"Anthony Perriam’s near-fatal battle with HPV-related head and neck cancer underscores the urgent need for greater public awareness and vigilance, especially among men, about this often-overlooked disease and the life-saving potential of early diagnosis and the HPV vaccine."
A father-of-two from Cardiff, Anthony Perriam, faced a harrowing cancer diagnosis that began with a seemingly innocuous lump under his jaw. His experience sheds a stark light on the insidious nature of Human Papillomavirus (HPV) and its lesser-known but increasingly prevalent link to head and neck cancers in men. What many associate primarily with cervical cancer in women, HPV can manifest in various forms, and Perriam’s ordeal serves as a critical public health warning, emphasizing the vital importance of early detection and the widespread uptake of the HPV vaccination program.

Anthony Perriam’s journey into the clutches of cancer commenced with an unsettling discovery: a small, painless lump beneath his jaw. With no other discernible symptoms, the 41-year-old father, like many, harbored no immediate concerns, unaware of the silent threat lurking beneath the surface. His perception of HPV, confined solely to its association with cervical cancer, reflected a common public misconception. "I’d only ever heard of HPV in relation to cervical cancer," Anthony recounted, expressing his shock. "I had no idea it could cause cancers like this, especially in men." This lack of awareness underscores a significant gap in public health discourse surrounding HPV’s broader oncogenic potential.
In March 2023, Perriam’s initial complacency shattered following a series of diagnostic tests, including a CT scan, biopsy, and MRI, which unequivocally confirmed the presence of cancer. The diagnosis sent shockwaves through his family. With a three-year-old and a six-year-old at home, his immediate thoughts were not of his own mortality but of their future. "My first thought wasn’t about me, it was about them. I was completely petrified for them," he shared, articulating the profound fear that grips parents facing life-threatening illnesses. The tumour was eventually located at the base of his tongue, a common site for HPV-associated oropharyngeal cancer.
HPV, a widespread group of viruses, typically manifests as skin infections and often clears from the body without intervention. However, certain high-risk strains of the virus can persist, leading to cellular changes that may progress to cancer over time. While most commonly recognized for its role in cervical cancer, HPV is increasingly implicated in a range of other malignancies, including anal, penile, vulvar, vaginal, and notably, head and neck cancers, particularly those affecting the oropharynx (the back of the throat, including the base of the tongue, tonsils, and soft palate). The Centers for Disease Control and Prevention (CDC) notes that HPV causes about 70% of oropharyngeal cancers in the United States, a trend observed globally, highlighting a shifting landscape in cancer epidemiology.

Anthony’s treatment regimen was aggressive and gruelling. Surgeons performed a radical neck dissection, removing 44 lymph nodes from his neck in a bid to halt the cancer’s spread. The primary tumour at the base of his tongue was excised using robotic-assisted surgery, a less invasive technique known as Transoral Robotic Surgery (TORS), which allows for precise removal of tumours in hard-to-reach areas, often preserving more healthy tissue than traditional open surgery. "They told me they caught it just in time," Anthony revealed, emphasizing the critical timing of his diagnosis and intervention. Doctors informed him that one of the removed lymph nodes was "on the verge of rupturing," a terrifying prospect that could have led to widespread metastasis had the cancer progressed further.
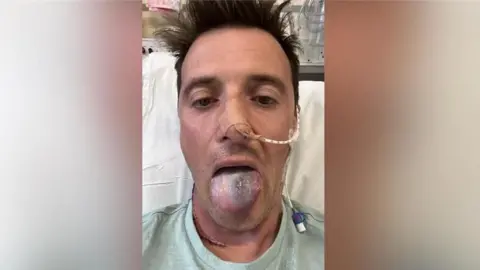
The subsequent rounds of radiotherapy and chemotherapy pushed Anthony’s physical and mental endurance to its limits. He experienced severe side effects, losing a staggering 22kg (48.5 lbs) in weight. The radiotherapy, targeting the head and neck region, ravaged his salivary glands, leading to debilitating dry mouth (xerostomia). "All of my saliva disappeared," he described, explaining how even drinking became an arduous task as everything "turned to powder in my mouth." The cumulative toll of treatment rendered him profoundly weak, necessitating the use of a wheelchair. Beyond the physical agony, the constant barrage of medical procedures and his deteriorating condition took a significant toll on his mental well-being. "Being wheeled down the corridor and into radiotherapy was starting to affect my mental health," he admitted. Yet, amidst the despair, his family provided an unwavering beacon of hope. "My family gave me the motivation to get through it, and I wanted to live to see my 40th birthday." This personal goal, driven by love and a desire to witness future milestones, became a powerful catalyst for his resilience.
Anthony Perriam’s journey serves as a powerful testament to the critical importance of early detection. His plea, "If you find a lump, even if it doesn’t hurt, get it checked," resonates with medical professionals globally. Head and neck cancers, particularly those linked to HPV, can present with subtle, often painless symptoms, making self-awareness and prompt medical consultation paramount. Other potential indicators might include a persistent sore throat, difficulty swallowing (dysphagia), voice changes, unexplained weight loss, or a non-healing mouth sore. Early diagnosis dramatically improves prognosis, often allowing for less aggressive treatments and a higher chance of a cure. Conversely, delayed diagnosis can lead to more advanced disease, requiring extensive surgery, radiotherapy, and chemotherapy, with a higher risk of recurrence and poorer outcomes, as Anthony’s close call vividly illustrates.
Understanding and leveraging the HPV vaccine is another cornerstone of prevention. NHS Wales, in line with national recommendations, offers the HPV vaccine to children aged 12 and 13, recognizing this age as optimal for developing a robust immune response before potential exposure to the virus. The vaccine, which has been part of a national immunisation program since 2008, has demonstrably reduced cervical cancer rates by almost 90% in women in their 20s, according to University Hospital of Wales. This success story highlights the vaccine’s transformative public health impact.
Sandeep Berry, a consultant otolaryngologist head and neck surgeon at Cardiff and Vale health board, passionately advocates for the vaccine’s uptake. "The HPV vaccine has been used worldwide for years; it’s safe and effective and is part of the national immunisation programme in Wales," he affirmed. He emphasized its comprehensive benefits: "It helps boys and girls stay healthy, prevents HPV-related cancer, and strengthens public health overall." The rationale for vaccinating adolescents in Year 8 is strategic, aligning with a period when the immune system is most responsive and typically precedes the onset of sexual activity, thus maximizing protection.
The expansion of the HPV vaccination program to include boys alongside girls has been a crucial development in combating HPV-related cancers comprehensively. This inclusive approach not only protects boys from cancers like oropharyngeal, anal, and penile cancers but also contributes to herd immunity, further reducing the circulation of the virus within the population and protecting unvaccinated individuals.

Anthony Perriam’s courageous sharing of his experience is a clarion call for increased public and medical community awareness. "This kind of cancer isn’t talked about enough, especially among men. Early action really does save lives," he asserted. His story serves as a potent reminder that while HPV is common, its potential to cause life-threatening cancers, particularly in the head and neck, is a reality that demands attention. Through continued public education, robust vaccination programs, and a collective commitment to early detection, the severe outcomes associated with HPV-related cancers can be significantly mitigated, ultimately saving lives and improving public health for generations to come.
