"This landmark birth represents a profound triumph of medical innovation and human generosity, offering a beacon of hope for countless women dreaming of carrying their own child."
The arrival of baby Hugo marks an extraordinary moment in British medical history, signifying the first successful birth in the UK following a womb transplant from a deceased donor. This groundbreaking achievement not only transforms the lives of Grace Bell and Steve Powell, who longed for a family, but also opens a revolutionary pathway for women nationwide affected by uterine factor infertility, demonstrating the profound potential of organ donation and advanced reproductive medicine.
A "Miracle" Ten Weeks in the Making
Grace Bell, in her thirties, and her partner Steve Powell from Kent, are celebrating the arrival of their son, Hugo Richard Powell, who is now 10 weeks old. Born just before Christmas 2025, weighing a healthy nearly 7lbs, Hugo is, in his mother’s words, "simply a miracle." Grace was born with Mayer-Rokitansky-Küster-Hauser (MRKH) syndrome, a condition affecting approximately one in 5,000 women in the UK, where individuals are born without a viable womb but possess normal ovaries. At the tender age of 16, Grace faced the devastating news that she would never be able to carry her own child. For years, the dream of having a biological child seemed distant, with surrogacy or a pioneering womb transplant being their only avenues.

The journey to Hugo’s birth was long, arduous, and emotionally charged. When Grace received the life-altering phone call confirming a suitable womb had become available from a deceased donor, she recalls being "in complete shock" and "really excited." Yet, intertwined with her personal joy was an acute awareness of the immense "kindness and selflessness" of the donor and her family, whose "incredible gift" made her dream a reality. Grace expresses profound gratitude, stating, "I think of my donor and her family every day and pray they find some peace in knowing their daughter gave me the biggest gift: the gift of life. A part of her will live on forever." The profound impact of this altruistic act is further underscored by the fact that the donor also saved four other lives through the donation of five additional organs.
The Intricate Dance of Medical Innovation
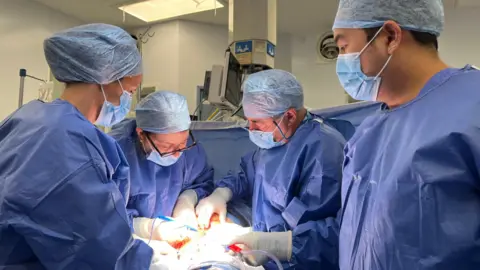
The successful transplant operation, a complex 10-hour procedure, took place at The Churchill Hospital in Oxford in June 2024. This surgical feat involved an elite multidisciplinary team of gynaecologists, transplant surgeons, anaesthetists, and specialist nurses, meticulously connecting delicate blood vessels and tissues to ensure the transplanted womb was viable. The procedure itself is one of the most challenging in transplant medicine, requiring exceptional precision to re-establish blood flow and nerve connections to the donor organ. Following a period of recovery and monitoring to ensure the body accepted the new organ and Grace’s immune system was adequately suppressed, Grace and Steve embarked on the next crucial step: In Vitro Fertilisation (IVF) treatment and subsequent embryo transfer at The Lister Fertility Clinic in London. This carefully orchestrated sequence of medical interventions culminated in a healthy pregnancy and, ultimately, Hugo’s birth via C-section at Queen Charlotte’s and Chelsea Hospital in west London.
Hugo’s delivery was a moment of unparalleled emotion for Grace. "It was simply a miracle," she recounts. "I remember waking up in the morning and seeing his little face, with his little dummy in, and it felt like I needed to wake up from a dream. It was just incredible." The middle name, Richard, was chosen as a tribute to Consultant Gynaecologist Professor Richard Smith, a visionary figure who has dedicated over 25 years to researching womb transplantation and founded the charity Womb Transplant UK. His unwavering commitment, alongside that of the entire medical team, brought this once-impossible dream to fruition.
Pioneering a New Pathway: The UK Clinical Research Trial

Hugo’s birth is not an isolated event but a monumental success within a carefully structured UK clinical research trial. This trial aims to rigorously assess the efficacy and safety of womb transplantation, paving the way for it to become an approved and regular treatment for women facing uterine factor infertility. Currently, 10 transplants from deceased donors are planned under this trial, with three already completed, culminating in Hugo being the first baby born. Additionally, five other womb transplants from close living relatives are also in the pipeline, highlighting the comprehensive approach to understanding both donor types and optimizing outcomes. The ethical framework governing these trials is stringent, ensuring patient safety and careful consideration of all medical and psychological aspects.
Professor Smith, from Imperial College Healthcare NHS Trust, was present at Hugo’s birth, reflecting on the culmination of decades of research and collaborative effort. He emphasised that "a huge team of people" were involved at every stage – from the intricate transplant operation to the delicate embryo transfer and the final delivery. The successful outcome provides tangible evidence that this procedure offers genuine hope to girls and young women who, like Grace, were told they would never carry their own child.
Transplant surgeon and joint team leader Isabel Quiroga expressed her delight, calling Hugo’s birth "a breakthrough for organ transplantation in the UK." She noted that "very few babies have been born in Europe as a result of their mothers receiving a womb from a deceased donor," underscoring the pioneering nature of this achievement. The trial’s overarching goal is to determine if this complex procedure can be scaled and integrated into standard medical practice, offering a lifeline to the increasing number of women of child-bearing age who do not possess a viable womb, whether due to congenital conditions like MRKH, cancer, or hysterectomy.
The Ethical and Altruistic Dimensions of Donation
Unlike other vital organ donations, such as kidneys or hearts, donating a womb for transplant is a unique and deeply personal decision. It is not automatically covered by general organ donation consent; instead, it requires a special, explicit request to potential donors’ families who have already agreed to donate their relative’s organs. This nuanced approach ensures that families are fully informed and comfortable with this specific form of donation, which carries profound emotional and symbolic weight, given its connection to motherhood and the creation of new life. The altruism required from donor families in such circumstances is immense, transforming their grief into a powerful legacy of hope.
The anonymous donor family, whose daughter’s gift made Hugo’s birth possible, shared their feelings of "tremendous pride" in the enduring legacy their daughter has left. They stated, "Through organ donation, she has given other families the precious gift of time, hope, healing and now life." This sentiment beautifully encapsulates the extraordinary ripple effect of organ donation, transforming despair into joy, and loss into new beginnings. The donor’s act of generosity extended beyond the womb, with five other organs successfully transplanted into four different individuals, a testament to her profound impact and the lifesaving potential of organ donation as a whole.
Global Progress and Future Horizons
Globally, the field of womb transplantation has seen remarkable progress since the first successful live-donor womb transplant in Sweden in 2014. More than 100 womb transplant operations have been performed worldwide, resulting in the birth of over 70 healthy babies. Subsequent advancements have broadened the scope to include deceased donors, as seen in the UK’s recent success. While the genetic material of the baby naturally derives from the recipient mother and father, there is no genetic link whatsoever to the womb donor, a point often clarified to reassure prospective parents and the public about the unique nature of this procedure.
Looking ahead, Grace and Steve may choose to have a second baby, utilising any remaining embryos from their IVF treatment. After their family is complete, the transplanted womb will be surgically removed. This is a crucial step to spare Grace from a lifetime of potent immunosuppressant drugs, which are necessary to prevent her body’s immune system from rejecting the transplanted organ but carry significant long-term health risks, including increased susceptibility to infections and certain cancers. This planned removal underscores the temporary, therapeutic nature of the transplant, designed specifically to enable childbearing rather than as a permanent organ replacement.
The success of this UK trial holds immense promise. It not only provides a tangible solution for women with uterine factor infertility but also pushes the boundaries of transplant medicine, fostering further research into organ viability, surgical techniques, and immunological management. While challenges remain, including the scarcity of suitable donors, the complexity and high cost of the procedure, and the extensive psychological support required for recipients throughout their journey, Hugo’s birth marks a pivotal moment. It signifies that hope is no longer a distant dream but a tangible reality for thousands of women who long to experience the profound journey of pregnancy and childbirth. This achievement stands as a testament to scientific ingenuity, the relentless dedication of medical professionals, and the unparalleled generosity of those who choose to give the gift of life.
