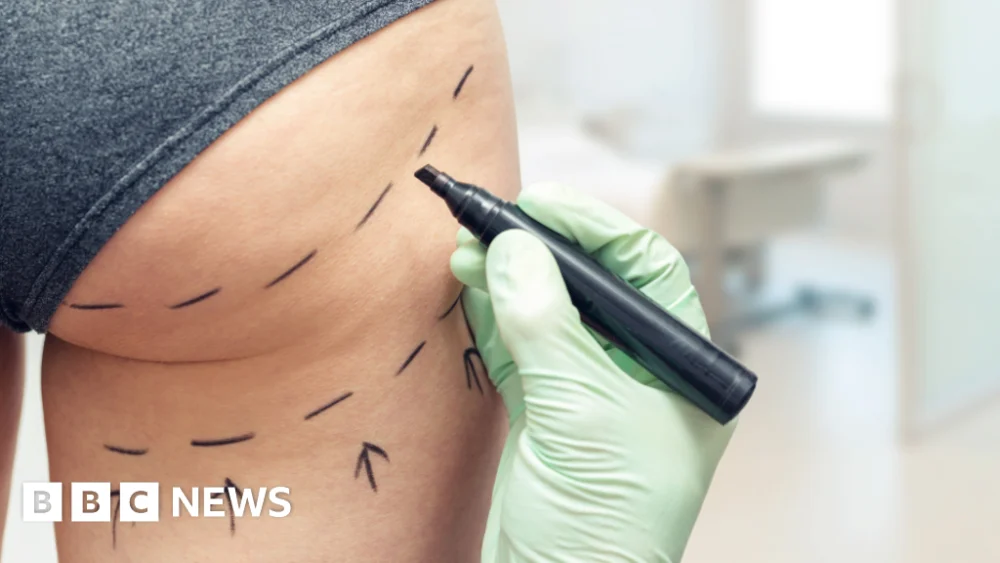
"Immediate, stringent regulations are imperative to halt the perilous ‘wild west’ of high-risk cosmetic procedures, with a cross-party parliamentary committee advocating for an exclusive doctor-led provision to safeguard public health and prevent further tragedies."
A stark warning has been issued by a cross-party parliamentary committee, demanding an immediate overhaul of regulations governing high-risk cosmetic procedures such as liquid Brazilian butt lifts (BBLs) and liquid breast augmentations. The Women and Equalities Committee has called for these treatments to be performed exclusively by qualified medical doctors, a measure that would effectively ban their widespread availability due to the inherent dangers. This urgent plea comes amidst a backdrop of a largely unregulated market, described by MPs as a "wild west," where life-threatening procedures are reportedly being carried out in unsafe and unsanitary environments, ranging from private homes to public toilets.
The committee’s report underscores a critical public health crisis, highlighting the severe complications that can arise from these non-surgical treatments when administered by untrained or unqualified individuals. Unlike traditional surgical BBLs, which involve fat transfer, liquid BBLs typically utilize injectable fillers – sometimes illicit, industrial-grade substances – that carry a high risk of embolism, infection, disfigurement, and even death. The current regulatory vacuum means that virtually anyone can offer these procedures without formal medical training, licensing, or oversight, creating a perilous landscape for consumers seeking cosmetic enhancements.
The government has acknowledged the need for reform and has proposed similar measures, including restricting high-risk procedures to regulated healthcare professionals. However, a definitive timeline for the implementation of these vital safeguards remains elusive. This delay has drawn sharp criticism from the committee, which argues that further consultation is unnecessary and that immediate action is paramount to prevent more individuals from suffering devastating consequences. The lack of regulation for non-incisional cosmetic treatments has fostered a booming, yet dangerous, industry where profit often supersedes patient safety.
The tragic case of Sasha Dean from Bedfordshire serves as a harrowing testament to the life-threatening risks associated with these unregulated procedures. In early 2024, Dean underwent a liquid BBL in a private residence, an experience that rapidly spiraled into a catastrophic health crisis. She developed sepsis, a severe infection that led to a heart attack, a collapsed lung, and failing kidneys, ultimately leaving her in an induced coma for five days. While Dean miraculously recovered, the ordeal has left her with profound and lasting physical and cognitive side effects, including hair loss, memory issues, and impaired vision. Her story is a stark reminder of the potential for irreversible damage and the urgent need for protective legislation. "It’s ruined my life, quite frankly," Dean shared, now a fervent advocate for banning the procedure entirely, emphasizing that despite being non-surgical, it remains incredibly dangerous.
Sarah Owen, the Labour MP and chair of the Women and Equalities Committee, voiced profound concern over the government’s perceived inaction. "The government is not moving quickly enough. There is no need for further consultation and delay," Owen stated, condemning the "wild west" market for placing the public at unacceptable risk. The committee’s recommendations extend beyond just high-risk procedures, also urging the government to commit to introducing a comprehensive licensing scheme for lower-risk non-surgical treatments, such as Botox and lip fillers, by the end of the current parliamentary term in 2029. Under the government’s proposed plans, high-risk procedures would be subject to inspection by the Care Quality Commission (CQC), while lower-risk treatments would fall under local council licensing schemes.
A spokesperson for the Department of Health and Social Care (DHSC) affirmed the government’s commitment to "crack down on ‘cosmetic cowboys’ and root out dangerous treatments." They stated that "tough new measures will ensure only qualified healthcare professionals will be able to perform the highest-risk procedures," and advised consumers to verify providers’ qualifications and insurance, and to be wary of suspiciously cheap treatments. However, the absence of a confirmed date for the introduction of these critical measures remains a significant point of contention for the committee and patient safety advocates. Calls for stricter regulations have been ongoing for over a decade, with formal consultations commencing only in 2023, a pace deemed insufficient given the escalating risks.
The delay in regulatory action has coincided with a rapid proliferation of businesses offering these cosmetic procedures. A recent study by University College London highlighted the alarming scale of the issue, revealing over 5,500 clinics providing non-surgical cosmetic treatments across the UK, with a mere third of practitioners being qualified doctors. This unregulated growth has led to a disturbing lack of consistency in training standards, with some individuals reportedly relying solely on online courses before administering treatments that carry significant medical risks. The ease of entry into this lucrative market for untrained individuals, combined with aggressive marketing tactics, further exacerbates the danger to unsuspecting consumers.
Dr. Sophie Shotter of the British College of Aesthetic Medicine echoed the committee’s call for immediate action, emphasizing that there is no justifiable reason for further delay. "If the government clearly defines which procedures are considered high-risk and legislates that only regulated healthcare professionals can perform them, implementation could happen relatively quickly," she explained. Dr. Shotter stressed that clarity in defining "high-risk" is paramount for effective enforcement, asserting that once a clear legal boundary is established, it should become a prosecutable offense for non-clinicians to carry out such treatments. The medical aesthetic community is united in its demand for a robust regulatory framework that prioritizes patient safety above all else.
Beyond the immediate domestic concerns, the MPs’ committee also raised critical points regarding the broader ecosystem influencing cosmetic procedures. They called upon the NHS to begin systematically recording data on complications arising from cosmetic surgery performed abroad. This initiative is crucial for understanding the full scope of medical tourism’s impact, particularly given reports of individuals requiring emergency care in the UK following botched treatments in other countries. The committee also expressed significant apprehension regarding the pervasive influence of social media platforms and online influencers. These digital trends, they argue, contribute to worsening body image issues and fuel an increasing demand for cosmetic procedures, especially among vulnerable young women and girls, often without adequately informing them of the associated risks.
In response to the committee’s comprehensive report, the government stated it would consider the recommendations. However, for the countless individuals like Sasha Dean, and for the medical professionals and parliamentary groups advocating for change, "considering" is no longer enough. The consensus is clear: the current regulatory vacuum is a ticking time bomb, and immediate, decisive action is urgently required to transform the dangerous "wild west" of cosmetic procedures into a safe, regulated, and ethical healthcare environment. The lives and well-being of thousands of individuals depend on it.