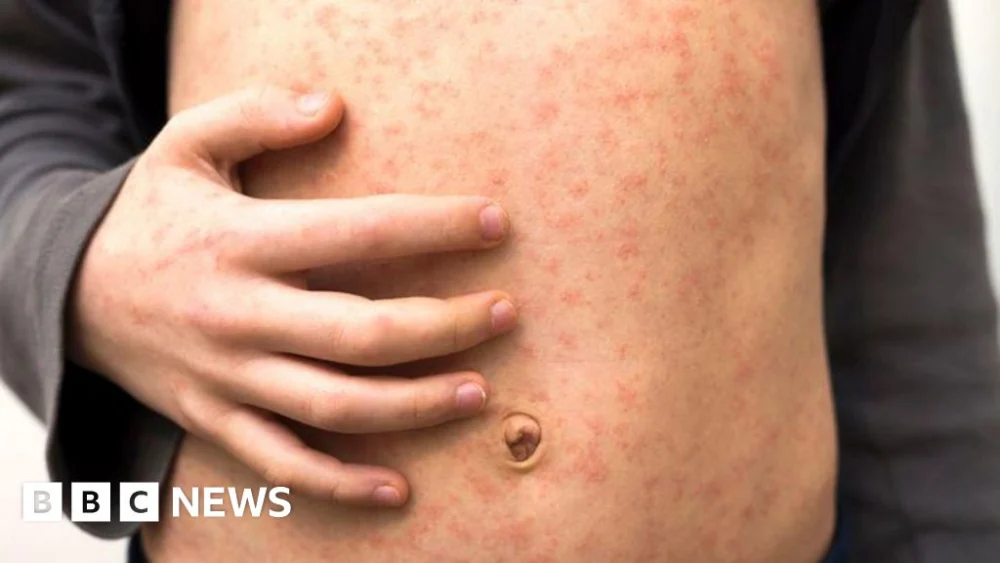
A "fast-spreading" measles outbreak has infected at least 34 children across multiple schools in North London, with alarming reports that one in five affected children required hospitalisation, all of whom were not fully immunised. This resurgence underscores the severe public health risk posed by declining vaccination rates, pushing the UK further from its target of measles elimination.
The recent outbreak in London’s Enfield and Haringey boroughs highlights a critical vulnerability in community immunity, with confirmed measles cases rapidly propagating through school environments. Health officials are sounding the alarm, emphasizing that this highly contagious disease, once considered largely eradicated in the UK, is making a dangerous comeback due to insufficient uptake of the Measles, Mumps, and Rubella (MMR) vaccine. The situation serves as a stark reminder of measles’ capacity to cause serious health complications, necessitating urgent action from families and public health bodies to prevent a wider epidemic.
An Alarming Resurgence in North London
Confirmed laboratory tests in January revealed a "fast-spreading" measles outbreak primarily affecting children in several North London schools. The UK Health Security Agency (UKHSA) reported at least 34 children have been infected, concentrated within the boroughs of Enfield and neighbouring Haringey. The severity of this outbreak is particularly concerning, with a local GP surgery, the NHS Ordnance Unity Centre For Health, stating that a distressing one in five children who contracted the illness required hospital admission. Critically, all hospitalised cases involved individuals who had not received their full course of immunisation against the disease.
Enfield Councillor Alev Cazimoglu confirmed that the outbreak had "mainly affected children and some have required additional care with a short stay in hospital," reinforcing the urgent need for preventative measures. This cluster of cases serves as a tangible demonstration of how quickly measles can take hold and escalate in communities with suboptimal vaccination coverage.
The Unseen Threat: Why Measles Poses a Serious Danger
Measles is far more than a simple childhood rash; it is a highly contagious and potentially devastating illness. The virus spreads with remarkable ease, primarily through respiratory droplets released when an infected person coughs or sneezes. Its airborne nature means it can linger in the air for up to two hours after an infected person has left a room, making transmission incredibly efficient. This high transmissibility (often cited with an R0 value between 12 and 18 in unvaccinated populations) necessitates a very high level of community immunity to prevent widespread outbreaks.
The health complications associated with measles are significant and can be life-threatening. While many experience fever, cough, runny nose, red eyes, and a characteristic rash, a substantial proportion can develop severe complications. These include pneumonia (the most common cause of measles-related death in young children), encephalitis (inflammation of the brain, which can lead to permanent brain damage, deafness, or intellectual disability), and ear infections that can result in permanent hearing loss. In rare but tragic cases, a condition known as subacute sclerosing panencephalitis (SSPE) can develop years after the initial infection, leading to progressive neurological deterioration and eventual death. Pregnant women who contract measles face risks of miscarriage, premature birth, and low birth weight. The high hospitalisation rate observed in North London underscores the serious nature of this preventable disease.
The Critical Role of Vaccination and Declining Uptake
The cornerstone of protection against measles is the Measles, Mumps, and Rubella (MMR) vaccine. This safe and highly effective vaccine provides robust immunity against all three diseases. Two doses of the MMR vaccine are recommended: the first at around one year of age, and the second before starting school, typically between three and five years old. A full two-dose course provides approximately 99% protection against measles.
Despite its proven efficacy and safety, MMR vaccine uptake has seen a worrying decline across the UK, a trend exacerbated by a debunked study from the late 1990s falsely linking the vaccine to autism. Although the study was retracted and its author discredited, the damage to public trust has lingered, contributing to vaccine hesitancy among some parents.
Recent UKHSA figures paint a stark picture. In Enfield, only 64.3% of five-year-olds had received both doses of the MMR vaccine by 2024/25, a rate significantly below the national average and far from the recommended threshold. Across the UK as a whole, 84.4% of children had received two MMR doses by their fifth birthday in 2023-24. This figure represents a decline from a high of 88.8% reached in 2014-15 and remains well below the 95% uptake rate recommended by the World Health Organization (WHO). Achieving this 95% target is crucial for establishing "herd immunity," a phenomenon where a sufficient proportion of the population is immune, thereby protecting those who cannot be vaccinated, such as infants, pregnant women, and individuals with compromised immune systems. When vaccination rates fall below this critical threshold, measles can find fertile ground, leading to outbreaks.
Losing Elimination Status: A National Concern
The declining vaccination rates have had significant national consequences. In January, the World Health Organization (WHO) announced that the UK had officially lost its measles elimination status, following outbreaks identified in the preceding year and early 2024. Measles elimination status is granted to countries that demonstrate no endemic transmission of the virus for at least 12 consecutive months, indicating that any cases are imported and do not spread widely within the population. Losing this status is a severe blow to public health, signifying that measles is once again circulating within the UK population, rather than merely being imported. This development places the UK among a growing number of countries grappling with a resurgence of measles, reflecting a global trend linked to vaccine hesitancy and disruptions to vaccination programmes.
Dr Vanessa Saliba from the UKHSA articulated the gravity of the situation, describing the current outbreak as "big" and "mostly affecting unvaccinated children under 10 in schools and nurseries." She underscored the tragic potential of the disease, stating, "Measles is a nasty illness for any child, but for some it can lead to long term complications and tragically death, but is so easily preventable with two doses of the MMR vaccine."
Public Health Response and Expert Appeals
In response to the escalating situation, Enfield Council is working closely with the UKHSA, the NHS, and local partners to implement national public health guidance and limit further spread. This collaborative effort typically involves enhanced surveillance, contact tracing, and targeted vaccination campaigns to reach unvaccinated individuals in affected areas.
Healthcare professionals and public health officials are issuing urgent appeals to families. Councillor Alev Cazimoglu reiterated, "Vaccination is the most effective way to protect yourself and your family. We urge everyone who is not fully vaccinated to act now." Dr Saliba echoed this sentiment, urging parents whose children had missed doses to "catch up as soon as possible" to protect not only their own children but also vulnerable members of the community who are too young to be vaccinated or medically unable to receive the vaccine.
Furthermore, with the Easter holidays approaching, Dr Saliba issued a critical warning to those planning international travel. She highlighted that "measles is widespread in some countries with close links to the UK, and there are ongoing outbreaks in parts of Europe." This warning serves as a reminder that global interconnectedness means that diseases can easily cross borders, making robust domestic vaccination coverage even more essential.
Understanding Measles: Symptoms and Progression
Recognizing the symptoms of measles early is crucial for timely diagnosis and preventing further spread. After exposure to the virus, there is an incubation period of typically 10 to 12 days before symptoms appear. The initial phase, known as the prodromal stage, is characterized by:
- High fever (often reaching 40°C or 104°F)
- A persistent cough
- Runny nose (coryza)
- Red, watery eyes (conjunctivitis)
A distinctive early sign, often appearing one to two days before the rash, are small white spots inside the mouth, particularly on the buccal mucosa opposite the molars. These are known as Koplik’s spots and are pathognomonic for measles.
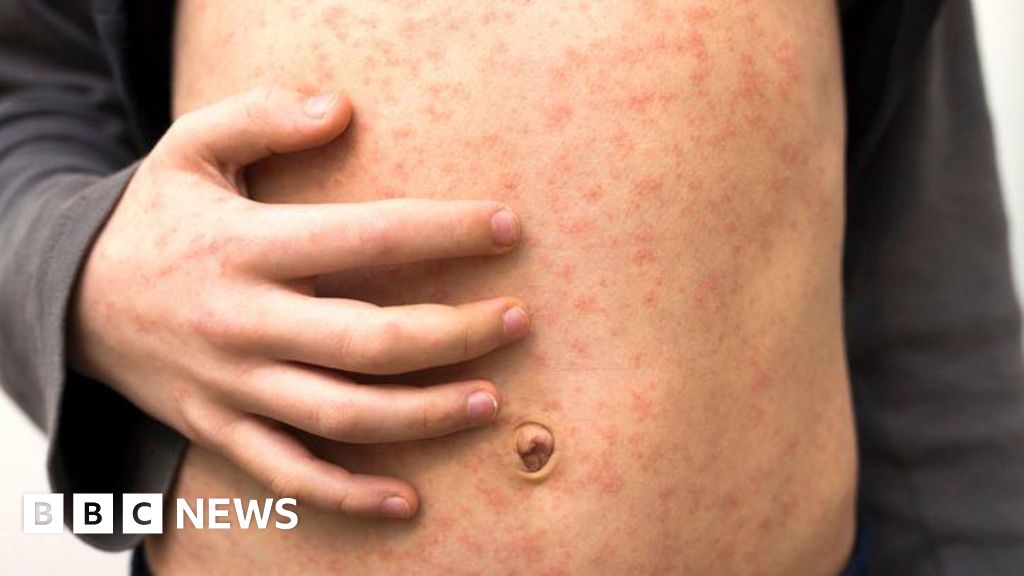
A few days after the initial symptoms, the characteristic blotchy red or brown rash emerges. It typically begins behind the ears and on the face, then spreads downwards to the neck, torso, arms, and legs. The rash can be itchy and coalesce into larger patches. On brown and black skin, the rash may be harder to detect as redness is less apparent, often appearing as darker, discoloured patches. The rash usually lasts for about 5-6 days before fading, leaving a brownish discolouration and sometimes fine peeling of the skin. An individual with measles is contagious from four days before the rash appears until four days after its onset.
The Path Forward: Rebuilding Immunity and Trust
The current measles outbreak in North London serves as a stark warning of the consequences of declining vaccination rates. The path forward requires a multi-pronged approach focused on restoring high levels of immunity and rebuilding public trust in vaccination. This includes sustained public health campaigns to educate parents about the safety and efficacy of the MMR vaccine, accessible vaccination services provided through GP practices and community clinics, and proactive outreach to identify and vaccinate unvaccinated or under-vaccinated children and adults.
Ultimately, the prevention of measles outbreaks is a collective responsibility. By ensuring children receive their recommended two doses of the MMR vaccine, communities can re-establish herd immunity, protect their most vulnerable members, and prevent this highly preventable disease from causing further illness, hospitalisation, and tragic complications.