"Unvaccinated children in North London face 21-day school exclusions as a severe measles outbreak prompts urgent calls for vaccination amidst alarmingly low uptake rates and the UK’s recent loss of its measles elimination status."
This escalating public health crisis underscores a critical vulnerability in community immunity, with local health authorities expressing significant concern over case numbers not seen in decades. The move to exclude unvaccinated pupils is a stark measure reflecting the highly contagious nature of measles and the imperative to protect vulnerable populations, highlighting a broader national challenge in vaccine coverage.
In a decisive move to curb a rapidly spreading measles outbreak, parents in North London, particularly within the borough of Enfield, have been informed that their children could face exclusion from school if not fully vaccinated against the highly contagious disease. This directive comes as local health officials grapple with a "significantly increased number" of cases, a level of infection not witnessed in the region for an extended period, signaling a serious public health challenge.
Enfield Council issued a letter to all parents in late January, stipulating that unvaccinated pupils identified as close contacts of confirmed measles cases could be excluded from educational settings for a period of 21 days. This measure aligns with national guidelines designed to control the spread of infectious diseases and protect the wider school community, especially those too young to be vaccinated or with compromised immune systems. A local health chief conveyed the gravity of the situation to the BBC, stating, "We are worried because actually, this is a significantly increased number than what we’re used to."
While the practice of asking unvaccinated close contacts to stay home during local outbreaks is a standard public health protocol, the sheer scale and intensity of the current situation in North London are causing particular alarm. A local GP surgery has reported confirmed infections in at least seven schools across Enfield and its neighbouring borough, Haringey. Although localised outbreaks have been occurring with increasing frequency across the UK since late 2023, the current cluster represents a worrying escalation. Dr. Jo Sauvage, the chief medical officer of North Central London Integrated Care Board, articulated the concern on BBC Radio 4’s Today programme, noting that while outbreaks do "happen in pockets across the country," her area had "not seen an increase in number of this degree before." She disclosed that approximately 60 suspected cases had been confirmed, predominantly affecting children in schools and nurseries, with some requiring hospital treatment—a disproportionate number of whom were unimmunised. The local health system, she explained, is actively "working closely to contain the infection, the spread, but also increase public knowledge and awareness."
The resurgence of measles in the UK has broader national implications. The country recently lost its World Health Organization (WHO) measles elimination status, a significant setback for public health. This status signifies the absence of endemic measles transmission for at least three consecutive years within a country, a benchmark the UK had proudly maintained. The reversal is largely attributable to a worrying increase in case numbers: over 2,900 measles cases were confirmed in England in 2024, marking the highest level in more than a decade. This was preceded by nearly 1,000 cases in 2023, indicating a concerning upward trend.
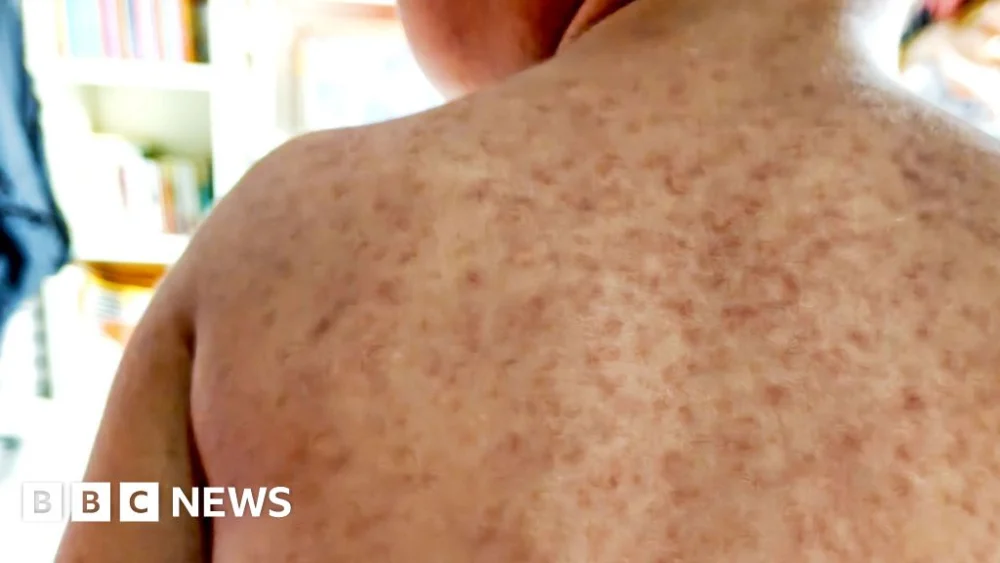
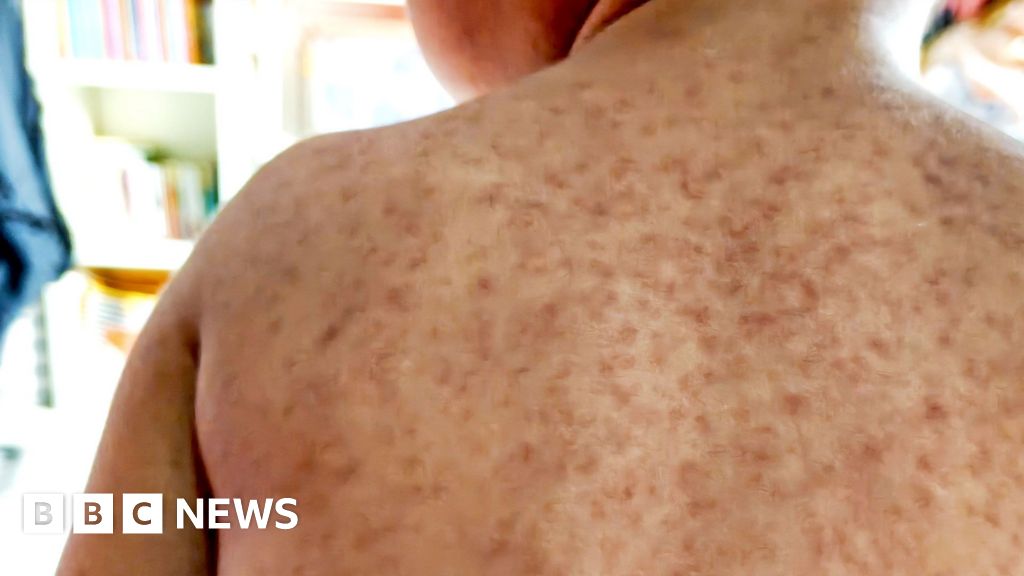
Measles is not merely a benign childhood rash; it is a highly contagious and potentially severe viral infection. Transmitted through respiratory droplets when an infected person coughs, sneezes, or breathes, it can also spread by touching surfaces contaminated with these droplets. Its reproductive number (R0) is estimated to be between 12 and 18, meaning one infected person can typically infect 12 to 18 others in an unvaccinated population, making it one of the most contagious diseases known. Symptoms typically begin with a high fever, followed by a cough, runny nose, and red, watery eyes. A distinctive feature is the appearance of small white spots, known as Koplik’s spots, inside the mouth. A few days later, a characteristic blotchy red or brown rash erupts, usually starting behind the ears and on the face before spreading across the body. It is important to note that this rash can be harder to detect on brown and black skin, potentially delaying diagnosis and treatment.
While most people recover from measles, it can lead to serious and sometimes life-threatening complications. These include pneumonia, ear infections, and, more rarely, encephalitis (inflammation of the brain), which can result in permanent brain damage. A particularly devastating, though rare, long-term complication is subacute sclerosing panencephalitis (SSPE), a fatal neurological disease that can develop years after a measles infection. The vulnerability of unimmunised children is particularly acute, as evidenced by the hospitalisations reported by Dr. Sauvage.
The primary defense against measles is the Measles, Mumps, and Rubella (MMR) vaccine. This highly effective and safe vaccine typically requires two doses for full protection. The first dose is usually given around 12-13 months of age, with the second dose administered before school entry, around three years and four months. To achieve herd immunity—where a sufficient proportion of the population is immune to prevent the spread of the disease and protect those who cannot be vaccinated (e.g., infants, immunocompromised individuals)—a vaccination coverage rate of 95% for both doses is required. Alarmingly, current rates fall significantly short of this critical threshold. In Enfield, only 64.3% of five-year-olds received both doses of the MMR vaccine in 2024/25, one of the lowest rates in the country. Nationally, the uptake stood at 84.4% in the same period, a decline from a high of 88.8% a decade ago. These figures illustrate a dangerous erosion of community protection.
Dr. Ellie Cannon, a local GP in North London, highlighted the severity of the situation, stating that this outbreak was likely the first time she had encountered measles at her surgery in her 20-year career. "We’ve definitely got an issue with children being vaccinated and it certainly needs to improve as we’ve seen with this outbreak," she told BBC Breakfast. The letter to parents from Enfield Council therefore urgently advised families to verify their child’s vaccination status, and indeed their own, to mitigate further spread.
Several complex factors contribute to the declining vaccine uptake. Both Dr. Sauvage and Dr. Cannon pointed to a confluence of issues, including practical difficulties in arranging appointments, a general lack of awareness regarding the importance and schedule of the vaccination programme, and lingering concerns about the vaccine itself. The challenges in accessing primary care services, exacerbated by the pressures on GP practices and the disruptions caused by the recent pandemic, have made it harder for some parents to ensure their children receive routine immunisations. Furthermore, a generation of parents has grown up in an era where diseases like measles were largely eliminated, leading to a diminished perception of the disease’s severity and the vaccine’s necessity.
Regarding vaccine concerns, Dr. Cannon made a crucial distinction between "vaccine refusers" and "vaccine hesitant" individuals. While a small segment of the population actively opposes vaccination based on misinformation or conspiracy theories, a larger group comprises those who are simply hesitant—they may have questions, seek more information, or harbour minor doubts that, if unaddressed, can lead to delayed or missed vaccinations. This hesitancy can often be amplified by historical, now discredited, claims linking the MMR vaccine to autism. Health experts universally affirm the safety and efficacy of the MMR vaccine, emphasizing that rigorous scientific studies have unequivocally debunked any such links. Dr. Sauvage underscored the most effective approach: engaging directly with families, listening to their concerns, and "dispel[ling] any concerns they have about side effects or problems with the vaccine, which is safe."
The public health response to this North London outbreak is multifaceted. Beyond the school exclusion policy, local health authorities are intensifying surveillance, conducting robust contact tracing, and launching awareness campaigns. These efforts aim not only to contain the immediate spread but also to rebuild public confidence in vaccination and improve uptake rates. The long-term implications of sustained low vaccination rates are profound, placing increased strain on healthcare services, disrupting education, and potentially leading to more widespread and severe outbreaks in the future.
Ultimately, the responsibility rests with individuals and communities to ensure collective protection. Parents are strongly urged to consult their GP or local health services to check their and their children’s vaccination records. The MMR vaccine remains the most effective tool to prevent measles, protecting not only the vaccinated individual but also contributing to the vital herd immunity that safeguards the most vulnerable members of society. Reversing the current trend of declining vaccination rates is paramount to preventing measles from becoming an endemic threat once more and to reinstating the UK’s hard-won status in global disease elimination.