"This groundbreaking internal lengthening technique, successfully performed on a child for the first time in the UK, heralds a new era for paediatric orthopaedics, promising less painful and more effective treatment for children facing significant limb discrepancies, fundamentally transforming their quality of life and future mobility."
In a landmark achievement for paediatric medicine, a nine-year-old boy named Alfie Phillips has become the first child in the United Kingdom to undergo a revolutionary surgical procedure designed to lengthen his limb internally. This innovative treatment, carried out by experts at Liverpool’s renowned Alder Hey Children’s Hospital, addresses a challenging condition known as fibular hemimelia, which left Alfie with a significant disparity in the length of his legs. The success of this pioneering operation not only marks a pivotal moment in Alfie’s personal journey towards greater mobility and confidence but also sets a new standard for limb reconstruction in younger patients across the nation.
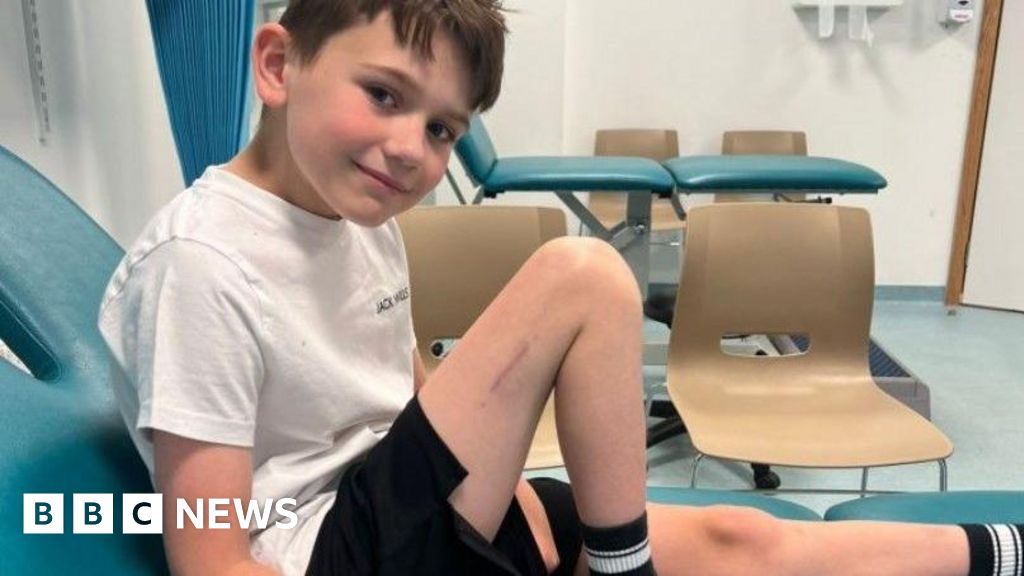
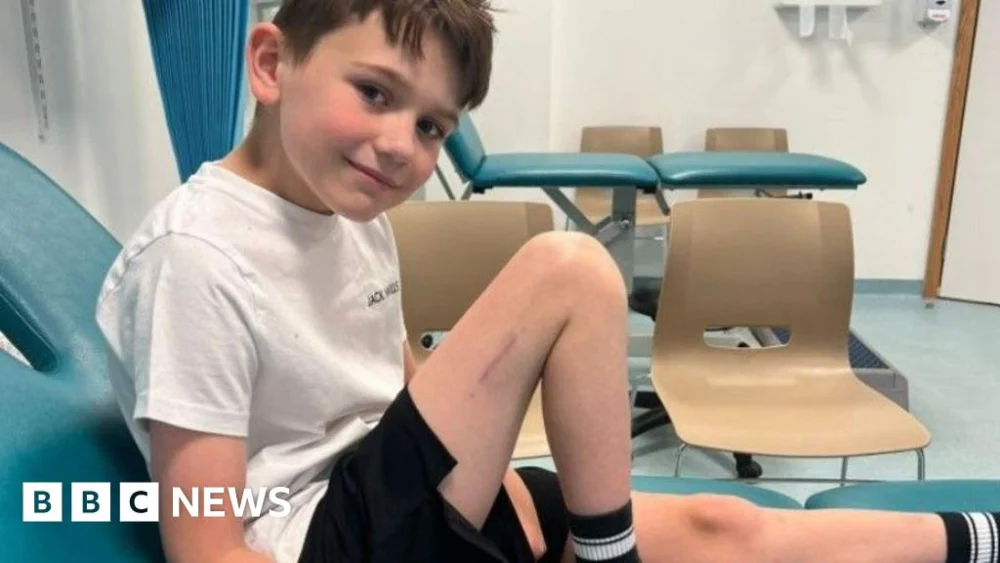
Alfie, hailing from Northampton, was diagnosed with fibular hemimelia, a rare congenital condition affecting fewer than one in 40,000 births. This developmental anomaly meant his right leg had not grown to its full potential, resulting in it being noticeably shorter than his left. Such a discrepancy can lead to a host of physical challenges, including gait abnormalities, chronic pain, spinal issues, and significant psychological distress as children navigate their formative years with a visible and functional difference. Historically, treatment options for paediatric limb length discrepancy have been invasive, prolonged, and often fraught with complications, particularly for very young children whose delicate growth plates pose unique surgical challenges.
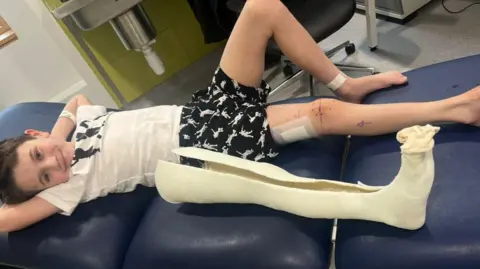
The conventional method for addressing significant limb length discrepancies in children involved external fixators – a cage-like apparatus fitted externally to the limb, with pins drilled through the skin and bone. While effective in gradually lengthening bone, these devices are notoriously uncomfortable, prone to infection, limit mobility, and carry a heavy psychological burden for children and their families, often requiring months, or even years, of wear. For Alfie, before his referral to Alder Hey in 2024, an external fixator was considered his primary option, underscoring the limited alternatives available at the time.
However, medical science continues to advance, and the team at Alder Hey Children’s Hospital has been at the forefront of adopting cutting-edge techniques. The procedure Alfie underwent utilized a state-of-the-art method involving the implantation of a motorised telescopic nail. Unlike traditional intramedullary nails, which are placed within the bone marrow cavity and can interfere with a child’s growth plates, this pioneering device was meticulously positioned on the surface of Alfie’s right femur, or thigh bone. This external-internal placement circumvents the risk of damaging the crucial epiphyseal growth plates, which are responsible for bone lengthening during childhood, thereby making internal lengthening a viable and safer option for younger patients for the first time.
Consultant Orthopaedic Surgeon Nick Peterson, a leading expert at Alder Hey, highlighted the profound impact of this innovation. "We know that being able to lengthen internally is less painful and a better experience overall," Mr. Peterson explained. "But before this technique, it wasn’t available for children." His words underscore the significance of this breakthrough, which promises to revolutionize the standard of care for paediatric limb reconstruction. The ability to perform lengthening internally translates into fewer complications, reduced pain, shorter hospital stays, and a vastly improved quality of life throughout the treatment period.
Alfie’s operation to install the innovative lengthening nail took place in March 2025. Following the surgical placement, which saw him spend less than a week recovering in hospital, the real work of lengthening began. The process involved a remarkable feat of biomedical engineering: a magnetic device was placed on Alfie’s leg three times a day for a month. This external magnetic field activated the internal telescopic nail, causing it to slowly extend by approximately 1mm each day. This controlled and gradual distraction stimulated the body’s natural regenerative capabilities, a process known as distraction osteogenesis, where new bone tissue naturally fills the created gap.
The careful calibration of this daily lengthening, coupled with rigorous weekly physiotherapy sessions, was crucial to the success of the treatment. These sessions, overseen by doctors and specialist nurses, ensured that Alfie’s muscles, tendons, and nerves adapted to the gradual increase in bone length, preventing stiffness and promoting optimal function. The active lengthening phase lasted around six weeks, during which Alfie gained an impressive 3cm (1.2in) in his right leg, significantly reducing the initial discrepancy that experts at Alder Hey had measured at 4cm (1.6in) and projected to increase to 6cm (2.4in) by adulthood. Alfie continued with physiotherapy until the nail was safely removed from his leg, approximately three to four months after the initial operation, allowing the newly formed bone to fully consolidate and strengthen.

Alfie’s mother, Laura Ducker, 34, spoke with immense pride about her son’s resilience and recovery. "He healed really well," she recounted. "He coped magnificently. He was keen to go back to school fairly quickly." Her account paints a vivid picture of a courageous young boy who embraced the challenges of his unique journey. "He’s running around as normal, if you were to look him you would never know that there had ever been anything happen. He is just incredible," she added, emphasizing the transformative outcome of the surgery. Indeed, almost a year on from his groundbreaking procedure, Alfie is thriving, enjoying a newfound freedom in his movements and actively participating in activities like basketball, which were previously hindered by his condition.
The implications of Alfie’s successful surgery extend far beyond his individual case. Mr. Peterson described Alfie’s recovery as "remarkable" and highlighted the broader impact: "Alfie’s case paves the way for this technique to replace that old fashioned way of doing things." Since Alfie’s pioneering procedure, Alder Hey Children’s Hospital has successfully performed the same technique on three other children with fibular hemimelia, further solidifying its efficacy and safety profile in a paediatric context. Moreover, other specialist centres across the UK are now actively preparing to adopt this innovative approach, signalling a nationwide shift in how limb length discrepancies will be managed in children.
This advancement not only improves the immediate experience for young patients by reducing pain and discomfort associated with external fixators but also promises significant long-term benefits. Children undergoing internal lengthening are likely to experience fewer complications, faster rehabilitation, and better psychological outcomes, fostering greater self-esteem and participation in age-appropriate activities. While Alfie may require further lengthening treatment on his shin bone in the future as he continues to grow, the foundation laid by this initial surgery has ensured that his overall experience will be "vastly superior to what it would have been," according to Mr. Peterson.
The development of this technique, originating in the US, represents a culmination of years of research and development in the field of orthopaedic biomechanics. It underscores the global collaborative effort within the medical community to push the boundaries of what is possible, particularly for vulnerable paediatric populations. Alder Hey Children’s Hospital, with its reputation as a leading centre for paediatric care and innovation, has demonstrated its commitment to bringing these world-class treatments to UK children, ensuring they have access to the best possible care.
Alfie Phillips’s journey is more than just a medical success story; it is a beacon of hope for countless children and families affected by limb length discrepancies. His courage as the first patient to undergo this groundbreaking surgery in the UK has not only transformed his own life but has also illuminated a new path for paediatric orthopaedic care, promising a future where children can grow, play, and thrive with greater ease and confidence. The widespread adoption of this internal lengthening technique is poised to fundamentally reshape the landscape of limb reconstruction, offering a less arduous and more effective route to full mobility and an enhanced quality of life for the next generation.