"This specialized shelter offers not just a roof, but a lifeline of medical support and dignity for seniors facing homelessness, a demographic increasingly overlooked by traditional services."
Nestled in Sandy, Utah, just outside the bustling metropolis of Salt Lake City, an unassuming two-story brick building has been transformed into a beacon of hope for the community’s most vulnerable seniors. This former hotel has been reborn as the Medically Vulnerable People (MVP) shelter, a facility specifically designed to address the complex needs of individuals aged 62 and older experiencing homelessness, as well as younger adults grappling with chronic health conditions. The MVP shelter represents a critical shift in how we approach homelessness, recognizing that age and chronic illness necessitate a level of care far beyond what conventional shelters can provide. Its innovative model offers a glimpse into a future where compassionate, medically informed support becomes the standard for a growing segment of the unhoused population.
The challenges faced by seniors experiencing homelessness are multifaceted and often exacerbated by their age and health status. Unlike the dormitory-style accommodations and limited facilities typical of many homeless shelters, the MVP shelter prioritizes resident comfort and dignity. Rooms are designed with accessibility in mind, catering to individuals with mobility issues. The provision of private bathrooms is a particularly significant amenity, offering much-needed privacy and addressing common health concerns such as incontinence, which can be a source of profound embarrassment and distress in shared living environments.
Dennis Culhane, a researcher at the University of Pennsylvania, highlights a sobering national trend: seniors are the fastest-growing demographic among the homeless population. This increase is driven by a dual phenomenon. Firstly, individuals who have experienced chronic homelessness for years are now aging, bringing with them a lifetime of accumulated health challenges. Secondly, and perhaps more alarmingly, a growing number of older adults are finding themselves homeless for the first time in their lives, often due to economic instability, health crises, or the loss of social support systems.
The inherent difficulties of traditional shelter life can be particularly daunting for older adults. Simple tasks such as navigating bunk beds, managing complex medication schedules, and accessing shared bathrooms in a timely manner can become insurmountable obstacles. In some cases, staff at conventional shelters, lacking the resources or training to adequately support these needs, may feel compelled to ask seniors to leave, further marginalizing an already vulnerable group. The MVP shelter stands in stark contrast, distinguishing itself by offering on-site medical care, a crucial element in supporting residents as they age and their health needs evolve.

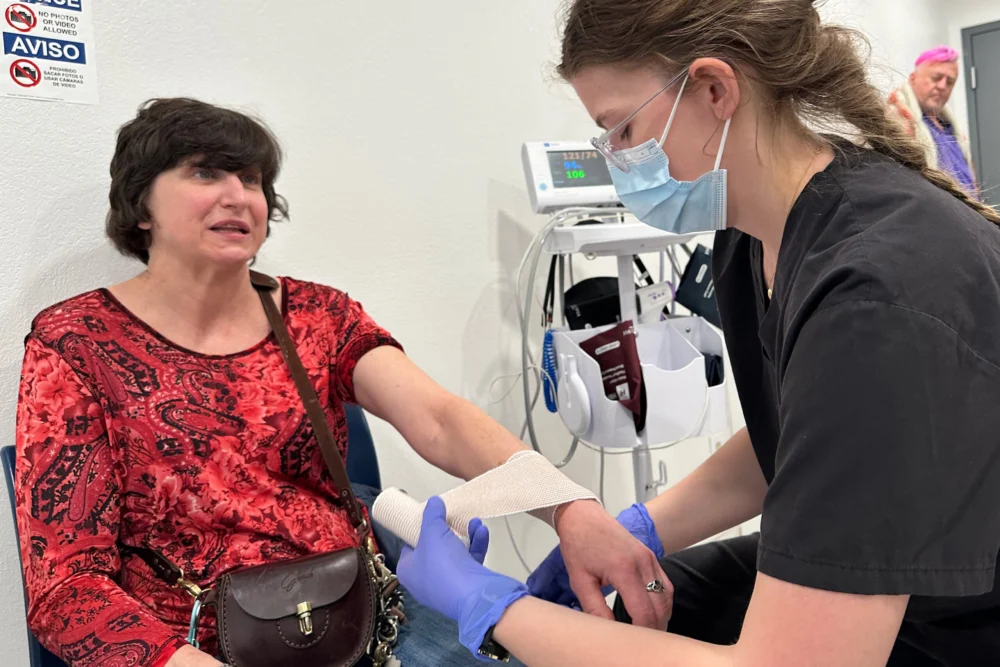
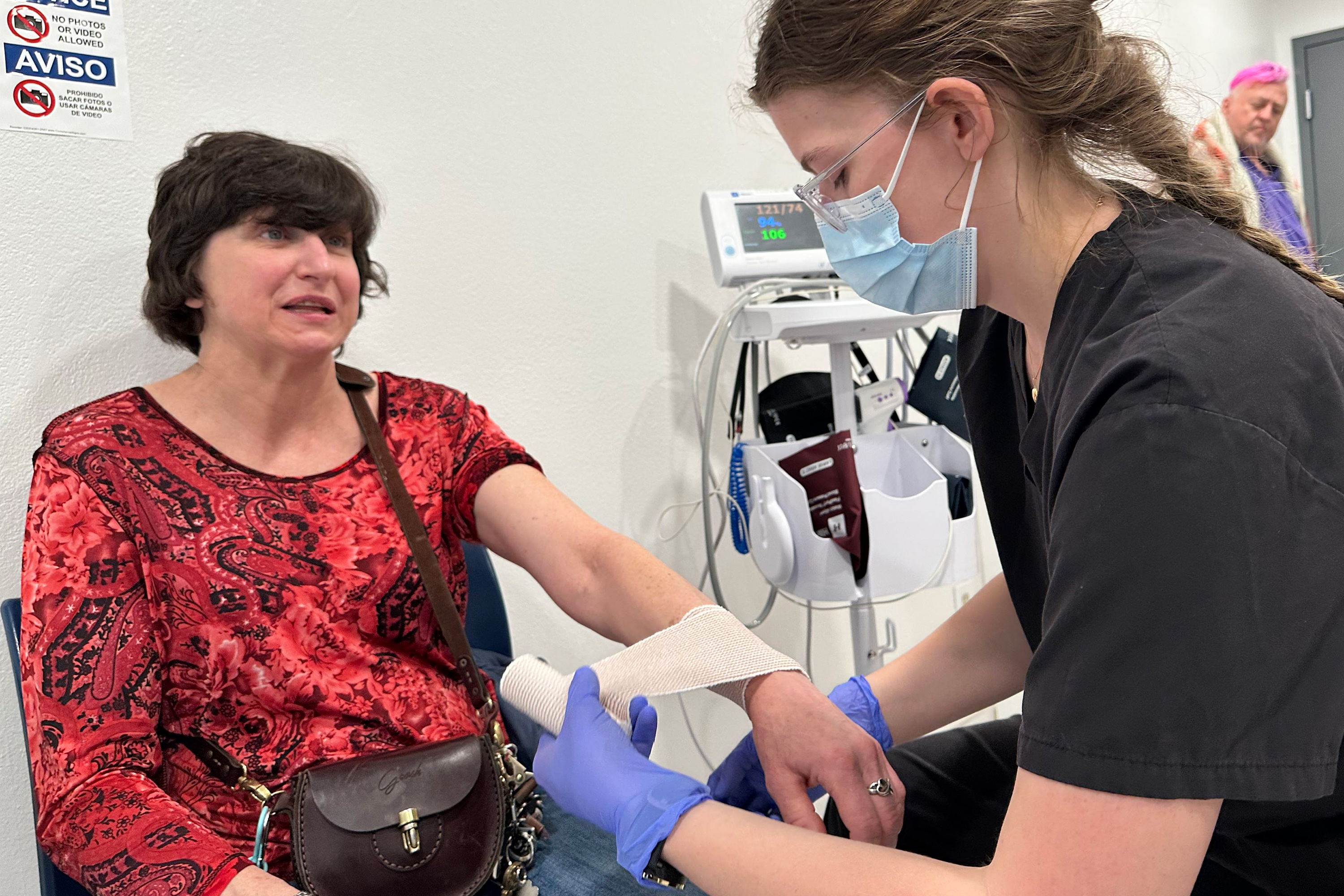
Jamie Mangum, a woman in her 50s battling lung cancer, experienced firsthand the life-altering impact of the MVP’s integrated medical services. After a fall in her room, she needed only to descend one floor to receive immediate attention from an on-site emergency medical technician. Her swollen wrist was swiftly treated, allowing her to return to her room without the arduous process of seeking external medical care. "There, I’d have to wait hours as opposed to come in here, be seen," Mangum stated, emphasizing the immediate and accessible nature of care at the MVP. Without such readily available support, she would have faced significant challenges in arranging transportation to an urgent care facility or calling for an ambulance. Beyond immediate medical needs, the specialized case managers at the MVP have also been instrumental in helping Mangum navigate her lung cancer treatment.
Baleigh Dellos, manager of the MVP shelter for The Road Home, a local nonprofit, elaborated on the diverse needs of their residents. "We have clients that need memory care. Maybe they were living independently before, but they were unable to maintain that and got evicted due to dementia or different things like that," she explained. This highlights the critical role of specialized support for seniors experiencing cognitive decline, a condition that can rapidly escalate into housing instability. The MVP’s model acknowledges these complex realities, providing a safe and supportive environment for individuals who might otherwise be lost in the system.
The shelter’s comprehensive approach to care is facilitated by a team of specialized medical case managers who work directly with residents. Furthermore, primary care physicians and therapists conduct weekly visits, and residents can even access physical therapy services in private, on-site spaces. This integrated model ensures that a spectrum of medical needs can be addressed without requiring residents to navigate the often-complex and inaccessible external healthcare system.
The partnership with the Fourth Street Clinic is central to the MVP’s success in delivering essential medical services. Matt Haroldsen from the Fourth Street Clinic noted that a primary challenge for new residents is regaining control over their medications. "Their medications get jacked when they’re in their camps," he stated, referring to the difficulties of securely storing and accessing vital prescriptions while living unsheltered. For individuals with chronic conditions like diabetes, maintaining the cold chain for insulin can be a life-threatening struggle; forgetting where it was buried or the risk of spoilage due to improper storage are common hurdles. By providing a stable environment and assistance with medication management, the MVP shelter stabilizes residents’ health conditions, freeing them to focus on other critical steps toward self-sufficiency, such as obtaining identification and vital documents necessary for applying for disability benefits, Social Security, and various housing programs.
The innovative MVP model is not isolated to Utah. Similar specialized shelters are emerging in states like Florida, California, and Arizona, demonstrating a growing recognition of the unique needs of older unhoused adults. Caitlin Synovec, assistant director of the National Health Care for the Homeless Council, underscores the life-saving potential of these tailored facilities. "Having access to specialized shelters can be the difference between life and death," she asserted. In colder climates, the risks for seniors with mobility and health issues are particularly acute. Synovec recounted a tragic incident in Bozeman, Montana, where a senior died from hypothermia in 2022 after being asked to leave a shelter due to incontinence.
The complexities of medical needs can also pose safety risks in traditional shelters, which are often ill-equipped to manage them. "A typical shelter doesn’t allow somebody on oxygen to come in because that’s such a fire hazard and risk," Synovec explained. By providing specialized care within a controlled environment, the MVP and similar facilities mitigate these risks, ensuring the safety of both residents and staff. Synovec further emphasizes that integrating healthcare access within shelters is paramount to helping seniors achieve stable housing. Health issues are frequently cited as a primary barrier preventing seniors from affording or maintaining housing.
The MVP model’s effectiveness is increasingly evident. Jacob Torner, vice president of programs for the TaskForce for Ending Homelessness in Fort Lauderdale, Florida, reported that over 80% of residents at their Elder Haven shelter have transitioned into stable or permanent housing within the past year. Locally, the MVP shelter near Salt Lake City has also demonstrated significant success, permanently housing 36 seniors by late last year.
Despite these successes, the demand for such specialized services far outstrips the available resources. Dellos, the MVP shelter manager, indicated that the waitlist typically hovers around 200 individuals. The shelter prioritizes applicants based on their medical urgency, rather than the length of time they have been on the waitlist, ensuring that those with the most critical needs receive prompt attention.
For those who secure a place at the MVP shelter, the impact is profound and life-changing. Jeff Gregg, a 62-year-old resident, shared his journey from chronic pain and opioid addiction to a path of recovery and hope. An old back injury had fueled a decades-long struggle with addiction, a cycle he found nearly impossible to break while simultaneously facing the daily challenges of homelessness. "Fighting that, having a job, insurance, then losing the job, not having insurance, going out to the streets and being back in that crap, and I’d be back in the same position," Gregg recounted, illustrating the precariousness of his situation.
Gregg explained that his immediate survival needs—finding food and shelter—often overshadowed his efforts toward sobriety. The MVP shelter provided him with the stability and support necessary to finally prioritize his recovery. "I was able to get clean. It took me a couple months, but I just kept plucking away," he said. This newfound stability paved the way for him to undergo back surgery, a procedure he hopes will alleviate his chronic pain and enable him to secure employment and eventually afford an apartment. His story, like many others at the MVP shelter, underscores the transformative power of specialized care that addresses both the immediate and long-term needs of aging individuals experiencing homelessness.
The burgeoning success of facilities like the MVP shelter near Salt Lake City, and initiatives such as Elder Haven in Florida, signals a growing understanding and commitment to serving this vulnerable population. As the number of seniors experiencing homelessness continues to rise, the development and expansion of such medically informed and compassionate shelters will be crucial in providing a pathway toward dignity, health, and lasting stability.