"A single moment of misfortune on a train journey unveiled a hidden battle, transforming Lauren Macpherson’s life from a celebratory trajectory to an urgent fight for time and access to vital treatment."

Lauren Macpherson’s story is a stark reminder of how life can pivot without warning, and how incidental findings can reveal profound truths. What began as a routine journey home from a music festival, marred by a common travel mishap, unexpectedly led to the discovery of a terminal brain tumour. This incident not only brought to light a serious medical condition that had been silently progressing but also propelled Lauren into an unforeseen role as an advocate for advanced cancer treatments, highlighting critical disparities within the healthcare system across the UK.
At 29 years old, Lauren Macpherson was on the cusp of a vibrant future. She had just celebrated significant milestones: passing crucial exams for a promotion at work and purchasing her first home with her boyfriend, Zak. The August bank holiday weekend had been spent reveling at a music festival in London, a joyous occasion marking what was meant to be the "first of many" celebrations. Little did she know that the journey home to Cardiff would dramatically alter the course of her life, revealing a silent and deadly adversary lurking within her.
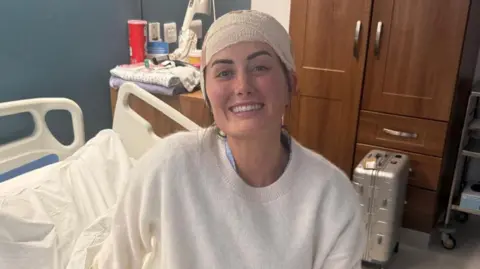
The fateful incident occurred on the train. As Lauren settled in for the ride, a heavy 35lb (16kg) suitcase dislodged from the overhead storage compartment, plummeting onto her head. The immediate concern was for a potential spinal injury, a common fear with such an impact. Consequently, Lauren was taken off the train at Swindon and rushed to hospital for a CT scan. While the scan aimed to rule out fractures to her spine, it uncovered something far more sinister: an unexpected "shadow" on her brain. This incidental finding marked the beginning of a harrowing diagnostic journey that would unravel years of unexplained symptoms and ultimately deliver a terminal prognosis.
Looking back, Lauren realised the "shadow" offered an explanation for a year of puzzling and often debilitating symptoms that had previously been dismissed. She had been struggling with emotional dysregulation, an inability to manage or express emotional responses, coupled with profound, extreme fatigue. Additionally, she experienced gut issues and unsettling blackouts. These symptoms had led her to visit her GP three times, undergoing various tests, but were attributed to hormonal imbalances or an undiagnosed Attention Deficit Hyperactivity Disorder (ADHD). The fatigue, in particular, was so severe that Lauren had to reduce her working hours as a cardiographer from full-time to part-time, just to manage her studies for her master’s degree. The ambiguity of these early signs underscores a pervasive challenge in brain tumour diagnosis, where symptoms can often mimic less severe conditions, delaying critical early intervention.

Upon being told about the shadow on her CT scan, Lauren recounted an immediate, visceral understanding. "There is an instinct inside you and when you have been feeling unwell, it just all made sense," she stated. Initially, a sense of relief washed over her – a feeling that the elusive cause of her prolonged malaise had finally been identified. "It’s almost like a relief, you think you’re going crazy, all these things going wrong. To be honest I was quite naive… I was worried but at this point I wasn’t scared." She harboured a hopeful, albeit misinformed, belief: "I didn’t think at this point, it’s incurable, I just thought ‘they’ve found it, they can get rid of it’." This initial optimism, however, was short-lived. An MRI scan in Cardiff two days later confirmed the presence of a brain tumour, but it was at a follow-up appointment a month later that the true gravity of her condition was laid bare. Doctors suspected glioblastoma, a highly aggressive and fast-growing form of brain cancer, notorious for its poor prognosis, often giving patients only 12-18 months, or in aggressive cases, as little as two years to live. The shock was profound: "We did not expect it at all. Then it kind of hit me and that’s when you’re like, ‘oh my god, you could be looking at two years’." The floor had indeed dropped from beneath her, leaving her grappling with a future unimaginable just weeks prior.
The immediate and critical next step was surgery to remove the tumour. However, Lauren faced a daunting four-month waiting list for this vital procedure within the NHS. For a condition as aggressive and fast-moving as a brain tumour, such a delay was not merely inconvenient but potentially life-threatening. Driven by a primal "survival instinct," Lauren and Zak explored private healthcare options. Leveraging Zak’s health insurance, they were able to dramatically cut the waiting time to just three weeks, highlighting a stark disparity in access to urgent medical care. A spokesperson for Cardiff and Vale University Health Board acknowledged that patients are assessed "in line with their clinical need" and cancer cases prioritised to ensure timely surgery and treatment. They added, "In Lauren’s case this would have been organised soon after she was assessed as fit and completed her pre-operative tests. However, Lauren ultimately made the decision to seek treatment privately." This incident underscores the ongoing pressures on public health systems and the difficult choices patients sometimes face when time is of the essence.

Lauren underwent brain surgery at the end of October, a procedure that successfully removed approximately 80% of the tumour. While this was a significant achievement, the tumour’s location in the speech cortex of her brain presented immediate and severe post-operative challenges. The speech cortex is a critical area responsible for language processing and production. Damage or disruption to this region can lead to aphasia, impairing a person’s ability to communicate. For weeks following the surgery, Lauren was unable to speak and experienced a substantial loss of cognitive function. Her recovery was arduous, marked by days of debilitating sickness and vertigo. "It’s almost like somebody had given me a new brain, it was really strange, nothing made sense, I didn’t feel like me," she recounted, describing the profound sense of disorientation and detachment from her former self. The journey back to basic cognitive abilities and speech was a testament to her resilience.
The biopsy results, however, brought a nuanced, albeit still challenging, diagnosis. It was confirmed that Lauren had a grade two oligodendroglioma, a rare type of incurable brain tumour. While still fast-growing, a grade two classification indicates a slower progression compared to the more aggressive glioblastoma initially suspected, offering a more extended prognosis of 10 to 12 years. Oligodendrogliomas are often characterised by specific genetic mutations, particularly in the IDH1 or IDH2 genes, making them potentially responsive to targeted therapies. It was through connecting with others on an Instagram page she started – a platform for raising awareness and documenting her journey – that Lauren discovered vorasidenib. This innovative treatment is a less aggressive option for patients not requiring immediate chemotherapy or radiotherapy post-surgery. As an IDH inhibitor, vorasidenib targets the specific mutations common in oligodendrogliomas, aiming to slow the tumour’s progression and potentially delay the need for more intensive treatments, thereby improving quality of life for a longer period.

Despite its promise, vorasidenib’s availability is uneven across the UK. The treatment has been approved by the Scottish Medicines Consortium for use in NHS Scotland, but this is not the case in Wales, England, or Northern Ireland. Lauren has become a passionate advocate, campaigning tirelessly to change this disparity. The Welsh government clarified its position, stating it relies on the independent advice of the National Institute for Health and Care Excellence (NICE) to ensure that the cost of treatments made routinely available to patients is "in balance with their benefits." They added that "While trial evidence shows it can slow cancer progression, there is no clear evidence it helps people live longer." NICE has provisionally recommended against vorasidenib’s availability on the NHS, with final guidance expected later this year. This highlights a critical tension in modern healthcare: the often-complex balance between scientific evidence, clinical benefit (such as delaying progression and preserving quality of life), and economic considerations in approving new, often expensive, treatments.
Facing the future with a terminal diagnosis requires immense courage and a proactive spirit. Lauren will undergo regular scans every three months to monitor the remaining tumour. Before commencing her vorasidenib treatment, which she is currently accessing privately, she is also undergoing fertility treatment, a poignant testament to her enduring hope for a future, despite the profound uncertainty. Her optimism is rooted in the rapid advancements in medical science: "Medicine is excelling at a rate it has never done before, AI is taking over as we know, so I’m really hopeful on that front." This perspective allows her to envision a future where new therapies might emerge, extending her life beyond current expectations.
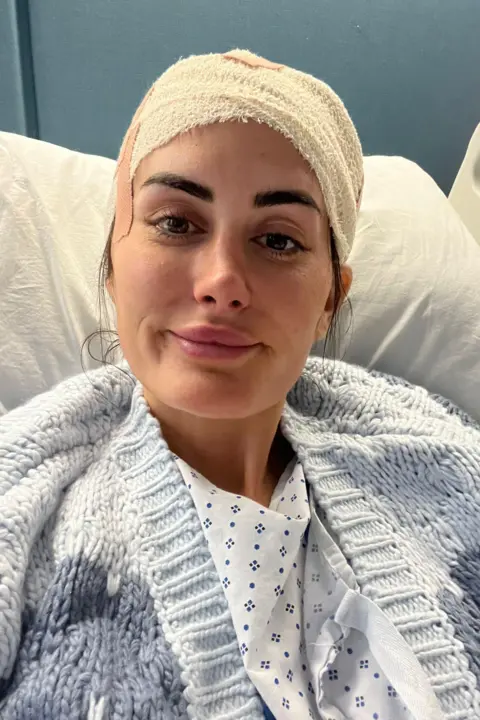
However, the emotional toll of a terminal diagnosis extends far beyond the individual, deeply impacting family and loved ones. Lauren candidly shared the immense burden this has placed on her family. "The whole thing has been hard for me… but for family, it’s almost been harder for them," she admitted. The profound pain of seeing their loved one face such a challenge, coupled with the helplessness, often leads to an unbearable wish: "I think everyone always says ‘I wish it was me, not you’ but I could really see it with them, constantly the pain in their eyes, because they wanted it to be them not me." In a beautiful display of unwavering commitment and hope amidst this adversity, Zak proposed to Lauren at her favourite beach in her hometown of Swansea just weeks after her diagnosis, a powerful symbol of their enduring love and shared future, however uncertain.
Lauren’s journey casts a harsh light on broader systemic issues within cancer care and research. Brain tumours remain the leading cause of cancer death in people under 40 in Wales, a statistic that underscores the severity and prevalence of these conditions. Despite this, Brain Tumour Research, a leading charity, reports that the disease has received a disproportionately low share of funding, accounting for just 1% of UK cancer research spending since 2002. This significant underinvestment profoundly impacts diagnostic advancements, treatment development, and ultimately, patient outcomes. Lauren Macpherson’s accidental diagnosis and subsequent advocacy serve as a powerful narrative, urging for greater awareness, increased research funding, and equitable access to life-extending treatments for all those facing the devastating reality of a brain tumour.
