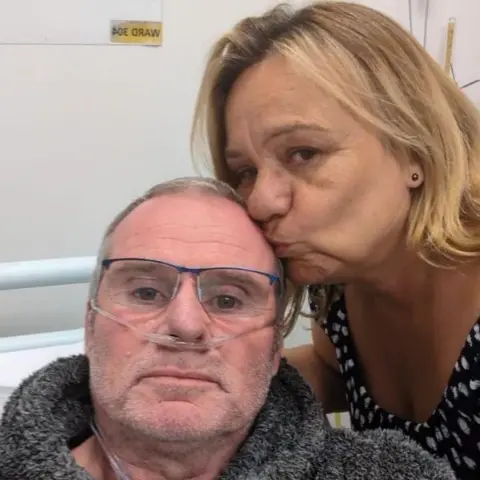
For Matthew and Nicola Smith, the day of the transplant was a crucible of emotions. "I think I cried from when he went in until he came out. It’s the start of a new beginning. It’s a new life," Nicola reflects. The arduous wait, the daily struggle for breath, and the constant fear of the future have given way to a profound sense of renewal. Matthew can now participate in activities that were once unimaginable, no longer confined by the limitations of his failing lungs. The couple now cherishes plans to renew their vows on their 30th wedding anniversary this year, on a sun-drenched beach in Cornwall – a testament to the transformative power of organ donation.

Nicola’s experience has instilled in her a fervent belief in the importance of organ donation, urging others to seriously consider the profound impact they can have. "You’re giving somebody the chance of a new future, to live a good, long life. To make memories," she passionately states. Her words encapsulate the essence of the organ donation debate: it is not merely about medical procedures, but about extending the precious gift of life, enabling individuals to create new memories, pursue dreams, and share more moments with their loved ones.
The current crisis in organ donation serves as a powerful reminder that legislative changes, while important, are only one part of the solution. The human element—the willingness to discuss, understand, and respect end-of-life wishes—remains paramount. To truly unlock the life-saving potential of the opt-out system and reduce the heartbreaking numbers on waiting lists, a cultural shift towards open family dialogue about organ donation is essential. Only then can the gap between presumed consent and the ultimate act of generosity be bridged, ensuring that more individuals like Matthew Smith receive their much-needed second chance at life.