"Amidst a record 8,000 Britons awaiting life-saving organ transplants, the critical role of family conversations in upholding donor wishes emerges as the key to unlocking new futures."
This quote encapsulates the paradoxical challenge currently facing the United Kingdom’s organ donation system. Despite the implementation of an "opt-out" law designed to boost donor numbers, a growing number of families are overriding their loved ones’ recorded decisions to donate. This critical disconnect leaves thousands in a precarious limbo, where the deeply personal choice to donate transforms into a vital family discussion, underscoring the profound impact of communication on the gift of life.
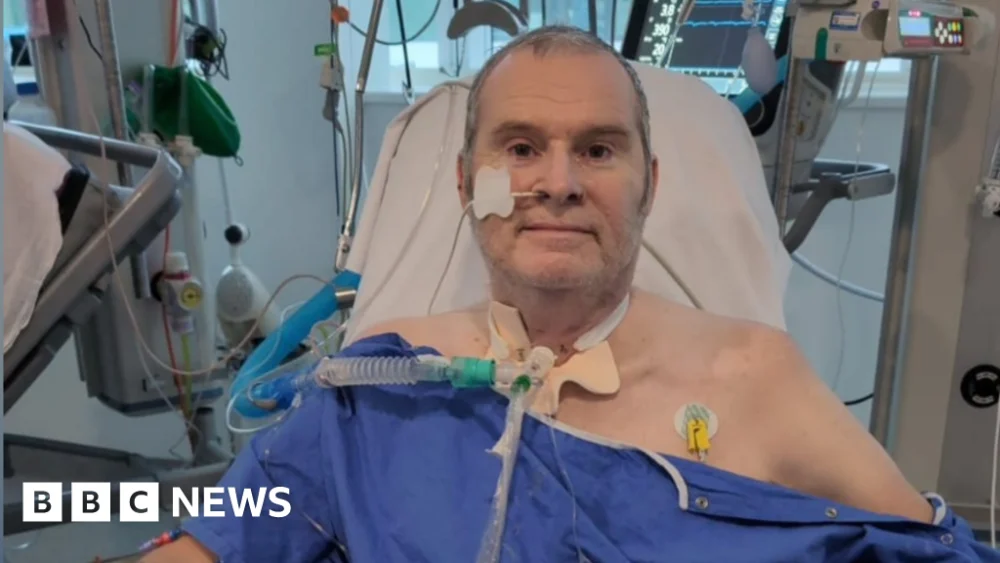
For Matthew Smith, a resident of Wednesbury in the West Midlands, each day for nearly a year was a torturous waiting game. Diagnosed in 2023 with a terminal lung condition that progressively robbed him of his breath and vitality, his only hope for survival lay in an urgent double lung transplant. The phone, a ubiquitous modern device, became a harbinger of destiny, its potential ring carrying the weight of his future. "From when you first wake up, you think, is today going to be the day we get that call?" he recounted, a sentiment echoed by his wife, Nicola. Her nights were punctuated by anxious checks of her phone, a vigilant guard against the possibility of missing the life-altering summons. The terminal nature of Matthew’s condition meant that without a transplant, his life expectancy was severely limited, with his days increasingly tethered to oxygen tanks, diminishing his quality of life and ability to engage in everyday activities.
After 10 agonizing months, the call finally came, offering Matthew a reprieve and a new lease on life. However, his journey underscores a growing national crisis. Currently, more than 8,000 individuals across the UK are on the waiting list for an organ donation – a number that represents an all-time high. In the West Midlands alone, approximately 500 people are in desperate need of a vital operation. While the demand for organs has soared, the donor consent rate has regrettably stagnated. A significant factor contributing to this stagnation is the increasing tendency of families to refuse to allow their loved ones’ organs to be donated after death, even when the deceased had expressed a clear wish to do so. This familial veto directly translates into longer waits and, tragically, preventable deaths for patients like Matthew.
In an effort to address the persistent shortage of organs, England introduced an "opt-out" donation system, often referred to as Max and Keira’s Law, in May 2020. This followed Wales, which had implemented a similar system five years earlier in December 2015. The core principle of this legislation is "presumed consent": all adults are considered to have agreed to donate their organs unless they have explicitly recorded a decision to opt out. When first proposed in 2018, then-Prime Minister Theresa May’s government estimated that this change could save up to 700 lives annually, a testament to the system’s potential to bridge the gap between supply and demand. The law was celebrated as a progressive step, aligning the UK with other European nations that had successfully adopted similar models.
However, the "fatal flaw" in this otherwise promising system lies in the continuing power of family members to veto a deceased loved one’s wishes. Even if an individual has signed up to the organ donor register or is presumed to have consented under the opt-out law, their next of kin can override that decision. This provision, while intended to respect the emotional distress of grieving families, inadvertently undermines the very foundation of the opt-out system and the autonomy of the donor. The reasons families provide for blocking donations are varied and deeply personal. They often include not being aware of what the patient would have wanted, feeling that the donation process takes too long during a time of immense grief, reluctance to allow further surgery to the body of their loved one, or objections based on religious or cultural beliefs. These factors highlight the complex emotional and ethical landscape surrounding end-of-life decisions and organ donation.
Christine Cox MBE, a dedicated campaigner from Wolverhampton, has been at the forefront of the organ donation movement for over 35 years. Her advocacy began in 1989 after the tragic death of her brother, Peter, from a brain tumour at the young age of 24. Despite his own terminal condition, Peter’s final wish was for his life to benefit others. His selfless decision ultimately led to 17 people receiving the gift of life through his organ donations. "He did say it was our duty to ensure that as many organs as possible could benefit others," Christine recalled, emphasizing the profound impact of his legacy. However, in the immediate aftermath of Peter’s death, Christine and her parents discovered a critical void: there was no official national list for individuals willing to donate. This significant systemic gap spurred them into relentless action, campaigning tirelessly until the introduction of the first organ donor register in 1994. Prior to this, organ donation relied precariously on individuals carrying physical donor cards, which were often not readily available or easily accessible during emergency situations. "People didn’t always carry the donor card on them in their pockets and handbags and the nurses and doctors didn’t have time to look through. So there was a problem," Cox explained, highlighting the logistical hurdles that limited potential donations.

Over the decades, Christine Cox’s unwavering commitment has earned her numerous accolades and awards. While she welcomed the introduction of the opt-out system as a significant victory, she quickly recognized the "fatal flaw" inherent in allowing next of kin to rescind a loved one’s recorded wishes. For Cox, the solution lies not in further legislative changes to the veto power, but in proactive and open discussion. "I implore everybody not just to make their wishes known but to talk to their friends and their family and also find out what their friends and family want," she urged. "It possibly will never happen however everyone needs to know what your wishes are." This emphasis on dialogue transforms organ donation from a solitary choice into a shared understanding, potentially alleviating the burden on grieving families to make a decision in a moment of profound distress.
This strategic approach is strongly echoed by the NHS, which recently launched its "Hope Takes Flight" campaign, specifically urging families to engage in conversations about organ donation before it becomes a time-sensitive, high-stakes decision. Harpreet Matharu, an organ donation specialist nurse for the NHS, articulated the critical impact of these discussions: "What we’ve always said is talk to your loved one, make a decision and sign on the register, because we know when a patient has opted in and had those conversations, consent is much higher in those circumstances." Her insight highlights the direct correlation between pre-emptive family discussions and successful donations.

For those who harbor apprehension or "squeamishness" about the process, Matharu emphasized the importance of understanding the facts. She assured potential donors and their families that the donation process is conducted with the "utmost respect" in hospitals, with all religious and cultural needs meticulously catered for. Furthermore, she noted that the act of donation can often provide a measure of solace and contribute positively to the grieving process for families, offering comfort in knowing their loved one’s final act has given life to others. The compassionate and professional care provided ensures that the dignity of the donor is maintained throughout.
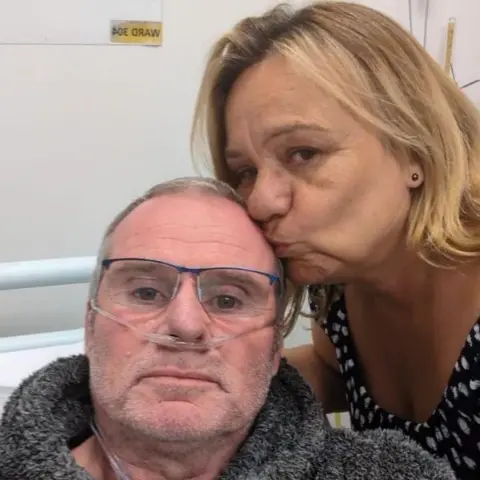
For Nicola Smith, the day her husband Matthew underwent his double lung transplant was fraught with intense emotion. "I think I cried from when he went in until he came out. It’s the start of a new beginning. It’s a new life," she shared, reflecting on the profound transformation. Matthew’s recovery has opened up a world of possibilities previously denied by his illness. "He can do so much more now, he can take part in things. It just feels like his life’s just beginning again now." This renewed vitality has allowed them to dream of future milestones, including renewing their vows on their 30th wedding anniversary this year on the picturesque beaches of Cornwall.

Nicola’s experience has solidified her belief in the life-altering power of organ donation. She implored everyone to seriously consider becoming an organ donor and to understand the lasting, positive impact such a decision can have. "You’re giving somebody the chance of a new future, to live a good, long life. To make memories," she stated passionately. In a nation where thousands await a miracle, these conversations are not merely advisory; they are potentially life-saving, transforming personal choices into collective acts of profound generosity that redefine futures and create enduring legacies.