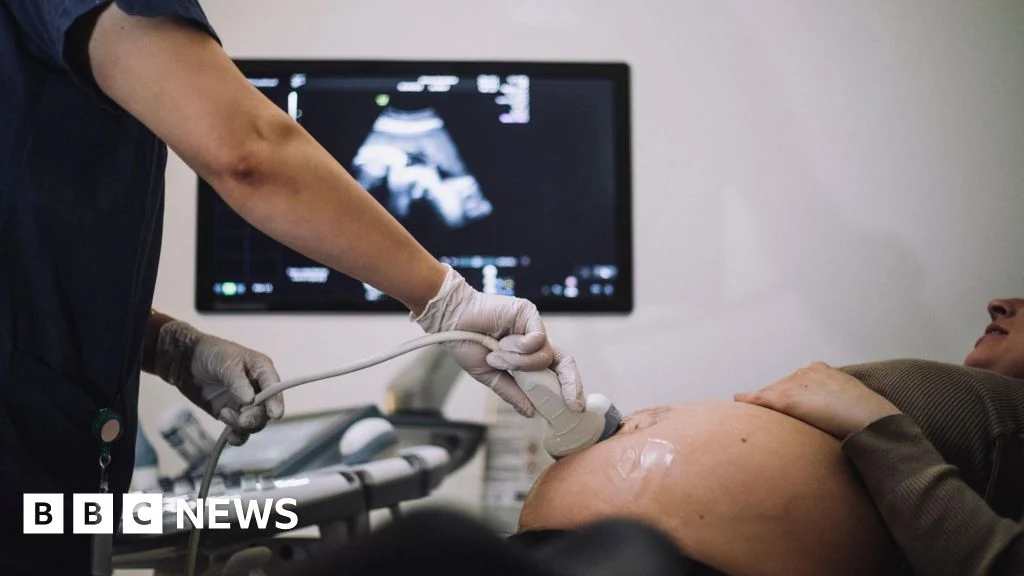
"At least 58 babies at Oxford University Hospitals Trust might have survived with better care, exposing a deeply concerning pattern of missed chances, alleged arrogance among senior doctors, and a ‘defensive culture’ that has left bereaved families fighting for answers and accountability."
This harrowing revelation from a BBC investigation casts a stark light on the state of maternity services at Oxford University Hospitals Trust (OUH), a major NHS provider. The period between 2019 and 2024 saw a tragic toll of 32 stillbirths and 26 neonatal deaths where improved medical intervention could have potentially altered the outcome. These findings echo a national crisis in maternity care, with families recounting devastating experiences marked by systemic failures and a perceived reluctance by the institution to fully acknowledge shortcomings, compelling calls for a comprehensive independent inquiry into the trust’s practices.
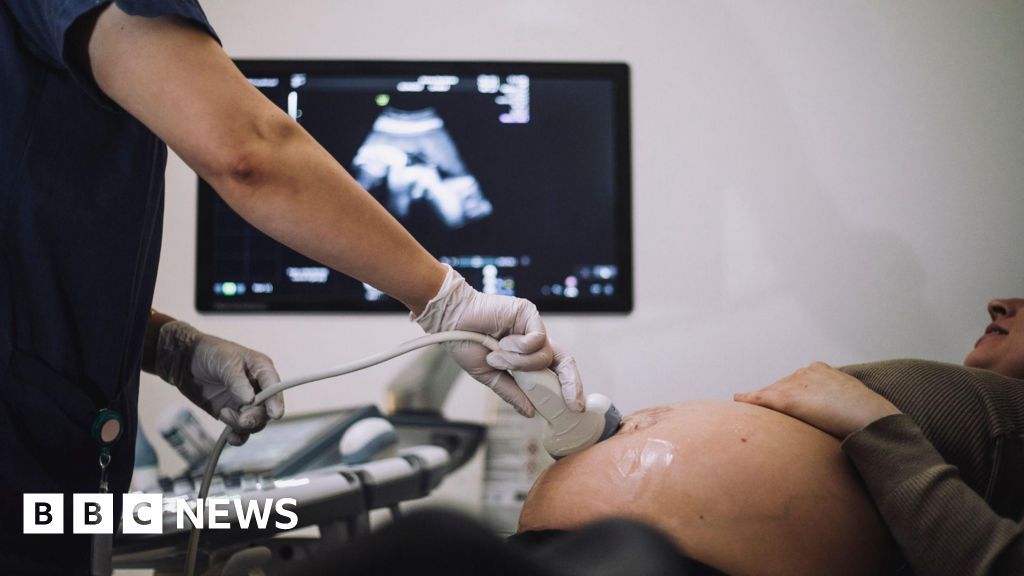
The BBC investigation, drawing on a Freedom of Information request, has unveiled a deeply troubling pattern within the maternity unit of Oxford University Hospitals Trust (OUH). Between 2019 and 2024, a total of 58 infant deaths – comprising 32 stillbirths and 26 neonatal deaths, occurring within 28 days of birth – were identified where a different course of care might or was likely to have led to a different outcome. This significant figure underscores severe concerns regarding the quality and safety of maternity services at the trust, which has long been a key provider of specialist and tertiary care across the region, handling some of the most complex cases. These revelations contribute to a growing national narrative of distress and systemic issues within NHS maternity departments, previously highlighted by high-profile inquiries into other trusts like Shrewsbury and Telford, East Kent, and Morecambe Bay, indicating a wider systemic challenge within the UK’s healthcare system.
For the families directly impacted, these statistics represent profound personal tragedies, often compounded by a desperate search for answers and a sense of injustice. Bereaved and harmed mothers have consistently pointed to critical "missed chances," an "arrogance" perceived among certain senior medical staff, and a pervasive "defensive culture" within the institution. "Missed chances" often manifest as failures to adequately monitor fetal well-being, misinterpretation of cardiotocography (CTG) readings – which monitor fetal heart rate and uterine contractions – or delayed intervention in critical situations. A "defensive culture," as described by families and legal professionals, suggests a lack of transparency, an institutional resistance to admitting errors, and a priority placed on protecting reputation over fostering an open learning environment. This posture can stifle crucial lessons from adverse events and alienate those who seek truth and accountability. In response, OUH acknowledged the figures, stating they include complex cases referred from across the region, and expressed regret that some mothers felt let down. The Trust affirmed its commitment to detailed reviews of every baby death to understand contributing factors and identify necessary improvements.
The deeply personal accounts of affected families bring the statistics into sharp focus. Eleanor Taylor-Verlaan, from Faringdon, Oxfordshire, is one such mother, whose life was irrevocably altered by the loss of her first daughter, Alissa, in 2017. Eleanor is due to have a Caesarean section next month, an experience profoundly shadowed by the impending anniversary of Alissa’s death. Alissa suffered severe brain damage due to oxygen deprivation, caused by a placental abruption – a life-threatening condition where the placenta prematurely separates from the uterine wall, leading to a sudden loss of oxygen and nutrients to the baby. Eleanor firmly believes that timely and appropriate medical intervention could have saved her daughter. She recounts being classified as high-risk following her 20-week scan, which indicated a heightened susceptibility to complications such as growth restriction, pre-eclampsia (a pregnancy complication characterized by high blood pressure), and stillbirth. Despite this, she argues, she was not adequately monitored throughout her pregnancy, a critical oversight for a high-risk patient.
At 35 weeks, Eleanor experienced alarming symptoms, including abdominal pains and sickness, yet was advised by healthcare professionals to remain at home and take paracetamol. This advice proved critical. On February 20, 2017, after enduring a wait of over two hours in the maternity assessment unit, an emergency C-section was performed. Baby Alissa was delivered in a critical condition and tragically passed away six weeks later. An internal review conducted by OUH identified some issues in the care provided but concluded that these were unlikely to have "improved the outcome for this baby." Eleanor, overwhelmed by grief at the time, did not know how to challenge these findings but is now pursuing an independent investigation with the assistance of birth injury lawyers. Laura Cook, a partner at Medilaw, criticizes such internal reviews as often being mere "tick-box exercises" designed to absolve the institution and avoid admitting fault. She argues this approach prolongs the suffering of grieving families by denying them genuine answers and forces them into protracted legal battles. Cook specifically highlights Oxford’s perceived "defensiveness," noting that "reputation is of the utmost importance," a stance she suggests differs from other trusts she has encountered, where there might be more openness to acknowledging mistakes. The trust reiterated its acknowledgment of families’ dissatisfaction and its commitment to learning from feedback.

Another heartbreaking case is that of Alice Topping, whose daughter Smokey was stillborn at the John Radcliffe Hospital in Oxford in September 2023. Like Eleanor, Alice had been identified as high-risk at her 20-week scan. Her midwife, concerned about the baby’s growth, referred her for an additional scan at 40 weeks, a crucial assessment often performed to monitor fetal development and detect potential issues that could impact delivery. However, Alice was never contacted to arrange this vital appointment. Driven by mounting anxiety, she made an astounding 44 calls in a single day, attempting to book the scan herself. Her persistent requests, she states, were ultimately denied by a consultant who informed her that the trust prioritised 36-week scans instead. Just one week later, her worst fears were realised as Smokey died during labour.
Alice’s experience echoes the frustrations voiced by Eleanor regarding the investigative process. An initial internal review by OUH concluded that no wrongdoing had occurred. However, a subsequent independent investigation painted a starkly different picture, uncovering a "catalogue of failings" and issuing five safety recommendations that, critically, "could have made a difference to the outcome." This stark contrast between internal and independent findings highlights the urgent need for unbiased scrutiny in such sensitive cases. Alice expressed profound anguish, stating, "At the most vulnerable time in my entire life I was failed… it’s just horrific knowing that with just basic care my daughter should be here, that’s not acceptable." She believes vital information regarding her pregnancy risks was withheld from her, underscoring a deep-seated demand for "answers, truth and change" from bereaved and harmed families.
The trust’s stillbirth rates provide further context to these individual tragedies. In 2023, the year Alice lost her daughter, Oxford University Hospitals Trust recorded the highest stillbirth rate among 25 specialist trusts that cater to the most critically ill babies. This statistic is particularly concerning given OUH’s role as a major referral center. While the latest figures from MBRRACE-UK – the national body monitoring maternal and infant deaths – show a slight decrease in OUH’s stillbirth rate to 3.47 per 1,000 births in 2024, bringing it in line with comparable trusts, and its overall mortality rates falling below average, the past performance raises serious questions about historical shortcomings. It is important to note that OUH handles over 7,000 births annually, with the vast majority proceeding safely and many women reporting positive experiences. However, the sheer volume of births also means that even small percentages of avoidable harm can translate into significant numbers of affected families. Furthermore, the trust notes that its claims-per-birth rate is among the lowest compared to similar trusts, and compensation figures often relate to incidents from many years earlier and can be skewed by one or two high-value cases involving life-long care needs. Between 2019 and 2024, OUH carried out 361 internal reviews into baby deaths, known as Perinatal Mortality Review Tools (PMRTs), with at least 58 cases graded C or D, indicating that different care either "may" have or was "likely" to have made a difference to the outcome.
The external scrutiny of OUH’s maternity services intensified in 2021 when the health watchdog, the Care Quality Commission (CQC), inspected the main maternity unit at the John Radcliffe Hospital. This inspection was prompted by five whistleblowers who raised serious concerns about a culture of bullying and dysfunctional team dynamics. Consequently, the CQC downgraded the unit’s rating from "Good" to "Requires Improvement," signaling a need for significant change in leadership, processes, and patient safety. Since then, NHS England has provided targeted maternity support to OUH, focusing on areas such as timely induction of labour decision-making and strengthening management oversight to enhance safety and quality of care. This support is scheduled to continue until June. A subsequent CQC inspection in October 2025 saw the watchdog issue a formal warning notice on December 8, 2025, citing five breaches of legal regulations pertaining to safe care and treatment, premises and equipment, good governance, and staffing. This is a severe step, as the CQC has the power to prosecute trusts for serious failures in care, a power it has exercised only five times since its inception in 2015, highlighting the gravity of the identified shortcomings.

The mounting evidence and the persistent concerns from families and legal professionals have fueled a campaign by hundreds of individuals calling for a judge-led public inquiry into OUH’s maternity services. Such inquiries are comprehensive, independent investigations designed to uncover systemic issues, assign accountability, and recommend far-reaching changes that extend beyond the scope of internal reviews. While Health Secretary Wes Streeting has authorised similar independent reviews for hospital trusts in Leeds and Sussex, no such investigation has yet been commissioned for Oxford. Michelle Welsh MP, who chairs the All Party Parliamentary Group on Maternity, passionately argues for this change, stating, "There is a systematic toxic culture there that needs tackling and families deserve accountability and answers." The psychological toll on families, repeatedly told that nothing could have been done, is immense, and a public inquiry offers the promise of a full, transparent reckoning. A spokesperson for the Department for Health and Social Care acknowledged the national efforts, mentioning Baroness Amos’s role in setting out clear steps to improve maternity and neonatal care across England and reiterating NHS England’s rapid, targeted support for OUH, designed to bring together hospital leaders and national experts to ensure progress.
Responding directly to the BBC’s investigation, Simon Crowther, the interim chief executive for OUH, expressed deep regret, acknowledging the "tragic" nature of the stories shared and the profound, lasting impact of losing a child. He specifically addressed Eleanor Taylor-Verlaan’s case, stating the trust’s willingness to re-examine it and urging her to contact them directly. Regarding Alice Topping’s case, Mr. Crowther noted its complexity and confirmed it had been scrutinized by multiple independent bodies. He concluded by affirming the trust’s unwavering commitment to "learning from every family’s experience and to continually improving the safety and quality of maternity care." While these assurances are offered, the calls for a broader, independent inquiry highlight the persistent demand from affected families and campaigners for greater transparency and systemic reform to prevent future tragedies, ensuring that lessons learned translate into tangible, lasting improvements across all maternity services.