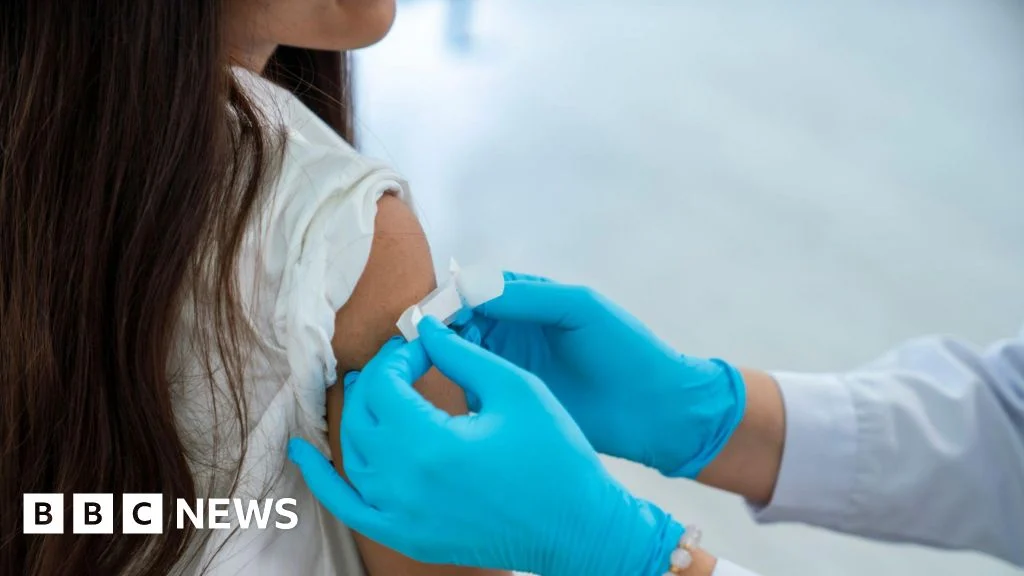
"Amidst a tragic meningitis outbreak claiming two young lives in Kent, health authorities are implementing urgent preventative measures, highlighting the critical importance of swift action and community vigilance against this rapidly progressing and potentially deadly infection."
A serious public health incident has emerged in Kent following the confirmed deaths of two young individuals from invasive meningococcal disease, prompting an immediate and extensive response from health authorities. The fatalities, involving a Year 13 pupil from Queen Elizabeth’s Grammar School in Faversham and a student from the University of Kent in Canterbury, underscore the severe and rapid nature of this bacterial infection. The UK Health Security Agency (UKHSA) has reported 13 suspected cases exhibiting symptoms of meningitis and septicaemia within a concentrated period, primarily across the Canterbury area, leading to a proactive distribution of antibiotics to potentially exposed individuals.
The tragic deaths, confirmed by a local Member of Parliament on Monday, have cast a sombre shadow over the academic communities in Kent. Both victims are believed to have been aged between 18 and 21, a demographic particularly susceptible to meningococcal disease due to close living conditions and social interactions common in schools and university environments. The rapid escalation of cases, with 13 individuals presenting with signs and symptoms of the dangerous infection between Friday and Sunday, triggered an urgent public health investigation and intervention.
Meningitis is an inflammation of the protective membranes (meninges) that surround the brain and spinal cord, while septicaemia refers to blood poisoning caused by the same bacteria. Both are life-threatening conditions that can develop very quickly. When the infection invades the bloodstream or brain linings, it is termed ‘invasive meningitis’ or invasive meningococcal disease (IMD), which is the most severe form of the illness and the focus of the current outbreak. This acute, severe infection demands immediate medical attention due to its potential for rapid deterioration and devastating consequences, including permanent disability or death, often within hours of symptom onset.
While the specific strain of meningococcal bacteria responsible for the current outbreak has yet to be definitively identified, public health officials are acting with extreme caution. Bacterial meningitis, which includes meningococcal disease, is significantly rarer but far more serious than its viral counterpart. It can lead to severe complications such as sepsis, permanent brain damage, hearing loss, and limb loss if not treated promptly with antibiotics.
Understanding the symptoms is paramount for early detection and intervention. Meningitis symptoms can develop suddenly and may initially mimic less serious illnesses like the flu or a bad cold, which makes timely diagnosis challenging, especially for young adults. Key symptoms of meningitis often include a sudden high fever, severe headache, stiff neck, dislike of bright lights (photophobia), drowsiness or altered consciousness, and vomiting. Babies and young children may also display unusual crying, floppy limbs, a bulging soft spot on their head, and poor feeding.
Septicaemia, which frequently accompanies meningitis, is characterized by symptoms such as cold hands and feet, pale or mottled skin, limb pain, and rapid breathing. A distinctive symptom of septicaemia is a rash that does not fade when a glass is rolled over it (a non-blanching rash). This rash, which can appear as small red or brown pinpricks, or larger blotches, is a critical indicator of severe blood poisoning and necessitates immediate emergency medical care. It is crucial to remember that a rash may not always be present or may be one of the last symptoms to appear, so waiting for it could delay lifesaving treatment.
The transmission of meningococcal bacteria typically occurs through close, prolonged contact with an infected person’s respiratory or throat secretions. This includes activities such as coughing, sneezing, deep kissing, or sharing eating utensils, drinks, or cigarettes. Many people can carry the bacteria in their nose or throat without becoming ill, acting as asymptomatic carriers who can still spread the infection to others. This characteristic makes controlling outbreaks particularly challenging in communal settings.
The current outbreak in Kent is believed to be linked to a social event in Canterbury, which some of those who fell ill reportedly attended. University campuses and other environments where young people live and socialize closely, such as schools and military barracks, are recognized as settings where meningococcal disease can spread more easily. Although outbreaks of meningococcal disease are rare, the close proximity and frequent social interaction in these settings increase the risk of transmission among individuals who may not be fully vaccinated or have waning immunity.
In response to the identified cases and the potential for wider spread, health experts are swiftly arranging for individuals identified as close contacts to receive prophylactic antibiotics. This preventative measure is designed to eliminate any meningococcal bacteria that these individuals may be carrying in their nose or throat, thereby preventing them from developing the disease themselves or transmitting it to others. This strategy is a cornerstone of public health management during outbreaks of highly transmissible bacterial infections, even before the specific strain has been confirmed.
Vaccination plays a crucial role in preventing meningococcal disease. The UK’s national immunization programme includes several vaccines that offer protection against different types of bacteria that cause meningitis. The MenACWY vaccine, typically offered to teenagers around 14 years old, protects against meningococcal groups A, C, W, and Y. For babies, the MenB vaccine is recommended at eight weeks, followed by a second dose at 12 weeks, and a booster at one year, providing protection against meningococcal group B, which is a common cause of meningitis in young children.
Other routine vaccinations also contribute indirectly to meningitis prevention. The six-in-one vaccine (DTaP/IPV/Hib/Hep B), given to infants, protects against Haemophilus influenzae type b (Hib), a bacterium that can also cause meningitis. The pneumococcal vaccine, administered to babies, offers protection against serious infections caused by pneumococcal bacteria, including pneumococcal meningitis. Furthermore, the MMR vaccine, which protects against measles, mumps, and rubella, is important because meningitis can sometimes occur as a complication of these viral infections. For young adults, particularly those starting university, ensuring up-to-date MenACWY vaccination is strongly advised due to their increased risk.
The advice from health officials to students and the wider community in the affected areas of Canterbury and Faversham is unequivocal: trust your instincts. Anyone experiencing symptoms of meningitis or septicaemia should seek immediate medical help by calling 999 or attending the nearest Accident and Emergency Department. Early treatment is absolutely lifesaving, and delays can have catastrophic consequences. It is vital not to wait for all symptoms to appear, nor to delay seeking help specifically for a rash, as this may be a late sign of severe illness.
Health officials have specifically warned students that early warning signs of meningitis can be easily confused with common illnesses like a severe cold, flu, or even a hangover. This misinterpretation can be particularly dangerous, leading to critical delays in seeking medical attention. Students are strongly urged to check on friends who go to bed feeling unwell and to not hesitate to contact their GP or the NHS 111 service for advice if they have concerns. Public health teams are working tirelessly to contain the outbreak, identify contacts, and ensure that all necessary preventative measures are in place to protect the community. The focus remains on rapid response, comprehensive treatment, and heightened public awareness to mitigate further spread and prevent additional tragedies.